Histopathological examination
back to main page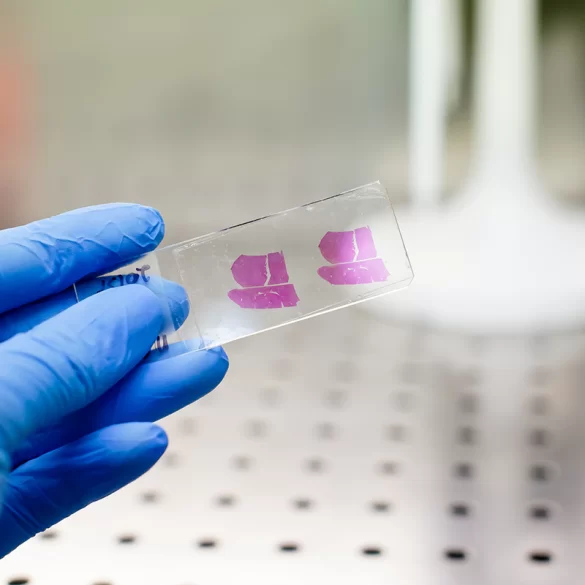

Histopathological examination is the microscopic evaluation of a tissue sample taken from a patient to determine its cellular structure and any potential pathological changes. It is considered the gold standard in the diagnosis of many conditions, especially cancers, as it allows for the direct assessment of tissue architecture, cellular atypia, and the presence of inflammatory infiltration or proliferative processes. The material for examination is most commonly obtained during a biopsy, surgical procedure, or removal of a skin lesion. The histopathological result forms the basis for making a definitive diagnosis and planning further treatment—whether it be conservative, surgical, or oncological.
Histopathological examination – what is it?
The histopathological examination involves the analysis of fixed tissue (usually in 10% formalin), dehydrated, embedded in paraffin, and then cut into very thin sections (3–5 µm), which are stained and evaluated under a light microscope.
The stages of the procedure include:
- collection of material (fine-needle biopsy, core-needle biopsy, surgical excision, lesion removal),
- fixation and laboratory processing,
- preparation of microscopic slides,
- evaluation by a pathologist.
If necessary, additional tests are performed:
- immunohistochemistry (IHC) – detection of specific cancer proteins,
- molecular studies (e.g., BRAF, KRAS mutations),
- assessment of surgical margins.
In dermatology and aesthetic medicine, histopathological examination is crucial for:
- suspicion of melanoma,
- atypical pigmented nevi,
- skin tumors (basal cell carcinoma, squamous cell carcinoma),
- lesions that are rapidly growing, bleeding, or have irregular borders.
It should be emphasized that dermoscopy is a screening test, whereas the definitive diagnosis is made exclusively by histopathology.
Histopathological examination - what it detects
The diagnostic scope of histopathological examination is very broad. It allows for the detection of:
1. Neoplastic changes
- benign tumors (e.g., fibromas, lipomas),
- malignant tumors (e.g., melanoma, skin cancer, breast cancer),
- precancerous changes (dysplasia, actinic keratosis).
2. Inflammatory conditions
- chronic and acute inflammations,
- autoimmune diseases (e.g., lichen planus),
- granulomatous diseases.
3. Dermatological diseases
- psoriasis,
- systemic lupus erythematosus,
- pemphigus and pemphigoid (using immunofluorescence).
4. Evaluation of surgical margins
After the removal of a neoplastic lesion, histopathology determines whether the excision was radical (i.e., whether the margins are clear of cancer cells). This is crucial for planning further treatment.
In oncology, this examination also allows for:
- assessment of malignancy grade (grading),
- determination of infiltration depth (e.g., Breslow scale in melanoma),
- qualification for systemic treatment.
Histopathological Examination - Results
The result of a histopathological examination is in the form of a medical report prepared by a pathologist. It contains:
- patient identification data,
- macroscopic description of the material,
- microscopic description,
- final diagnosis,
- any recommendations for further diagnostics.
In the case of neoplastic changes, the report may include:
- histological type of the tumor,
- degree of differentiation (G1–G3),
- presence of vascular invasion,
- width of surgical margins,
- TNM classification (if applicable).
Waiting time for the result:
- standard: 7–14 days,
- urgent (intraoperative): even within 30–60 minutes (so-called immediate examination).
The interpretation of the result should always be correlated with the clinical picture and additional examinations (ultrasound, magnetic resonance imaging, tumor markers).
Histopathological examination – when to perform
Indications for performing a histopathological examination include situations where there is suspicion of significant structural tissue pathology.
In dermatology and skin surgery:
- A pigmented lesion with irregular borders,
- Asymmetry of a mole,
- Rapid growth of a lesion,
- Ulceration or bleeding,
- A persistent change despite treatment.
In gynecology:
- Abnormal cytology results,
- Endometrial polyps,
- Suspicion of cervical cancer.
In general surgery:
- Breast nodules,
- Changes in the gastrointestinal tract,
- Suspicion of metastases.
There should be no delay in performing the examination if there are any features suggesting a tumor. The clinical practice rule is: every excised skin lesion should be submitted for histopathological examination, even if it appears clinically benign.
In the case of surgical removal of skin lesions, it is advised to:
- send the material for histopathological examination,
- check the wound after 7-14 days,
- discuss the result with a doctor,
- if necessary, widen the surgical margin.
As part of the procedures carried out at the Ambasadzie Urody Clinic & Spa, this includes:
- surgical removal of moles,
- removal of skin lesions,
- dermatoscopic diagnostics,
- qualification for further dermatological or oncological treatment.
Every lesion raising clinical doubts requires confirming diagnostics. In medicine, there is no effective alternative to histopathological examination for the final structural diagnosis of tissue.