Genital warts
back to main page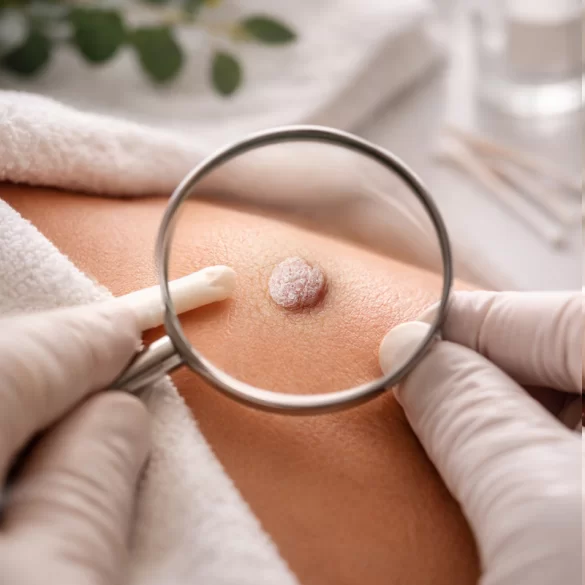
Genital warts, also known as condylomata acuminata, are one of the most common sexually transmitted diseases. They are caused by the human papillomavirus (HPV), primarily the low-oncogenic types 6 and 11. These lesions are benign growths of the epithelium of the skin and mucous membranes in the genital area and around the anus. Although the warts themselves do not typically pose an oncogenic threat, the presence of HPV infection is associated with the risk of virus transmission and, in the case of other HPV types, the development of precancerous and cancerous changes.
Genital warts - what are they?
Genital warts are the result of local proliferation (multiplication) of epithelial cells infected with the HPV virus. The virus enters the basal layer of the epidermis through micro-injuries and then uses cellular mechanisms to replicate its genetic material.
Key information:
- Etiological factor: HPV types 6 and 11 (over 90% of cases).
- Mode of transmission: primarily sexual contact (vaginal, anal, oral).
- Incubation period: from a few weeks to a few months (on average 2-3 months).
- Prevalence: one of the most common sexually transmitted infections among sexually active individuals.
It is worth noting that HPV infection can be asymptomatic. The immune system of some individuals eliminates the virus spontaneously within 1-2 years, but in others, the infection becomes persistent and clinical changes develop.
Factors promoting the development of warts:
- reduced immunity (e.g., stress, chronic diseases, immunosuppression),
- frequent change of sexual partners,
- co-existing other sexually transmitted infections,
- micro-injuries to the skin and mucous membranes.
Genital warts - symptoms
The symptoms of genital warts vary and depend on their location and number. In many cases, they are initially sparse in symptoms.
Most common complaints:
- Presence of single or multiple soft growths in the genital area,
- Itching, burning, or a feeling of discomfort,
- Bleeding from mechanical injury (e.g., during intercourse),
- Increased vaginal discharge (in women),
- Pain during urination or defecation (in case of perianal location).
In women, the lesions may be located:
- On the labia,
- In the vaginal vestibule,
- On the cervix,
- In the anal area.
In men, they most commonly occur:
- On the glans and foreskin,
- In the frenulum area,
- On the shaft of the penis,
- In the anal area.
In the case of lesions on the cervix, they may remain invisible to the naked eye and can only be detected during a gynecological examination, Pap smear, or colposcopy.
Genital warts - what do they look like
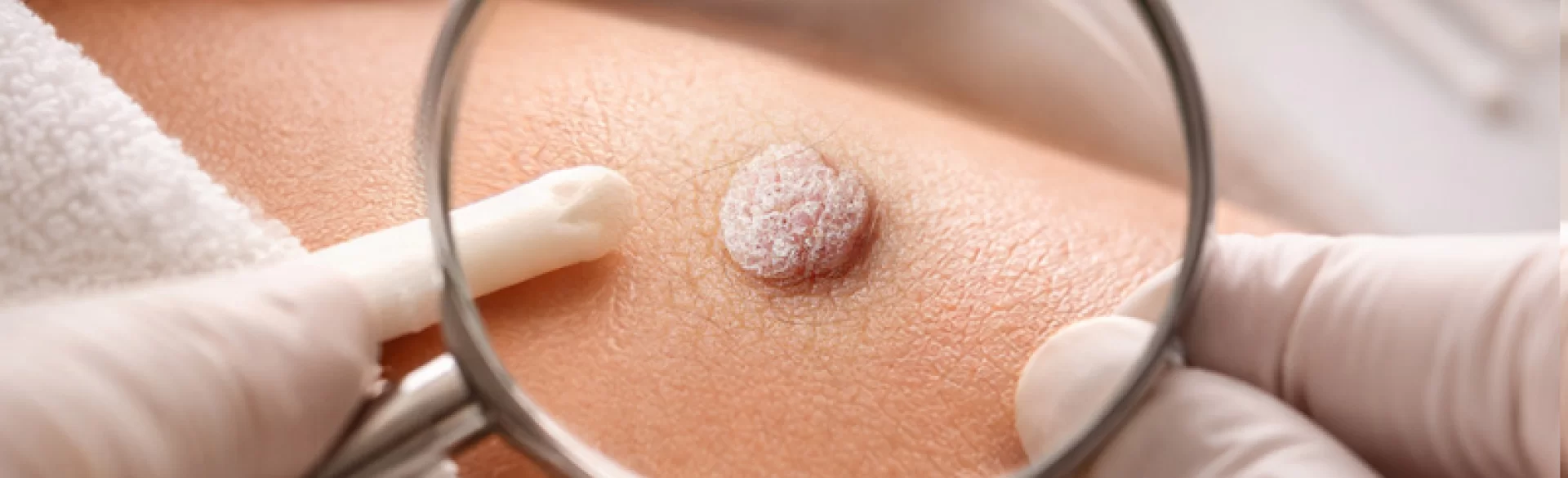
Genital warts have a characteristic clinical appearance, although their appearance can vary.
Typical morphological features:
- soft, pedunculated, or flat growths,
- flesh-colored, pink, or slightly brownish,
- irregular, warty surface,
- tendency to merge into larger clusters.
In advanced cases, the lesions may form extensive structures resembling cauliflower (known as cauliflower-like appearance).
Several clinical forms are distinguished:
- classical condylomata acuminata – distinctly elevated, warty lesions,
- flat form – more difficult to notice, often requires specialized diagnostics,
- giant form (Buschke-Löwenstein tumor) – rarely occurring, with aggressive local progression.
Differential diagnosis includes:
- soft fibromas,
- molluscum contagiosum,
- psoriatic lesions,
- precancerous and cancerous conditions.
For this reason, any suspicious lesion on the genital area should be evaluated by a doctor (dermatologist, gynecologist, urologist).
Genital warts - treatment
The treatment of genital warts aims to remove clinical lesions and limit virus transmission. However, it must be clearly stated that no method completely eliminates the virus from the body, and recurrences are possible.
Treatment methods can be divided into:
1. Topical treatment (pharmacological)
- imiquimod (stimulates immune response),
- podophyllotoxin (cytotoxic action),
- trichloroacetic acid (chemical coagulation).
These are mainly used for small, superficial lesions.
2. Surgical treatment
- CO₂ laser therapy – precise vaporization of the lesion,
- electrocoagulation,
- cryotherapy (freezing with liquid nitrogen),
- surgical excision of the lesion.
In clinical practice, surgical methods are characterized by:
- greater effectiveness with multiple and extensive lesions,
- the possibility of obtaining material for histopathological examination,
- shorter therapy time.
In clinical settings, such as Ambasada Urody Clinic & Spa in Warsaw, the following are applied:
- surgical removal of skin lesions,
- laser removal of skin lesions,
- dermatoscopic diagnostics and qualification for histopathological examination.
3. Prevention
The most effective methods of preventing HPV infections are:
- HPV vaccinations (multivalent vaccines),
- use of condoms (reduces but does not eliminate the risk),
- regular gynecological and cytological examinations.
For women, systematic cytology is crucial and, in certain situations, HPV DNA testing.

