Diaphragm and pelvic floor
back to main page
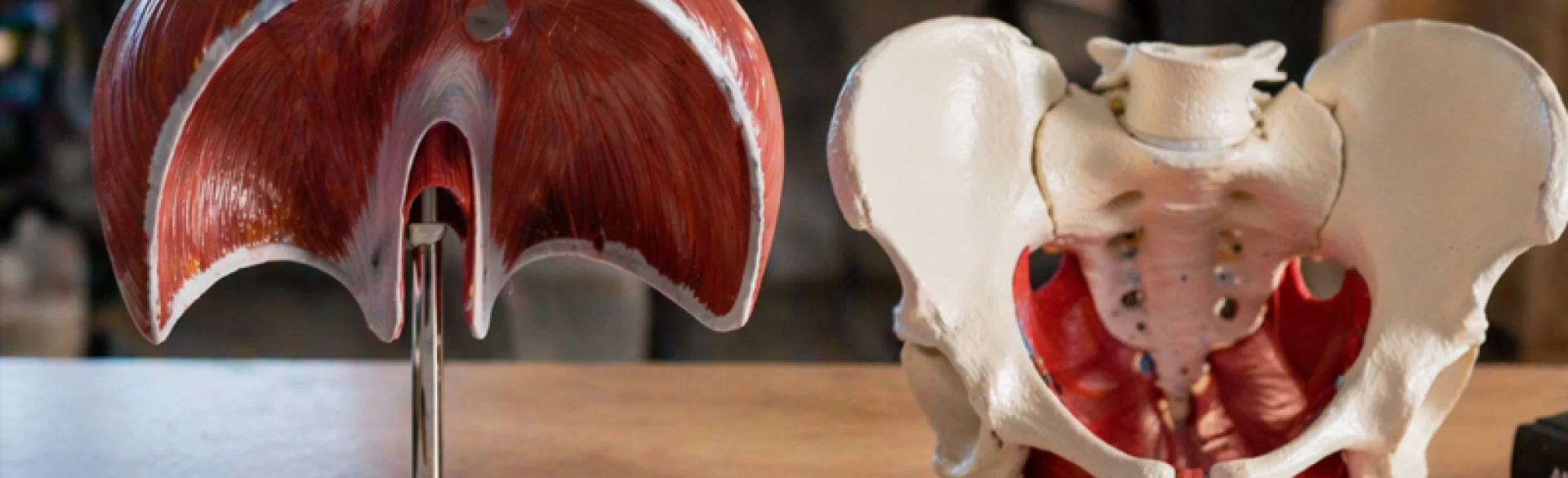
The diaphragm and the pelvic floor constitute a functionally linked muscular system that plays a key role in maintaining proper trunk stabilization, controlling intra-abdominal pressure, and the functioning of internal organs. The diaphragm is the main respiratory muscle separating the thoracic cavity from the abdominal cavity, while the pelvic floor forms the lower closure of the abdominal cavity. Both structures act synchronously, forming, together with the abdominal muscles and the deep muscles of the spine, the so-called stabilization cylinder. Their proper cooperation underpins effective movement biomechanics and proper urogynecological functions.
Diaphragm and pelvic floor – relationship
The relationship between the diaphragm and the pelvic floor is anatomical and functional. Both muscle systems are elements of the so-called central stabilization system (core), which includes:
- the diaphragm (upper boundary),
- the pelvic floor muscles (lower boundary),
- the transverse abdominal muscle,
- the deep spinal muscles (including the multifidus muscle).
During breathing the diaphragm moves in a caudal direction (downward) during the inhalation phase, simultaneously causing a lowering of the pelvic floor. In the exhalation phase the diaphragm rises, and the pelvic floor becomes activated and elevated. This synchronized action provides:
- an even distribution of pressure within the abdominal cavity,
- stabilization of the lumbar spine,
- support for the pelvic organs.
Disruption of this synchrony (e.g., as a result of chronic stress, abnormal breathing patterns, or pregnancy and childbirth) can lead to dysfunction of both the respiratory and urogynaecological systems.
Diaphragm and pelvic floor – the influence of breathing on the muscles
Breathing is a primary mechanism regulating muscle tone within the pelvic floor. The physiological breathing pattern (diaphragmatic breathing) engages the diaphragm, intercostal muscles and abdominal muscles, enabling the harmonious function of the pelvic floor.
Incorrect breathing patterns, such as:
- upper-chest breathing,
- chronic breath-holding,
- excessive activation of the abdominal muscles,
can lead to:
- increased pelvic floor tension (hypertonia),
- weakening of its supportive function,
- disorders of urination and defecation,
- pelvic pain.
Conversely, proper breathing function:
- improves blood flow and oxygenation of tissues,
- supports the flexibility of the pelvic floor muscles,
- allows their proper activation and relaxation.
Therefore, breathing training is a fundamental component of urogynecological physiotherapy and postpartum rehabilitation.
Diaphragm and pelvic floor – intra-abdominal pressure
Intra-abdominal pressure (IAP) is a key biomechanical parameter regulated by the coordinated action of the diaphragm, abdominal muscles and pelvic floor. Under physiological conditions, increases in pressure (e.g., during coughing, sneezing or physical exertion) are distributed evenly, and the pelvic floor provides adequate support for internal organs.
Impaired pressure regulation can lead to:
- stress urinary incontinence,
- pelvic organ prolapse,
- overload of fascial structures,
- worsening separation of the rectus abdominis muscle.
Factors that disrupt proper management of intra-abdominal pressure include:
- chronic constipation and straining,
- improper exercise technique (e.g., intensive „bracing” without breath control),
- obesity,
- chronic cough.
Proper cooperation between the diaphragm and pelvic floor enables dynamic adaptation to pressure changes, protecting anatomical structures from overload.
Diaphragm and pelvic floor – why they are important in therapy
Understanding the relationship between the diaphragm and the pelvic floor forms the foundation of modern therapeutic strategies in physiotherapy, aesthetic medicine, and functional rehabilitation. Therapy focused exclusively on one of these links (e.g., isolated Kegel exercises) without taking the breathing pattern into account often does not yield optimal results.
In clinical practice, a comprehensive approach is used, including:
- breathing therapy (diaphragmatic breathing re-education),
- urogynecological physiotherapy,
- fascial manual therapy,
- core stabilization training,
- work on scars (e.g., after a cesarean section or an episiotomy).
In the context of procedures that support tissue function, methods that improve their quality and elasticity are also used, such as:
- microneedle radiofrequency – stimulating collagen remodeling,
- laser therapy – supporting tissue regeneration and tone,
- regenerative therapies (e.g., platelet-rich plasma) – improving tissue trophism.
An integrated therapeutic approach makes it possible to restore proper function of the muscular system, improve quality of life, and effectively treat pelvic floor disorders.