Hair bulb
back to main page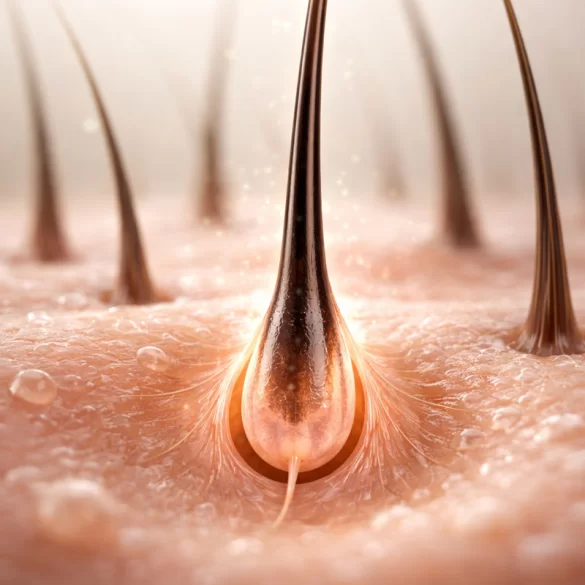

The hair bulb is the lower, living part of the hair follicle, located in the deep layers of the dermis, and in the case of terminal hair, even in the subcutaneous tissue. It is a key component of the hair apparatus, responsible for hair growth, nourishment, and pigmentation. Within it, there are intensely proliferating matrix cells, the dermal papilla, and melanocytes producing pigment. The hair bulb is a dynamic structure, and its activity depends on the phase of the hair cycle (anagen, catagen, telogen). Damage to the bulb can lead to hair growth disorders, thinning, and in some cases, permanent hair loss.
Hair bulb – what it looks like
The hair bulb is shaped like an expanded, spherical structure resembling an "onion," from which it gets its name. It is the lower part of the hair follicle, surrounding the dermal papilla, which is richly vascularized and innervated.
The structure of the hair bulb includes:
- Hair matrix – cells that divide intensively through mitosis, responsible for the growth of the hair shaft.
- Dermal papilla – a connective tissue structure with a network of blood vessels supplying oxygen and nutrients.
- Melanocytes – cells that produce melanin, determining the color of the hair.
- Inner and outer sheaths – protective and supportive layers of the hair follicle.
In microscopic view, the hair bulb in the anagen phase is large, well-demarcated, and strongly vascularized. In the catagen phase, it shrinks, while in the telogen phase it transforms into the so-called club hair – with the atrophy of the active matrix.
Macroscopically, when a hair is pulled out in the telogen phase, a clear, thickened tip is visible – this is the dead part of the bulb.
Hair follicle – does it grow back
The possibility of hair regrowth depends on the degree of damage to the matrix structures and the dermal papilla.
Hair regrowth is possible when:
- the dermal papilla is intact,
- there is no permanent damage to the stem cells within the follicle,
- there is no fibrosis (scarring) within the hair follicle.
Plucking hair (e.g., mechanical depilation) usually does not permanently damage the bulb – hair regrows because hair follicles go through successive growth cycles.
However, in cases of:
- scarring alopecia,
- deep burns,
- severe inflammatory conditions,
- chronic androgenic alopecia in advanced stages,
there may be permanent destruction of the follicle and loss of regenerative capacity.
Systemic factors also play a significant role:
- hormonal disorders (e.g., hypothyroidism),
- deficiencies of iron, zinc, vitamin D,
- chronic oxidative stress,
- autoimmune diseases (e.g., alopecia areata).
Modern trichology and regenerative medicine utilize, among others, mesotherapy, platelet-rich plasma, or therapies stimulating microcirculation to improve bulb function – provided that it has not been irreversibly damaged.
Hair bulb - what color is it
The color of the hair bulb depends on the phase of the growth cycle and the presence of melanin.
- In the anagen phase, the bulb is heavily vascularized and contains active melanocytes – it may have a darker, brownish hue (especially in people with dark hair).
- In the telogen phase, the bulb takes on a light, whitish-transparent appearance (known as the club hair).
- In the case of graying, there is a gradual loss of melanocytes within the matrix – the bulb becomes devoid of pigment.
It is worth noting that the visible "white tip" of a plucked hair does not always indicate disease – in most cases, it is a physiological telogen form.
However, a change in the color of the bulb may accompany:
- pigmentation disorders,
- chronic inflammatory processes,
- toxic damage to the follicle (e.g., chemotherapy).
Hair bulb – diseases
The hair follicle can be affected by inflammatory, autoimmune, and degenerative processes. The most important disease units include:
1. Androgenic alopecia
- progressive miniaturization of follicles,
- shortening of the anagen phase,
- decrease in bulb volume.
2. Alopecia areata
- autoimmune disease,
- lymphocytic infiltration around the bulb,
- inhibition of matrix activity.
3. Scarring alopecia
- permanent destruction of the hair follicle,
- replacement of structure with fibrous connective tissue,
- lack of regrowth capability.
4. Folliculitis
- bacterial, fungal, or viral etiology,
- pain, erythema, pustules,
- possible secondary bulb damage.
5. Telogen effluvium
- excessive transition of hairs to the resting phase,
- usually reversible after eliminating the triggering factor.
Diagnostics include:
- trichoscopy,
- laboratory tests,
- in selected cases, skin biopsy.
Early identification of hair follicle dysfunction is crucial for effective treatment. Inflammatory and autoimmune processes often require systemic therapy, while metabolic disorders require correction of deficiencies and support of microcirculation.