Boils under the armpits
back to main page
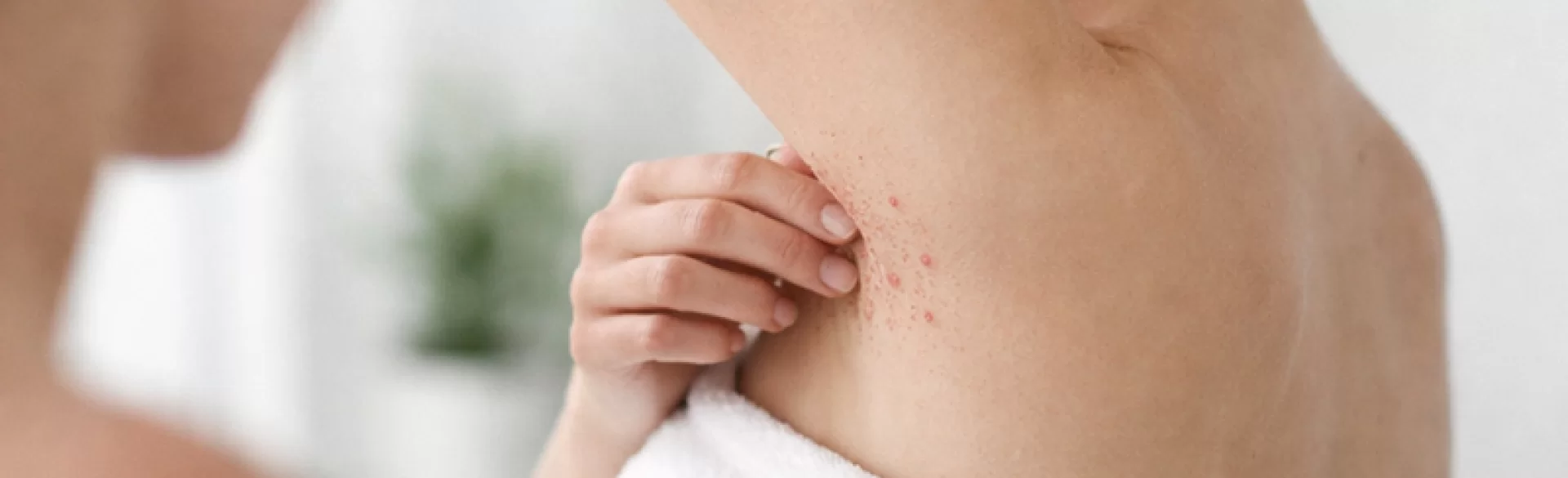
Pimples under the armpits are a common dermatological issue characterized by inflammatory, papular, pustular, or nodular changes located in the axillary regions. This area is part of the so-called intertriginous zones - warm, moist areas rich in sweat glands (particularly apocrine glands) and hair follicles. Due to constant friction, hair removal, and the presence of bacterial and fungal microflora, the skin of the armpits is particularly susceptible to infections, irritations, and chronic inflammatory dermatoses. Depending on the etiology, the pimples can be mild and transient (e.g., folliculitis) or may indicate a chronic condition, such as hidradenitis suppurativa (acne inversa).
Armpit Bumps – Causes
The etiology of skin changes under the arms is multifactorial. The most common causes include:
1. Folliculitis
- bacterial infection, most commonly Staphylococcus aureus,
- micro-injuries from shaving or depilation,
- ingrown hairs,
- excessive sweating and skin occlusion.
2. Hidradenitis suppurativa
- chronic, recurrent inflammatory disease of the apocrine glands,
- formation of painful nodules, abscesses, and fistulas,
- strong association with obesity and smoking,
- autoinflammatory and immunological component.
3. Contact dermatitis
- allergic or irritant reaction to deodorants, antiperspirants, cosmetics,
- erythema, itching, small pustules.
4. Fungal infections (e.g., cutaneous candidiasis)
- moist environment conducive to the growth of Candida albicans,
- redness, maceration, small satellite pustules.
5. Hormonal and metabolic factors
- insulin resistance,
- androgenic disorders,
- genetic predispositions.
Armpit pimples – types
Changes under the armpits can present in various clinical forms:
- hard, painful protrusions,
- often associated with inflammation of the hair follicle.
- filled with purulent content,
- can rupture and form crusts.
- deep, painful changes,
- typical of hidradenitis suppurativa,
- can leave scars.
- small, itchy bumps,
- often accompanied by redness and burning.
Epidermoid Cysts
- slow-growing, movable lumps,
- may become secondarily infected.
Differential diagnosis should also take into account systemic diseases, such as diabetes, which predisposes to recurrent skin infections.
Underarm Pimples – Home Remedies
In the case of mild, single lesions, conservative management can be implemented:
- gentle cleansing agents with physiological pH,
- thorough drying of the armpits after bathing,
- avoiding occlusion (tight synthetic clothing).
- a break from shaving until the lesions heal,
- use of new, sharp blades,
- skin disinfection after depilation.
- ointments with ichthyol (anti-inflammatory effect),
- zinc preparations,
- compresses with saline solution.
- elimination of irritating antiperspirants,
- choosing hypoallergenic products.
It should be emphasized that home methods should not be used in the case of painful, recurring nodules, extensive abscesses, or general symptoms (fever, enlarged lymph nodes).
Armpit pimples – treatment
Treatment depends on the cause and the extent of the changes.
Pharmacological Treatment
- Topical antibiotics (e.g., clindamycin),
- Systemic antibiotics for extensive infections,
- Anti-inflammatory and immunomodulating drugs for hidradenitis suppurativa,
- Antifungal agents for confirmed fungal infections.
- Incision and drainage of abscesses,
- Removal of cysts,
- Laser closure of fistulas in the course of hidradenitis suppurativa.
- Weight reduction,
- Smoking cessation,
- Treatment of hormonal disorders.
In the context of aesthetic medicine and procedural dermatology, in the case of changes associated with excessive sweating or chronic folliculitis, the following are used:
- Laser hair removal (e.g., Thunder MT) – reducing hair follicles decreases the risk of inflammation recurrence,
- Antiperspirant therapies using botulinum toxin – reducing excessive sweating,
- Anti-inflammatory and regenerative laser treatments.
Proper dermatological diagnosis is crucial. Recurrent, painful changes under the arms require specialist consultation, as they may be an early sign of hidradenitis suppurativa – a chronic, progressive disease requiring long-term treatment.