Diabetic blisters
back to main page
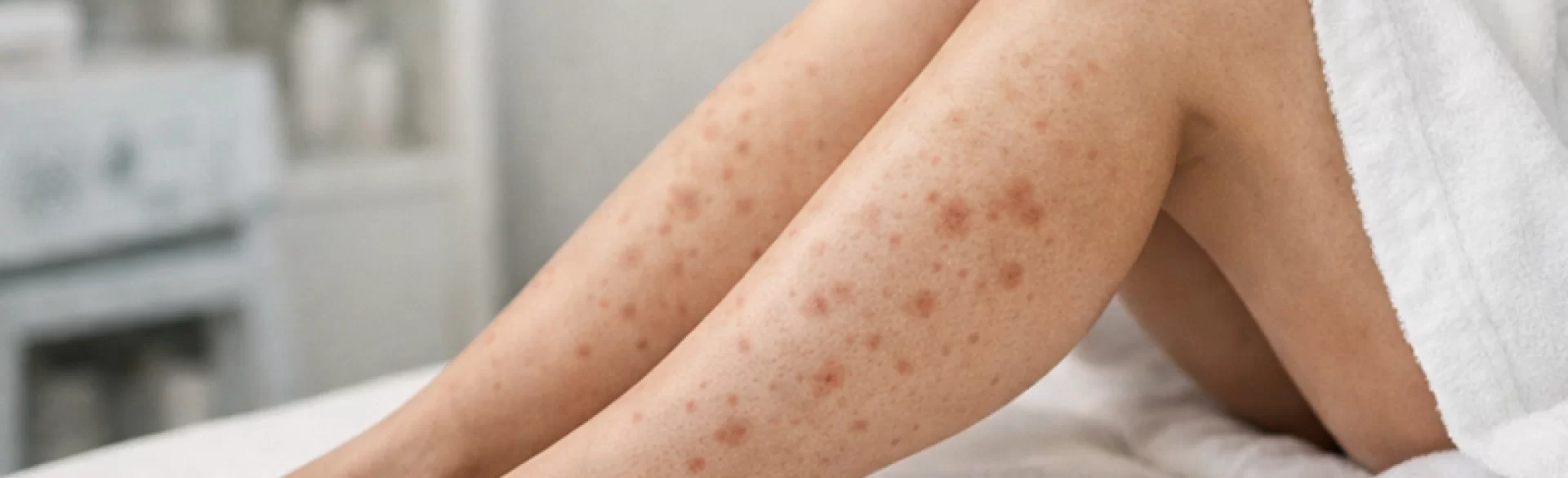
Diabetic bumps are a colloquial term for skin changes that occur in individuals with diabetes, resulting from chronic hyperglycemia (elevated blood glucose levels), diabetic microangiopathy (damage to small blood vessels), and immune system disorders. In dermatology, there is no specific disease entity under this name – it encompasses various dermatoses related to diabetes, including diabetic dermopathy, diabetic blisters (bullosis diabeticorum), lichen sclerosus, and bacterial and fungal skin infections. These changes can be the first sign of undiagnosed diabetes or an indication of metabolically uncontrolled disease. Their presence always requires internal and dermatological diagnostics.
Diabetic blisters - causes
Skin changes in the course of diabetes are the result of complex metabolic and vascular disorders. The main pathogenetic mechanisms include:
1. Chronic hyperglycemia
- Excess glucose leads to protein glycation (the formation of so-called AGE – advanced glycation end products).
- This results in damage to collagen, elastin, and blood vessel walls.
- Nourishment of the skin and its ability to regenerate are impaired.
2. Diabetic microangiopathy
- Damage to small skin vessels causes hypoxia and increased susceptibility to injuries.
- Healing disorders and a tendency to superinfections occur.
3. Peripheral neuropathy
- Decreased sensation of pain and temperature promotes micro-injuries.
- Patients often do not notice minor skin damage, which becomes secondarily infected.
4. Immune disorders
- Diabetes impairs the function of neutrophils and macrophages.
- There is an increased susceptibility to bacterial (e.g., staphylococcal) and fungal (Candida, dermatophytes) infections.
The most common clinical entities referred to as "diabetic dermopathy":
- Diabetic dermopathy – brown spots and papules on the shins.
- Diabetic blisters (bullosis diabeticorum) – sudden, painless blisters on the feet and hands.
- Purulent skin infections – boils, folliculitis.
- Fungal infections of the skin and nails – especially on the feet.
It is worth noting: these changes occur more frequently with long-standing, poorly controlled type 1 and type 2 diabetes.
Diabetic blisters - what do they look like?
The clinical picture depends on the type of dermatosis, but there are some common features.
Characteristic symptoms:
- Papules and pustules – most commonly around hair follicles, with a tendency to enlarge.
- Blisters filled with serous fluid – tense, painless, without inflammatory erythema.
- Brown or reddish spots on the lower legs – 0.5–1.5 cm in diameter, often symmetrical.
- Itching and burning – especially with coexisting fungal infections.
- Tendency for hard-to-heal erosions and ulcers.
Location of changes:
- lower legs,
- feet and interdigital spaces,
- hands,
- groin area,
- buttocks.
Features distinguishing diabetic skin changes from acne vulgaris:
- Patient's age – diabetic skin changes most commonly occur in adults and the elderly, usually with a long history of metabolic disorders. Acne vulgaris primarily affects adolescents and young adults.
- Location of changes – in diabetes, typical areas are the lower legs, feet, interdigital spaces, groin, or buttocks. Acne is mainly located on the face, back, and chest, areas with high sebaceous gland activity.
- Healing process – diabetic changes heal slowly, often leaving pigmentation or erosions and have a tendency for infections. In acne, with proper treatment, the regeneration process is usually faster.
- Relation to glycemia – in diabetes, the severity of changes correlates with glucose levels and HbA1c values. Acne vulgaris does not show a direct connection with carbohydrate metabolism disorders.
Skin changes in diabetes tend to recur, especially with improper HbA1c levels.
Diabetic blisters - treatment
Therapeutic management requires a multidisciplinary approach: diabetological, dermatological, and - in the case of complications - surgical.
1. Metabolic Control (Basis of Treatment)
- optimization of insulin or oral medication therapy,
- monitoring HbA1c (target <7% for most patients),
- weight reduction,
- low glycemic index diet.
Without glucose stabilization, topical treatment has limited effectiveness.
2. Topical Treatment
Depending on the diagnosis:
- Topical or systemic antibiotics - for bacterial infections.
- Antifungal medications - for skin and nail fungal infections.
- Barrier repair preparations - emollients, urea creams (5-10%).
- Specialized dressings - for erosions and ulcers.
3. Procedural Management (in selected cases)
For scars, post-inflammatory hyperpigmentation, or chronic lesions, aesthetic dermatology procedures may be considered, such as:
- Fractional laser therapy - to improve skin structure.
- Medical peels - to reduce hyperpigmentation.
- Regenerative therapies - stimulating skin regeneration.
Each procedure must be preceded by an assessment of the patient's general condition and diabetes control level.
4. Prevention
- daily foot skin check,
- avoiding injuries and tight footwear,
- proper hygiene and thorough drying of interdigital spaces,
- regular visits to a podiatrist for the so-called diabetic foot.
Changes referred to as "diabetic blisters" are a clinical signal of systemic metabolic disorders. In medical practice, they are treated not only as a dermatological issue but as an indicator of the degree of diabetes control and the risk of vascular complications.

