Measles spots
back to main page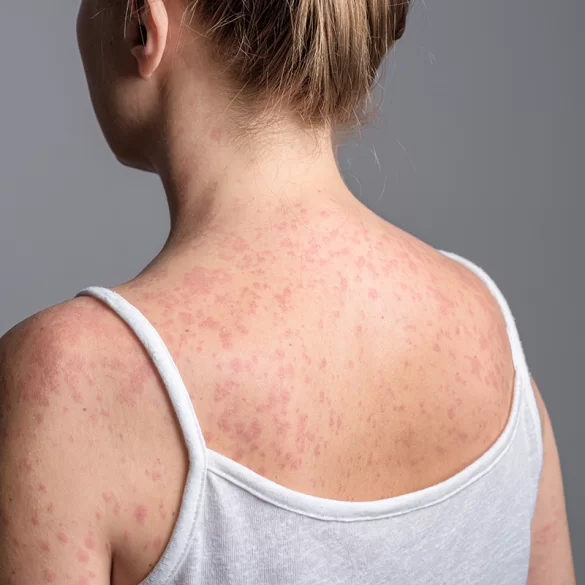
"Krosty odry" is a colloquial term for the skin lesions that appear in the course of measles (morbilli) – an acute, highly contagious viral disease caused by the measles virus of the genus Morbillivirus (family Paramyxoviridae). The characteristic measles rash takes the form of maculopapular skin lesions and is one of the main clinical manifestations of the disease. These lesions usually appear several days after the onset of general symptoms such as fever, cough, coryza or conjunctivitis. The rash has a characteristic pattern of spread on the skin and is accompanied by an intense immune response. Although the term "krosty odry" is used colloquially, in reality these lesions represent a maculopapular viral rash, not typical pustules.
Measles spots – what do they look like
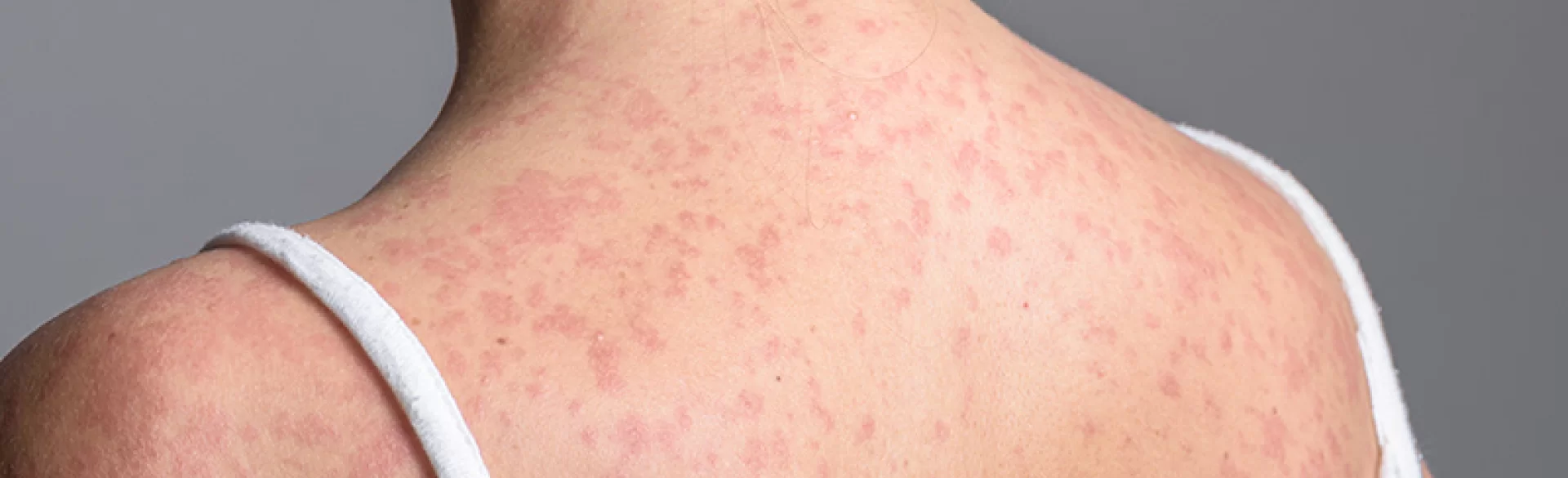
The rash in measles is maculopapular, which means the presence of both flat macules and small raised papules. Lesions are usually intensely red and over time may merge together, forming larger erythematous patches.
Typical features of the measles rash include:
- onset on the face, especially behind the ears and at the hairline,
- gradual spread downward – to the neck, trunk, upper and lower limbs,
- coalescence of skin lesions, especially on the face and trunk,
- symmetric distribution of the lesions on the skin,
- associated skin erythema.
The lesions do not contain purulent material or blisters, and therefore are not termed pustules in medical terminology. The rash usually persists for about 4–6 days, after which it gradually fades and may leave transient brown discoloration and fine-scale peeling of the epidermis.
An important sign preceding the rash is the so-called Koplik spots – small, white lesions with a red border that appear on the buccal mucosa. They are considered one of the most characteristic early signs of measles.
Measles rash – course of the disease
Measles develops in stages, and the appearance of a rash is one of the disease's key phases. The incubation period, that is the time from infection to the onset of the first symptoms, usually lasts 10–14 days.
The course of measles can be divided into several phases:
1. Prodromal period (catarrhal)
It lasts about 3–5 days and includes symptoms resembling an upper respiratory tract infection:
- high fever (often >39°C),
- cough,
- runny nose,
- conjunctivitis,
- photophobia,
- general weakness.
In this phase Koplik spots appear on the oral mucosa.
2. Rash phase
After several days of general symptoms a skin rash appears. Its development follows a characteristic sequence:
- day 1 – face and areas behind the ears,
- day 2 – trunk and arms,
- day 3 – lower limbs and feet.
With the appearance of the rash fever often rises again. The skin lesions may coalesce and cover extensive areas of skin.
3. Recovery period
After a few days the rash begins to gradually fade in the same order in which it appeared. The skin may undergo mild desquamation, and post-inflammatory discoloration persists for a short time.
Measles can lead to complications, especially in infants, elderly people and patients with weakened immunity. The most important include:
- pneumonia,
- middle ear infection (otitis media),
- encephalitis,
- subacute sclerosing panencephalitis (SSPE).
Measles pustules – how to alleviate
There is no causal treatment that eliminates the measles virus, therefore therapy is mainly symptomatic and supportive. Management aims to relieve the symptoms of the disease and to prevent complications.
The basic elements of management include:
Symptomatic treatment
- use of antipyretic medications (e.g., paracetamol),
- adequate hydration,
- rest and isolation of the patient,
- maintaining appropriate humidity in the room.
Skin care
Although the measles rash usually does not cause intense itching, the skin may be irritated and sensitive. It is recommended to:
- gentle cleansers without irritating substances,
- light moisturizing preparations that support restoration of the epidermal barrier,
- avoiding overheating of the skin.
Vitamin A supplementation
The World Health Organization (WHO) recommends administration of vitamin A to children with measles because it reduces the risk of complications and severe disease course.
The most effective method of preventing measles remains protective vaccination with the MMR vaccine (against measles, mumps, and rubella), which provides high immunological effectiveness and significantly reduces the occurrence of the disease in the population.