Burn scars
back to main page
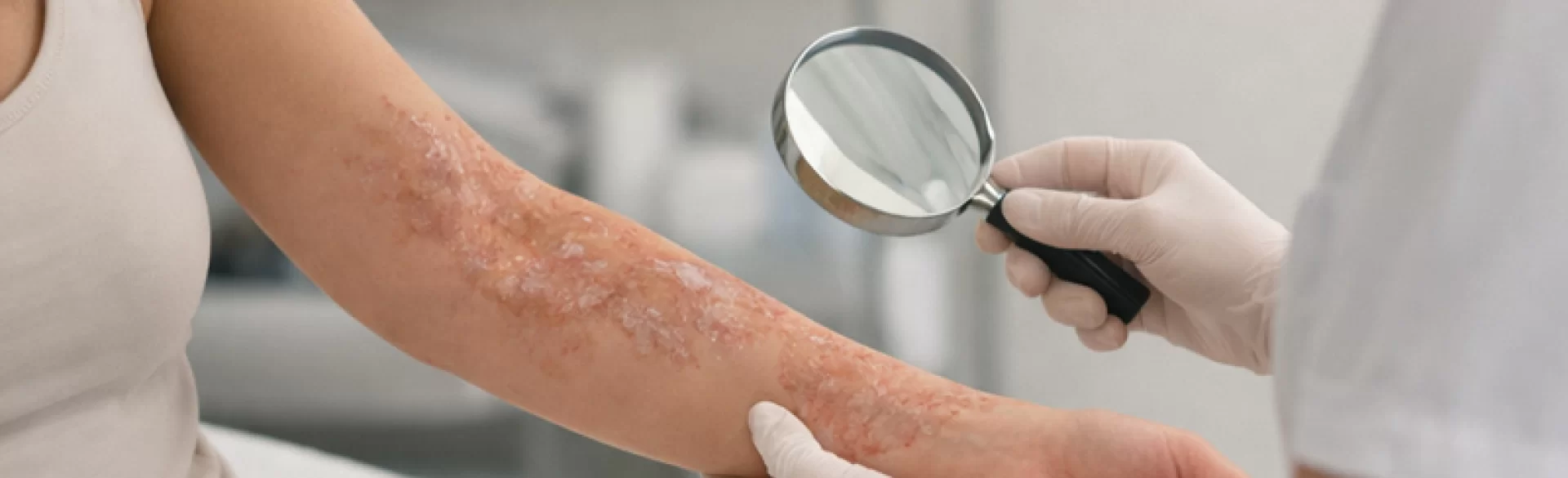
Burn scars are permanent consequences of damage to the skin and deeper tissues resulting from exposure to high temperatures, chemicals, electricity, or radiation. Their formation is a result of a disrupted wound healing process, which includes the inflammatory, proliferative, and extracellular matrix remodeling phases. Burns penetrating the dermis lead to abnormal synthesis of type I and III collagen, excessive fibroblast activity, and impaired angiogenesis. As a result, scar changes of varying severity develop, ranging from normotrophic to hypertrophic and contracture scars. Burn scars have not only aesthetic but also functional significance, as they can limit mobility, cause chronic itching, pain, and lead to anatomical deformities.
Burn scars – what they look like
The clinical appearance of a burn scar is directly related to the depth of the injury and the time it takes to heal. First-degree burns usually do not leave permanent marks, whereas deep second-degree and third-degree burns lead to the formation of permanent scar tissue.
In the first few months after the wound has healed, the scar:
- has an intensely red or purple coloration (increased angiogenesis),
- is hard and elevated,
- exhibits increased sensitivity to touch,
- is often accompanied by itching (a result of hyperreactivity of nerve endings).
In histological examination, one observes:
- disorganization of collagen fibers,
- increased density of fibroblasts,
- predominance of type III collagen in the early phase,
- reduced amount of elastin.
During the maturation period (6–24 months), there is partial reorganization of collagen, a decrease in vascularization, and a reduction in the volume of the scar. This process, however, is incomplete in cases of pathological scars.
A characteristic feature of burn scars is the absence of skin appendages (hair follicles, sebaceous, and sweat glands), which leads to:
- dryness,
- tendency to microcracks,
- reduced resistance to mechanical injuries.
Burn scars – types
The classification of burn scars includes several clinical types:
1. Normotrophic scars
These develop after superficial burns. They are flat, elastic, and do not cause significant functional disturbances.
2. Hypertrophic scars
The most common pathological form. They are characterized by:
- elevation above the skin level,
- restriction to the boundaries of the original wound,
- intense erythema,
- itching and tenderness.
Risk factors:
- healing >21 days,
- infection,
- excessive skin tension,
- young patient age.
3. Keloids
Changes that extend beyond the boundaries of the original injury. They are less common in burns than after surgical procedures but may develop in individuals with a genetic predisposition. They are characterized by:
- uncontrolled proliferation of fibroblasts,
- excessive synthesis of type III collagen,
- tendency to recur after treatment.
4. Contracture scars
The most functionally problematic. They develop due to the shortening of scar tissue and fascial fibrosis. They lead to:
- limitation of the range of motion,
- deformities of the face, neck, hands,
- swallowing or speech disorders (depending on the location).
Burn scars – ointments
Topical therapy is most significant in the early phase when the remodeling process is still active. Its aim is to modulate fibroblast activity and regulate collagen synthesis.
Preparations with documented efficacy:
1. Silicones (gels, silicone sheets)
The mechanism of action includes:
- maintaining optimal hydration,
- reducing tension within the scar,
- regulating growth factors (including TGF-β).
They are considered the standard in hypertrophic scar prevention.
2. Topical corticosteroids
Used short-term in active scars. They inhibit fibroblast proliferation and collagen synthesis.
3. Preparations with heparin and allantoin
They support remodeling and have anti-inflammatory effects, though their efficacy is moderate.
4. Preparations with onion extract (Allium cepa)
They exhibit antiproliferative and anti-inflammatory effects.
It should be emphasized that in the case of mature, established scars, the effectiveness of ointments is limited. Pharmacological therapy should be part of a combined treatment approach.
Burn scars – home remedies
Home methods can serve only as supportive measures and do not replace specialized treatment.
Recommended actions:
- regular scar massage (improving flexibility, reducing adhesions),
- use of emollients,
- sun protection SPF 50+ for a minimum of 12 months,
- avoiding mechanical irritation.
In selected cases, the following are used:
- compression garments (compression therapy),
- molding pressure dressings.
It is not recommended to use unverified substances (alcohol, essential oils with irritating effects) that may lead to secondary inflammation and worsen the quality of the scar.
Contemporary aesthetic medicine and plastic surgery offer methods that enable the remodeling of scar tissue through controlled stimulation of neocollagenesis.
1. Fractional ablative and non-ablative lasers
Mechanism:
- ablative microcolumnar coagulation of tissues,
- induction of controlled damage,
- activation of regenerative processes.
Effects:
- scar flattening,
- improvement in elasticity,
- reduction of erythema.
Laser therapy is particularly effective for hypertrophic and contracture scars.
2. Radiofrequency
Action:
- heating the dermis to 60–70°C,
- shortening of collagen fibers,
- stimulation of fibroblasts.
Used to improve the structure and elasticity of scars.
3. Biostimulating therapies
- mesotherapy with platelet-rich plasma (PRP),
- collagen preparations,
- growth factors.
Their purpose is to support the remodeling of the extracellular matrix.
4. Surgical procedures
In cases of severe contractures, the following are performed:
- Z-plasty,
- skin grafts,
- tissue expanders.
Surgical treatment requires close collaboration with a physiotherapist to prevent recurrence of contractures.
The best therapeutic outcomes are achieved through combined treatment, which encompasses local therapy, laser procedures, and rehabilitation.