Guttate psoriasis
back to main page
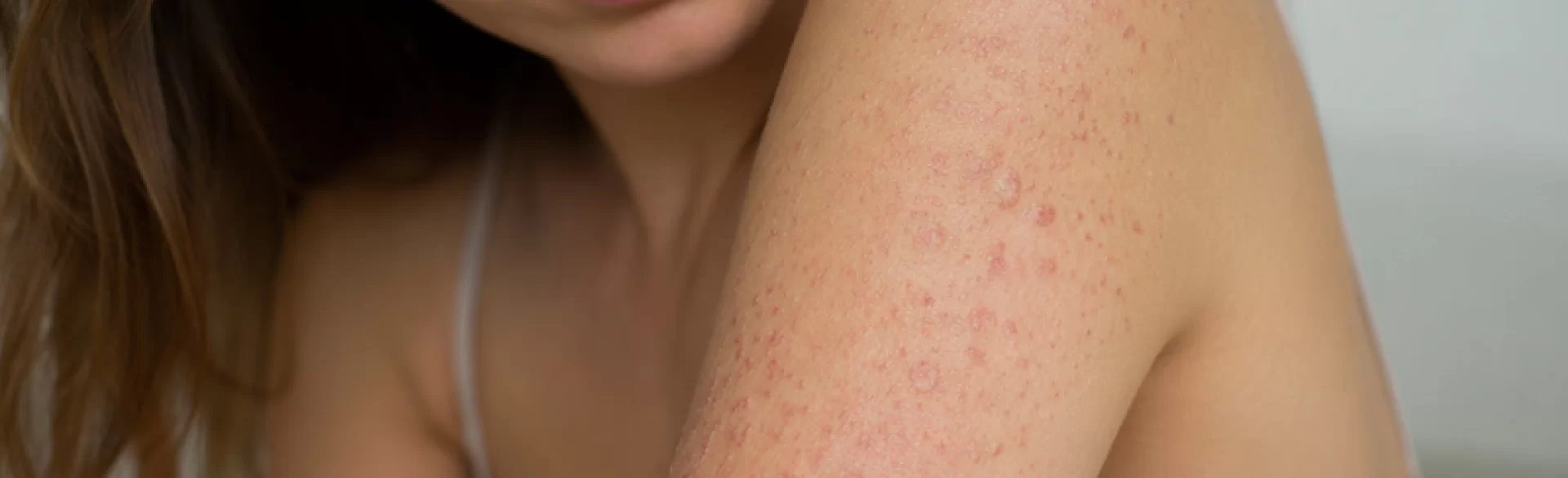
Guttate psoriasis (psoriasis guttata) is one of the clinical forms of psoriasis, a chronic inflammatory skin disease with an immunological basis. It is characterized by the sudden appearance of numerous, small, drop-shaped skin lesions, most commonly on the trunk and limbs. Unlike plaque psoriasis, the lesions are smaller in size and more disseminated in nature. The disease often occurs in children and young adults, and its development is often associated with a previous infection, particularly streptococcal. The course can be acute or transient; however, in some patients, it transforms into a chronic form.
Guttate psoriasis – what it looks like
Guttate psoriasis is distinguished by a characteristic clinical picture that allows for its relatively quick diagnosis. Skin lesions appear suddenly and take the form of numerous, small papules and spots with a diameter usually ranging from a few millimeters to about 1–2 cm.
Typical features of the lesions include:
- teardrop shape – the lesions resemble drops of water (hence the name "guttata"),
- pink or red color – resulting from the ongoing inflammatory process,
- presence of a fine scale – superficial scaling of the epidermis,
- symmetrical distribution – particularly on the trunk, back, chest, and limbs,
- sudden eruption of lesions – often within a few days.
Lesions less commonly involve the face, hands, and feet, which distinguishes this form from other varieties of psoriasis. Pruritus may occur, but it is usually of moderate intensity.
In the dermoscopic and histopathological picture, features typical of psoriasis are observed:
- parakeratosis (disorder of epidermal keratinization),
- acanthosis (thickening of the epidermis),
- elongation of rete ridges,
- inflammatory infiltrate in the dermis.
An important diagnostic element is the temporal relationship with an infection, especially:
- streptococcal pharyngitis (strep throat),
- pharyngitis,
- upper respiratory tract infections.
In many patients, the lesions resolve spontaneously within a few weeks or months; however, in some, recurrences occur or the condition progresses into plaque psoriasis.
Guttate psoriasis – treatment
Treatment of guttate psoriasis depends on the severity of the lesions, the patient's age, and the presence of triggering factors. In many cases, the disease is self-limiting; however, proper therapy accelerates the resolution of lesions and reduces the risk of recurrence.
General management
The basis is the identification and elimination of the triggering factor, especially bacterial infection. In the case of a confirmed streptococcal infection, the following are used:
- antibiotic therapy (e.g., penicillins or cephalosporins),
- treatment of infection foci (e.g., tonsils).
Additionally, it is recommended to:
- avoid stress,
- ensure proper skin care,
- use emollients that restore the epidermal barrier.
Topical treatment
In mild and moderate cases, topical therapy is the mainstay:
- glucocorticosteroids – anti-inflammatory and immunosuppressive action,
- vitamin D₃ analogs (calcipotriol) – regulation of keratinocyte proliferation,
- keratolytic preparations (e.g., salicylic acid) – scale reduction,
- tars and coal tar preparations – anti-proliferative and anti-inflammatory action.
Phototherapy
One of the most effective methods for treating guttate psoriasis is phototherapy:
- UVB 311 nm (narrowband UVB) – inhibition of excessive skin cell proliferation,
- PUVA (psoralen + UVA) – used in more severe cases.
The mechanism of action is based on:
- modulation of the immune response,
- reduction of T lymphocyte activity,
- reduction of inflammation.
Systemic treatment
In severe cases or cases resistant to topical treatment, systemic treatment is used:
- methotrexate – an immunosuppressive drug,
- cyclosporine – inhibition of T lymphocyte activity,
- retinoids (acitretin) – regulation of epidermal differentiation.
Biological drugs, which act selectively on specific pro-inflammatory cytokines (e.g., TNF-α, IL-17, IL-23), are also becoming increasingly important. However, this therapy is reserved for severe forms of the disease.
Supportive therapies and procedures
Modern dermatology and aesthetic medicine offer methods that support treatment and improve skin quality:
- LED light therapies – anti-inflammatory and regenerative action,
- procedures using radiofrequency (RF) – improvement of microcirculation and skin regeneration,
- needle and microneedle mesotherapy – support for skin reconstruction,
- regenerative therapies (e.g., platelet-rich plasma) – stimulation of repair processes.
Although they do not constitute a causal treatment for psoriasis, they can support the skin regeneration process and improve its condition after the lesions have resolved.
Prognosis
Guttate psoriasis often has a favorable prognosis:
- in many patients, the lesions resolve completely,
- recurrences are possible, especially after subsequent infections,
- in some patients, a chronic form of psoriasis develops.
Early implementation of treatment and elimination of triggering factors significantly improve the course of the disease.