Adhesions after a cesarean section
back to main page
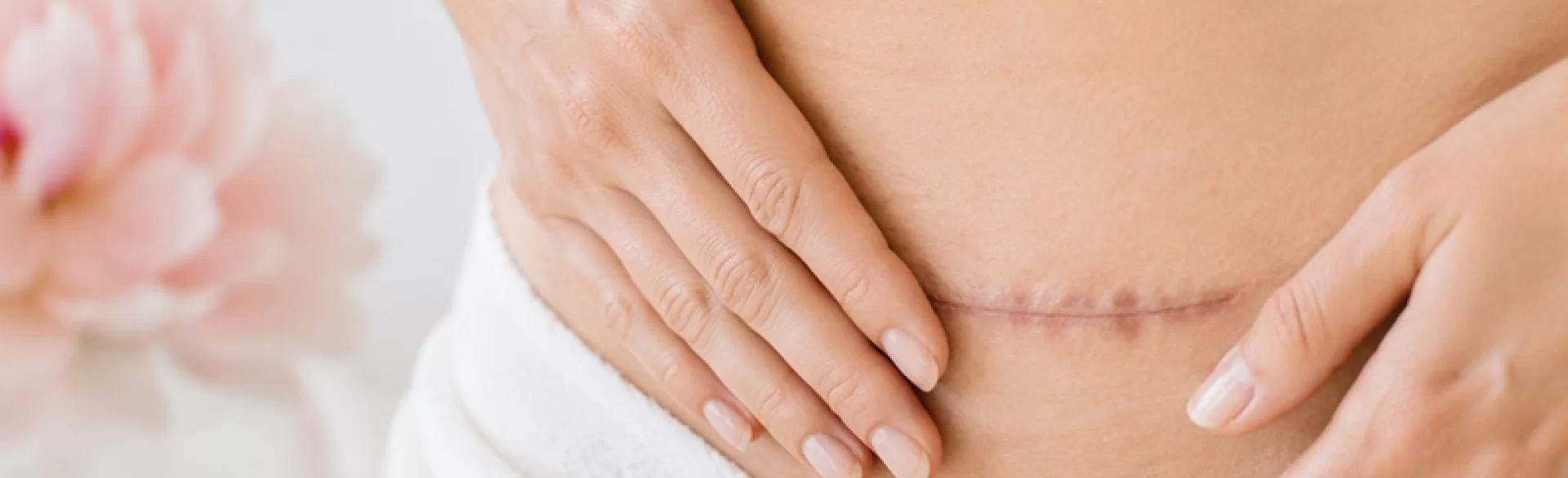
Adhesions after a cesarean section are pathological tissue connections that form between organs of the abdominal cavity or between organs and the body wall as a result of the healing process after surgery. They are the result of excessive activity of the body's repair processes, in which fibrin is deposited and connective tissue is remodeled. Adhesions can involve various structures, including the uterus, bladder, intestines and fascia, leading to restriction of their physiological mobility. Although they often remain asymptomatic, in some patients they are a cause of chronic pain, functional disorders and surgical complications.
Adhesions after a cesarean section - how they form
The process of adhesion formation is directly related to the inflammatory response and tissue healing after surgical intervention. During a cesarean section the continuity of the abdominal wall and organs is disrupted, which initiates a cascade of reparative processes.
In the first phase of healing the following occur:
- release of inflammatory mediators (cytokines, prostaglandins),
- deposition of fibrin, which forms a temporary "matrix" for regenerating tissues,
- influx of inflammatory cells and fibroblasts.
Under physiological conditions fibrin undergoes gradual degradation due to the activity of the fibrinolytic system. However, if the balance between synthesis and degradation is disturbed (e.g., as a result of tissue ischemia, infection, excessive surgical manipulation), fibrous connections may become persistent.
Factors that increase the risk of adhesion formation:
- the extent of the surgical procedure,
- postoperative complications (e.g., infections),
- presence of a hematoma or exudate,
- individual predisposition to excessive fibrosis,
- repeat cesarean sections.
Adhesions can form both within the abdominal cavity (visceral adhesions) and within the layers of the abdominal wall (fascial adhesions), affecting the biomechanics of the entire body.
Adhesions after a cesarean section vs. scar - differences
Although the terms „adhesion” and „scar” are sometimes used interchangeably, they refer to different anatomical structures and biological processes.
Scar:
- is the visible result of skin healing,
- forms at the site of tissue incision,
- involves mainly the epidermis, dermis and subcutaneous tissue,
- can be assessed visually and by palpation.
Adhesions:
- form deeper, between organs or layers of tissue,
- are not visible from the outside,
- may involve fascia, muscles, the peritoneum and internal organs,
- affect the mobility and function of structures.
The key difference is therefore location and functional impact. A scar may be an aesthetic or superficial problem, whereas adhesions affect organ systems and the body’s biomechanics.
In clinical practice the two phenomena often coexist. An improperly healed scar (e.g., with limited mobility) may be an indicator of the presence of adhesions in deeper tissue layers.
Adhesions after a cesarean section - symptoms
The clinical presentation of adhesions is varied and depends on their location, extent, and the degree of tissue tension. In many patients adhesions remain asymptomatic, but in some cases they lead to significant complaints.
The most commonly observed symptoms include:
- chronic pain in the lower abdomen or around the scar,
- a sensation of pulling, tension, or "stiffness" of the tissues,
- limited mobility of the abdominal wall,
- pain during physical activity,
- bowel function disturbances (e.g., bloating, constipation),
- pain during intercourse (dyspareunia).
In more advanced cases adhesions can lead to:
- infertility (by disrupting the anatomy of the reproductive organs),
- intestinal obstruction (rare, but a potentially serious complication),
- chronic pelvic pain syndromes.
An important aspect is the impact of adhesions on the fascial system – they can alter the distribution of tensions in the body, leading to distant complaints, e.g., low back pain or postural disorders.
Adhesions after a cesarean section - when to see a specialist
Specialist consultation is indicated in cases of persistent symptoms suggesting the presence of adhesions or abnormal tissue healing after surgery. Particular attention should be paid to chronic pain and functional impairments.
Indications for diagnosis and therapy include:
- pain persisting for more than 3–6 months after surgery,
- restriction of scar mobility,
- a sensation of pulling during movement or changes in position,
- unexplained bowel problems,
- painful intercourse,
- difficulty becoming pregnant.
Therapeutic management is multifaceted and may include:
- urogynecological physiotherapy (manual therapy, mobilization of the scar and fascia),
- osteopathic techniques to restore tissue mobility,
- visceral therapy (affecting the abdominal organs),
- in selected cases, surgical treatment (adhesiolysis).
In the context of aesthetic and regenerative medicine, procedures that support scar and tissue quality are also used, such as:
- fractional laser therapy,
- microneedle radiofrequency,
- procedures stimulating collagen remodeling.
Early therapeutic intervention allows limiting the progression of changes and restoring normal tissue function, which is important both for the patient's quality of life and overall health.