Eczema
back to main page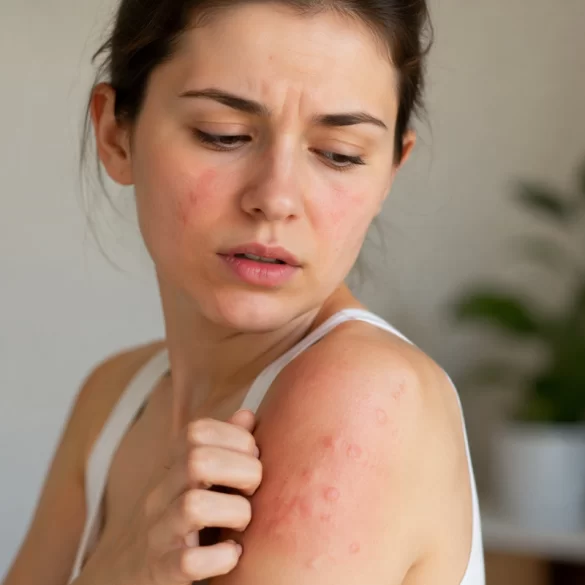

Eczema, also referred to as dermatitis (Lat. eczema), is a chronic or recurrent inflammatory skin disease with a complex etiopatogenesis, involving both immunological and environmental factors. This condition is characterized by damage to the epidermal barrier and an excessive inflammatory response, leading to the occurrence of various skin lesions. Eczema is not a single disease entity, but a group of dermatoses with a similar clinical picture, including, among others, atopic dermatitis, contact dermatitis, or seborrheic dermatitis. The disease can affect people of all ages and significantly affects the quality of life of patients.
Eczema – what it is
Eczema is a heterogeneous group of skin diseases whose common feature is inflammation involving the epidermis and dermis. In the pathogenesis, a key role is played by skin barrier dysfunction, resulting, among others, from disturbances in the structure of epidermal lipids and abnormal synthesis of proteins, such as filaggrin. Impairment of this barrier leads to increased transepidermal water loss (TEWL – transepidermal water loss) and easier penetration of allergens and microorganisms.
Eczema can be:
- acute – with a dominance of exudate and vesicles,
- subacute – with scaling and erythema,
- chronic – with skin thickening (lichenification).
The most commonly distinguished forms of eczema include:
- atopic dermatitis (AD),
- allergic and non-allergic contact dermatitis,
- dyshidrotic eczema,
- seborrheic eczema,
- nummular eczema.
Each of these forms differs in its mechanism of development, yet all lead to a chronic inflammatory process of the skin.
Eczema – what characterizes it
Eczema is characterized by a dynamic and multi-stage course of skin lesions. The clinical picture depends on the phase of the disease, location, and the patient's individual predispositions.
Typical features of eczema include:
- erythema (skin redness) resulting from the dilation of blood vessels,
- edema of the tissues,
- serous vesicles, which may rupture and form erosions,
- exudate and oozing, especially in the acute phase,
- scaling of the epidermis,
- skin thickening (lichenification) in the chronic course,
- intense pruritus.
A characteristic feature is the variability of the clinical picture – different stages of lesions can coexist at the same time. In the chronic course, skin remodeling occurs, along with increased roughness and intensification of skin lines.
Depending on the type of eczema, lesions may be located:
- on the face and neck (often in AD),
- on the hands and feet (contact eczema, dyshidrotic eczema),
- in the joint flexures (elbows, knees),
- on the trunk and limbs.
Eczema – causes
The etiology of eczema is multifactorial and involves the interaction of genetic, immunological, and environmental factors. There is no single universal cause – rather a network of interconnected mechanisms.
Genetic factors
- mutations in the filaggrin gene (FLG),
- predisposition to atopic diseases,
- hereditary hyperreactivity of the immune system.
Immunological factors
- excessive activation of T lymphocytes,
- predominance of Th2-type response (in AD),
- production of pro-inflammatory cytokines (IL-4, IL-13, IL-31).
Environmental factors
- contact allergens (nickel, cosmetics, detergents),
- irritants (chemicals, water, detergents),
- air pollution,
- climate changes (low humidity, cold).
Additional factors
- psychological stress,
- bacterial infections (e.g., Staphylococcus aureus),
- skin microbiome disorders,
- diet (in some cases).
It is worth emphasizing that in contact eczema, direct contact with a sensitizing or irritating substance plays a key role, while in AD, immunological and genetic mechanisms predominate.
Eczema – symptoms
Eczema symptoms are diverse and depend on the stage of the disease and its clinical form. The most characteristic and often dominant symptom is itching, which can lead to a vicious cycle of "itch–scratch–exacerbation of lesions."
Skin symptoms
- erythema and swelling,
- papules and vesicles,
- erosions and oozing,
- crusts,
- scaling,
- lichenification (in the chronic phase),
- excoriations (skin damage due to scratching).
Subjective symptoms
- intense itching,
- burning of the skin,
- feeling of tightness and dryness.
Symptoms of complications
- bacterial superinfections (most commonly staphylococcal),
- viral infections (e.g., herpes),
- sleep disturbances,
- deterioration in quality of life and psychological symptoms (anxiety, frustration).
In the chronic course of eczema, permanent structural changes of the skin occur, which can complicate treatment and increase susceptibility to further exacerbations.
Eczema – how to treat
Eczema treatment requires a comprehensive and individual approach, taking into account both the elimination of triggering factors, as well as symptomatic therapy and the restoration of the skin barrier.
Topical treatment
The basis of therapy consists of preparations applied directly to the skin:
- emollients – they restore the hydrolipid barrier and reduce TEWL,
- glucocorticosteroids – anti-inflammatory and immunosuppressive action,
- calcineurin inhibitors (tacrolimus, pimecrolimus) – an alternative to steroids,
- antiseptic preparations in case of secondary infections.
Systemic treatment
In more severe cases, the following are used:
- antihistamines (reduction of itching),
- oral corticosteroids (short-term),
- immunosuppressive drugs (e.g., cyclosporine),
- modern biological therapies (e.g., dupilumab in AD).
Supportive therapies
In clinical practice, methods supporting skin regeneration and modulating inflammation are becoming increasingly important:
- phototherapy (UVB 311 nm),
- treatments improving skin barrier function,
- procedures reducing inflammation and itching.
In a procedural context, the following are used, among others:
- skin mesotherapy – improvement of hydration and regeneration,
- LED light therapies – anti-inflammatory action,
- regenerative treatments supporting skin restoration,
- medical peels with low irritant potential (only in selected cases, outside the acute phase).
Non-pharmacological management
- avoidance of irritants and allergens,
- use of gentle cleansing agents,
- appropriate skin care (regular lubrication),
- stress reduction,
- patient education.
Effective treatment of eczema requires consistency and a long-term approach – the disease is chronic and recurrent, which is why the goal of therapy is to control symptoms and extend periods of remission.