Laparoscopy scars
back to main page
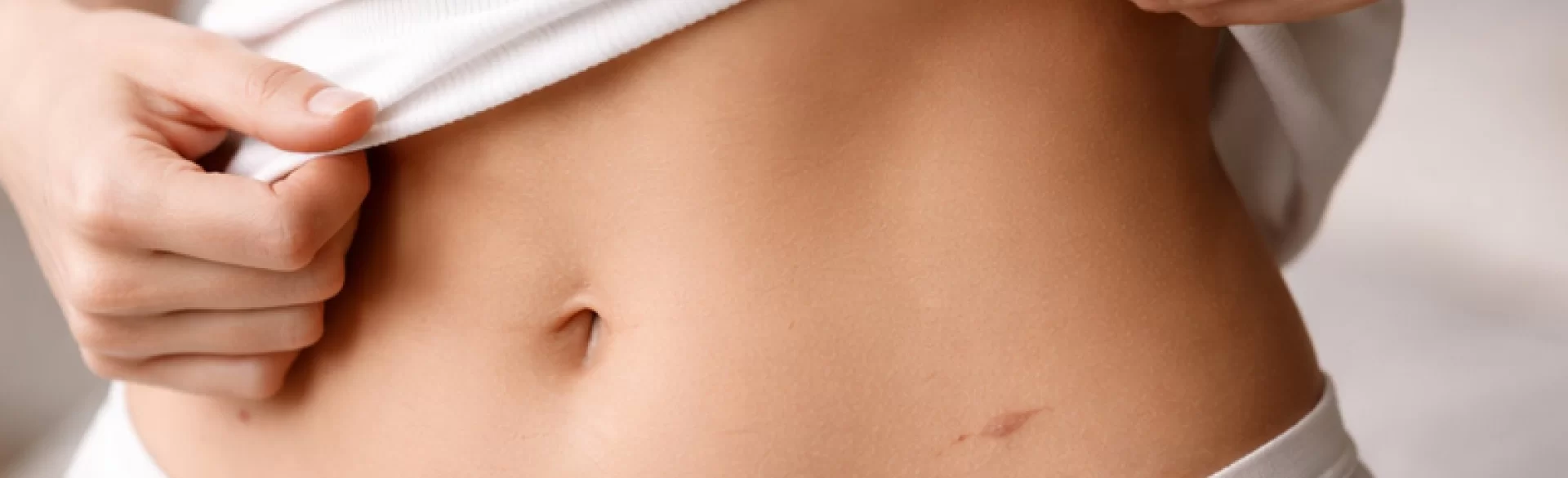
Scars from laparoscopy are small skin changes that occur at the sites where trocars (surgical instruments) are inserted into the abdominal cavity during minimally invasive surgery. Laparoscopy, used in general surgery, gynecology, and urology, typically involves making 2–4 incisions ranging from 5–12 mm in length. Although this method significantly reduces tissue trauma compared to laparotomy, the healing process still leads to scar formation – a result of the physiological repair of the skin and subcutaneous tissues. The quality and visibility of the scar depend on several factors: surgical technique, genetic predisposition, the healing process, wound infection, and proper postoperative care.
Laparoscopy scars – how to care for them
Proper care of a laparoscopic wound is crucial for reducing the risk of complications and minimizing scar visibility. The healing process occurs in three phases: inflammatory, proliferative, and remodeling, which can last up to 12–18 months.
Basic principles of management:
- Keep the wound clean and dry during the first few days after the procedure.
- Avoid excessive skin tension around the scar area (intense physical activity, lifting heavy objects).
- Protect from UV radiation for at least 6–12 months (SPF 50+ filters) to prevent post-inflammatory hyperpigmentation.
- Early inclusion of silicone therapy (patches, gels) after complete epidermal healing.
- Gentle scar massage (after suture removal and wound healing) to improve tissue elasticity and limit adhesions.
Factors that increase the risk of improper scarring include:
- diabetes and microcirculation disorders,
- postoperative wound infection,
- tendency to keloids,
- protein and vitamin C deficiencies.
It is important to emphasize that starting therapy too late (e.g., a year after surgery) limits the possibilities for full correction of the scar structure. Prevention is always more effective than treating an established change.
Laparoscopy scars – what do they look like
A typical laparoscopic scar appears as:
- a small, linear or pinpoint change measuring 0.5–1.5 cm in length,
- initially pink or red (related to blood supply),
- eventually fading and flattening over time.
The most common locations are:
- around the navel (optical port),
- lower abdomen,
- above the pubic region.
Possible clinical variants:
- Normotrophic scar – thin, elastic, almost invisible after a few months.
- Hypertrophic scar – thickened, elevated above the skin level, confined to the area of the incision.
- Keloid – growing beyond the boundaries of the original wound.
- Atrophic scar – sunken, associated with the loss of subcutaneous tissue.
Within the scar, the following may occur:
- temporary sensory disturbances (paresthesias),
- tenderness upon pressure,
- a sensation of pulling – especially with fascial adhesions.
In the case of persistent pain or bulging at the scar site, a postoperative hernia should be ruled out.
Laparoscopy scars – ointments
Topical preparations that support scar remodeling work by modulating collagen synthesis and maintaining an appropriate level of hydration.
Best clinically documented:
- Silicone gels and sheets – the gold standard for hypertrophic scar prevention; they work through occlusion and regulation of the skin's water balance.
- Preparations with heparin and allantoin – support tissue remodeling and reduce inflammation.
- Onion extract (Allium cepa) – exhibits anti-inflammatory and antiproliferative effects.
- Preparations with vitamin E – their effectiveness is controversial; they may cause contact dermatitis.
Silicone usage regimen:
- start after full wound healing,
- apply 12–24 hours a day,
- minimum 2–3 months (longer if there is a tendency to develop keloids).
It should be emphasized that no topical preparations "remove" scars – they can only improve their structure and appearance during the remodeling phase.
Laparoscopy Scars – Treatments
In the case of persistent, aesthetically unacceptable, or symptomatic scars, it is possible to apply procedural therapies.
Most commonly used methods:
- Fractional CO₂ laser – stimulates collagen remodeling and smooths the scar surface.
- Microneedle radiofrequency – improves tissue tension and elasticity.
- Platelet-rich plasma (PRP) therapy – supports regeneration and remodeling.
- Needle mesotherapy – improves hydration and the structure of atrophic scars.
- INDIBA therapy (448 kHz) – supports tissue regeneration by stimulating cellular metabolism and microcirculation.
- Steroid injections (triamcinolone) – used in treating hypertrophic scars and keloids.
- Surgical scar revision – in selected cases.
In clinical practice, combined therapies are often used because the process of collagen remodeling requires multidirectional stimulation.
In the treatment of postoperative scars, the following are used, among others:
- fractional laser therapy,
- microneedle radiofrequency,
- regenerative mesotherapy,
- procedures utilizing INDIBA technology.
The choice of method should be preceded by an assessment of the type of scar, the time since surgery, and the patient's predisposition to abnormal scarring.