Epidermal nevus
back to main page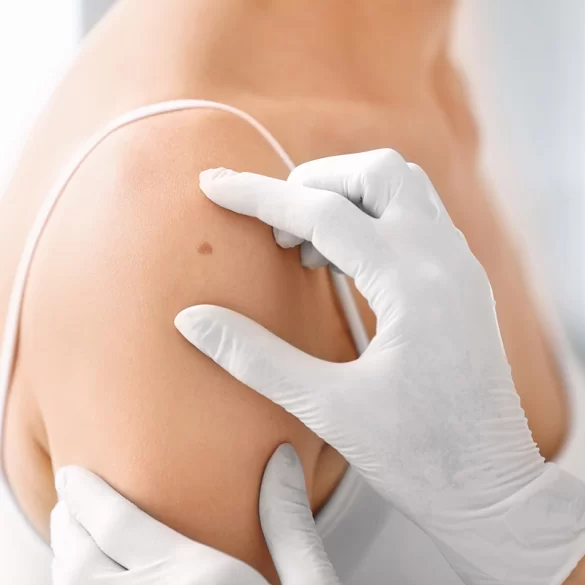
The epidermal nevus (Latin: naevus epidermalis) is a congenital, benign malformation of the skin classified among epidermal nevi, arising from disturbances in the development of epidermal cells and their appendages during the fetal period. These lesions are usually present at birth or appear in early childhood. They have a varied appearance — from flat, slightly pigmented patches to verrucous, thickened lesions with an irregular surface. An epidermal nevus most commonly occurs on the scalp, face, neck, or trunk and may follow the so‑called Blaschko lines, which are characteristic lines of skin cell migration during embryonic development. Although in most cases these lesions are benign, in some situations they require dermatological monitoring or treatment for medical or cosmetic reasons.
Epidermal nevus – types
An epidermal nevus does not constitute a single, homogeneous disease entity. It is a group of skin lesions that differ in histologic (microscopic) structure, clinical appearance, and origin from specific epidermal structures and its appendages. In dermatology, several basic types of epidermal nevi are distinguished.
The most commonly described include:
- verrucous epidermal nevus (verrucous epidermal nevus) – the most common form of epidermal nevus; it appears as raised, warty, rough lesions ranging in color from flesh-toned to brown. It usually appears in childhood and gradually enlarges as the body grows;
- naevus sebaceus (naevus sebaceus) – a lesion associated with abnormal development of the sebaceous glands; it most often localizes to the scalp or face. During puberty it may thicken and change in structure;
- syringocystadenoma papilliferum (syringocystadenoma papilliferum) – a less commonly encountered variant, originating from the sweat glands;
- follicular nevus – associated with abnormal development of hair follicles; it may manifest as clusters of papules or areas of hyperkeratosis around follicular openings;
- epidermal nevus syndrome (epidermal nevus syndrome) – a rare form in which the skin lesions coexist with developmental disorders of other organs, e.g., the skeletal system, nervous system, or eyes.
These lesions often arrange themselves linearly or in bands, which results from their development along the aforementioned Blaschko's lines. In most cases they are stable and do not undergo malignant transformation; however some variants — especially naevus sebaceus — may, in rare cases, provide a basis for the development of secondary skin tumors.
Epidermal nevus – causes and mechanism of formation
An epidermal nevus arises as a result of developmental disturbances of the skin during the fetal period. Underlying it are somatic genetic mutations, i.e., changes in the genetic material of skin cells that occur during embryonic development and are not inherited from the parents. Such mutations lead to the so-called genetic mosaicism, a situation in which part of the body's cells carry altered genetic material while the remaining cells remain normal.
In the case of epidermal nevi, the mutations most often affect genes related to the regulation of growth and differentiation of epidermal cells. The most frequently described include mutations in the genes:
- FGFR3 (fibroblast growth factor receptor 3)
- PIK3CA
- HRAS and KRAS
These changes lead to uncontrolled proliferation of keratinocytes, i.e., the primary cells that make up the epidermis. As a result, an area of skin with altered structure and increased cell proliferation forms.
A characteristic feature of epidermal nevi is their arrangement along Blaschko's lines. These are lines not visible in normal skin that correspond to the pathways of epidermal cell migration during embryonic development. Therefore the lesions often take on a:
- band-like,
- linear,
- spiral or wavy,
In most cases an epidermal nevus is present at birth or becomes apparent in early childhood. Lesions may gradually enlarge with the growth of the organism, but usually grow proportionally with body growth.
It is worth emphasizing that epidermal nevi are not infectious nor an acquired lesion – their presence results from developmental disturbances of the skin that occur before birth.
Epidermal nevus – what it looks like and where it occurs
The clinical presentation of an epidermal nevus can be very varied, which results from differences in the histological structure of the various types of lesions. Most often these are raised, thickened, or warty lesions, with an uneven surface and a color ranging from light brown to dark brown.
Typical clinical features of epidermal nevi include:
- a rough, warty surface, sometimes resembling viral warts,
- a linear or band-like distribution of lesions,
- an irregular shape,
- slow growth as the body develops.
In some cases, the lesions may appear as:
- flat discolorations,
- thickened skin plaques,
- clusters of small papules.
The most common locations of epidermal nevi are:
- scalp,
- face,
- neck,
- trunk,
- upper and lower extremities.
Lesions may occur singly or involve larger areas of skin. In rare cases they take the form of extensive bands affecting a significant portion of the body.
In some patients an epidermal nevus may be part of the so‑called epidermal nevus syndrome. In such cases, in addition to skin lesions, other developmental abnormalities may also occur, e.g.:
- skeletal abnormalities,
- neurological disorders (e.g., epilepsy),
- ocular defects.
However, such situations are rare.
In most cases an epidermal nevus is benign and stable, but any skin lesion with an irregular appearance should be evaluated by a dermatologist. Particular attention should be paid when a lesion:
- begins to grow rapidly,
- changes color or texture,
- becomes ulcerated or bleeds.
In such cases, more detailed dermatological diagnostics may be necessary, and sometimes also histopathological examination of the removed lesion.
Epidermal nevus – is it dangerous?
In the vast majority of cases an epidermal nevus is a benign lesion and does not pose a health risk. It is a congenital malformation of the skin resulting from local disturbances in the development of the epidermis, not a skin tumor. These lesions usually grow very slowly and remain stable for many years.
The risk of malignant transformation is small, however in some variants of epidermal nevi – particularly within a sebaceous nevus (naevus sebaceus) – secondary skin tumors may develop later in life. Most often these are benign tumors, such as:
- sweat gland adenoma (syringocystadenoma papilliferum),
- trichoblastoma,
- sebaceous adenoma.
Less commonly, malignant skin tumors may develop within the nevus, for example:
- basal cell carcinoma,
- very rarely other skin malignancies.
For this reason periodic dermatological follow-up of skin lesions is recommended, especially when the nevus:
- begins to enlarge noticeably,
- changes color or texture,
- becomes painful or itchy,
- bleeds or becomes ulcerated.
In such situations the doctor may recommend dermoscopy, a non-invasive examination that allows assessment of the lesion’s structure at high magnification. If diagnostic doubts remain, excision of the lesion and histopathological examination is performed, which allows definitive determination of its nature.
It is also worth emphasizing that in many cases an epidermal nevus represents an aesthetic or functional problem, especially when located on the face, scalp, or in areas exposed to chronic irritation. In such situations dermatological or surgical treatment may be considered, with the aim of improving skin appearance and preventing chronic inflammatory conditions.
Epidermal nevus – treatment
In many cases an epidermal lesion does not require treatment, especially when the lesion is small, stable and does not cause clinical symptoms. The decision about therapy depends primarily on the location of the lesion, its size, symptoms and aesthetic considerations. Indications for treatment may also include rapid enlargement of the lesion, mechanical irritation or suspicion of malignant transformation.
The most commonly used treatment methods include:
1. Surgical treatment
Surgical excision is the method of choice in cases of:
- large lesions,
- lesions suspected of malignancy,
- nevi causing chronic irritation.
An advantage of this method is the possibility of performing a histopathological examination at the same time, which allows for an accurate assessment of the nature of the lesion.
2. Laser treatment
In aesthetic dermatology ablative lasers (e.g., CO₂ laser or erbium-YAG laser) are often used, which enable layer-by-layer removal of the lesion by vaporizing the altered tissue. This method allows for:
- improvement of the skin's appearance,
- reduction of the lesion's elevation,
- reduced scarring compared with traditional excision.
However, it should be remembered that laser treatment does not always remove the lesion completely, so in some cases partial recurrence is possible.
3. Other dermatological methods
In selected situations the following are also used:
- cryotherapy (treatment with liquid nitrogen),
- electrocoagulation,
- dermabrasion.
These methods are usually used for smaller superficial lesions.
In clinical practice the treatment of epidermal lesions is often individually tailored, taking into account both medical and aesthetic aspects. In modern dermatology and aesthetic medicine clinics various techniques are used to remove skin lesions, including laser removal of skin lesions, surgical excision of nevi and procedural dermatology treatments that improve skin texture.