Allergic pustules
back to main page
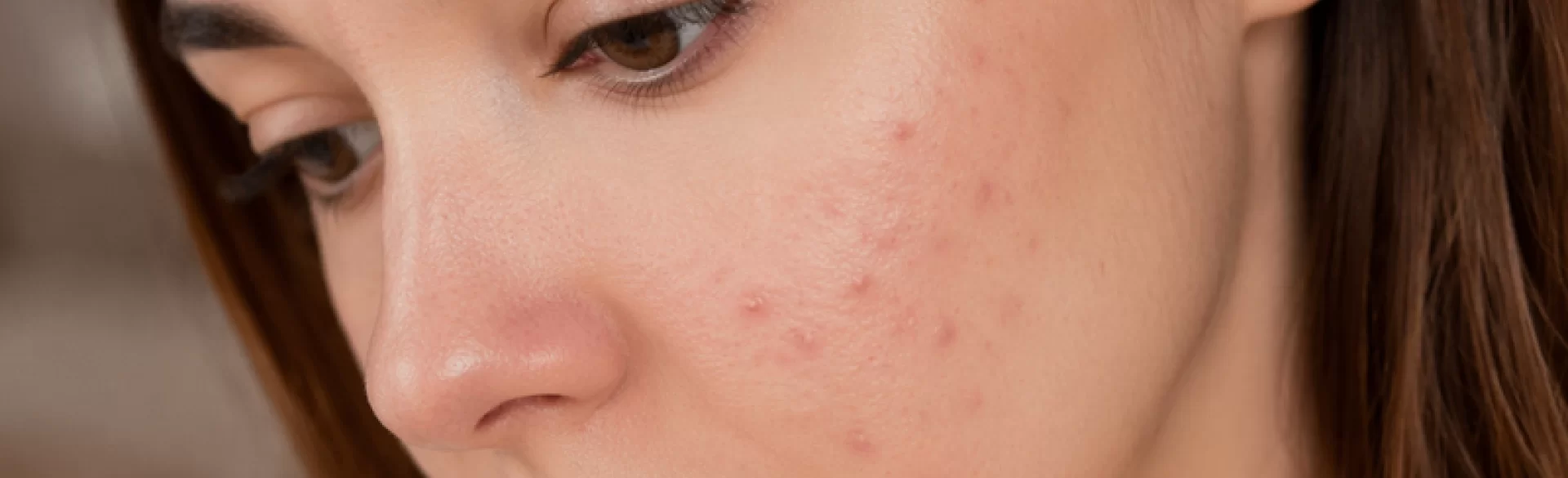
Allergic pustules are inflammatory skin lesions resulting from a hypersensitivity reaction of the immune system to specific allergens. They can take the form of papules, vesicles, or pustules, often coexisting with erythema and pruritus. The mechanism of their formation is linked to the activation of immune system cells, including mast cells and T lymphocytes, leading to the release of inflammatory mediators such as histamine. These lesions occur in the course of contact allergy, atopic dermatitis, or drug reactions. Allergic pustules are not a separate disease entity, but a clinical symptom requiring the identification of the cause.
Allergic pustules – what they look like
The morphology of allergic pustules is diverse and depends on the mechanism of the immune reaction and its duration. Most commonly observed are:
- papules – raised, small lesions with a diameter of several millimeters,
- vesicles – filled with serous fluid,
- pustules – lesions containing purulent content, although not always of bacterial etiology,
- erythema – redness of the skin resulting from vasodilation,
- edema – especially in acute reactions.
A characteristic feature is intense itching, which leads to scratching and secondary epidermal damage (excoriations), increasing the risk of bacterial superinfection. In chronic forms, lichenification may occur, which is the thickening of the skin with accentuation of its markings.
Unlike infectious lesions, allergic pustules usually appear suddenly, often symmetrically, and may subside after the elimination of the triggering factor. However, their clinical presentation can mimic other dermatoses, therefore differential diagnosis (e.g., with acne, folliculitis, or pustular psoriasis) is crucial.
Allergic pustules – location
The location of allergic skin lesions depends primarily on the route of contact with the allergen and the type of immune reaction. The most common locations are:
- face – especially in contact allergies (cosmetics, skincare ingredients),
- neck and cleavage – reactions to perfumes, detergents, metals,
- hands – contact with occupational allergens or chemicals,
- elbow and knee creases – typical for atopic dermatitis,
- back and chest – drug-induced or systemic reactions,
- abdomen and hip area – e.g. nickel allergy (buttons, buckles).
In contact allergy, lesions are usually limited to the site of exposure. In systemic reactions (e.g. after allergen ingestion or in a drug-induced reaction), they may be generalized.
The symmetry of lesions – often observed in allergies – and their recurrent nature in case of re-exposure to the sensitizing agent also have significant diagnostic importance.
What for allergic bumps
Therapeutic management in the case of allergic pustules should be causal and symptomatic, based on the identification and elimination of the allergen. Key strategies include:
1. Elimination of the sensitizing factor
- avoiding contact with allergens (e.g., cosmetics, detergents, metals),
- dietary modification in the case of food allergy,
- changing medications in drug-induced reactions.
2. Pharmacological treatment
- antihistamines – reduction of pruritus and inflammatory reaction,
- topical glucocorticosteroids – anti-inflammatory and immunosuppressive action,
- calcineurin inhibitors (tacrolimus, pimecrolimus) – especially in chronic treatment,
- in severe cases: systemic corticosteroids or immunosuppressive treatment.
3. Skin care
- using emollients that restore the hydrolipid barrier,
- avoiding irritants (SLS, alcohol, intense fragrances),
- gentle skin cleansing.
4. Supportive methods in aesthetic medicine and dermatology
In chronic or recurrent cases, when the skin barrier is damaged, supportive therapies are used:
- regenerative mesotherapy – improvement of hydration and skin restoration,
- LED light therapies – anti-inflammatory and regenerative action,
- medical peels with a soothing effect – regulation of epidermal renewal,
- radiofrequency treatments – supporting tissue regeneration.
5. Specialist diagnostics
In the case of recurrent lesions, it is advisable to perform:
- patch tests (contact allergy),
- skin prick tests,
- determination of specific IgE.
It should be emphasized that symptomatic treatment without identifying the cause often leads only to short-term improvement. Effective therapy requires an interdisciplinary approach and conscious elimination of factors triggering the allergic reaction.