Pityriasis versicolor on the abdomen
back to main page
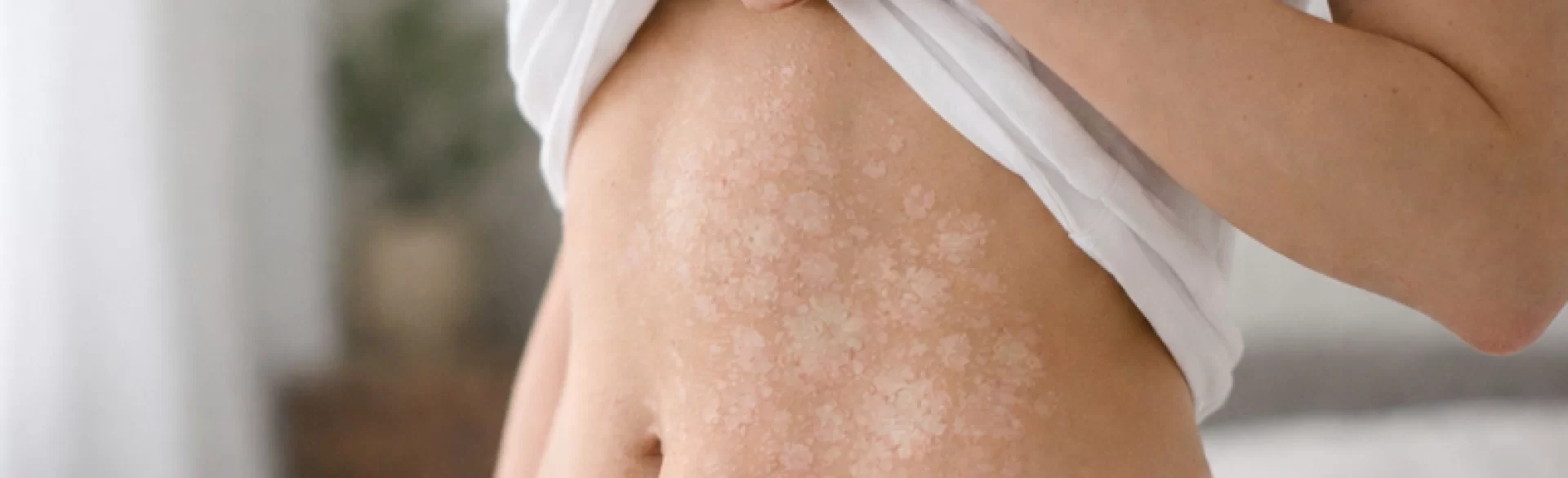
Pityriasis versicolor on the abdomen is a superficial fungal skin infection caused by yeast from the Malassezia genus, which physiologically reside on human skin. Under certain conditions—mainly excessive sebum production, high humidity, and reduced local immunity—these microorganisms become pathogenic, causing pigmentation disorders and skin scaling. The changes most commonly occur on the chest and back, but the abdomen is one of the typical areas affected during the course of the disease. The condition does not pose a systemic threat but is chronic and prone to recurrences, especially during the summer months.
Pityriasis versicolor on the abdomen – causes
The direct cause of pityriasis versicolor is the excessive proliferation of Malassezia furfur yeasts, M. globosa, and related species. Under physiological conditions, they are part of the skin microbiome, but favorable factors can lead to their transformation into a hyphal form and colonization of the stratum corneum of the epidermis.
Predisposing factors:
- excessive sweating (hyperhidrosis),
- warm and humid climate,
- wearing tight, non-breathable clothing,
- seborrheic skin,
- use of greasy occlusive preparations,
- immunosuppression (e.g., treatment with glucocorticosteroids),
- hormonal disorders (puberty, pregnancy).
The pathogenic mechanism involves the production of dicarboxylic acids (including azelaic acid) by Malassezia, which inhibit the activity of melanocytes. This leads to the development of hypopigmentation or hyperpigmentation on the skin, particularly on the abdomen. The process is superficial—the fungi do not penetrate into the deeper layers of the skin.
Contrary to popular belief, pityriasis versicolor is not a classical infectious disease—most people are carriers of Malassezia, and the development of changes depends on individual skin conditions.
Pityriasis versicolor on the abdomen – what it looks like
Skin changes on the abdomen have a characteristic clinical appearance that allows for preliminary diagnosis during a dermatological examination.
Typical features:
- numerous, oval or irregular spots,
- color: light brown, yellowish, pinkish, or depigmented (lighter than the surrounding skin),
- fine, branny scaling visible upon rubbing (sign of "branny scale"),
- tendency to merge into larger patches.
On the abdomen, the changes may be symmetrical and involve the lower parts of the torso. In the summer, after sun exposure, the spots become more noticeable—the healthy skin tans, while the areas affected by the fungus remain lighter (so-called secondary leukoderma).
In diagnosis, the following are helpful:
- examination with a Wood's lamp (yellow-green fluorescence),
microscopic examination of scraping preparations ("spaghetti and meatballs" appearance—hyphae and spores).
Tinea versicolor on the abdomen – symptoms
Pityriasis versicolor typically does not cause severe subjective symptoms, which distinguishes it from many other dermatoses.
Most common symptoms:
- discreet skin scaling,
- sensation of dryness,
- occasionally mild itching (more common with overheating and sweating),
- aesthetic disturbances related to uneven pigmentation.
Lack of pain, erythema, or exudate is typical for this condition. If there is pronounced itching, burning, or inflammation, other differential diagnoses should be considered, including:
- seborrheic dermatitis,
- vitiligo,
- guttate psoriasis,
- dermatophyte infection of smooth skin.
It is worth noting that pigmentary disturbances may persist for several weeks after effective antifungal treatment – this does not indicate an active infection, but rather a temporary dysfunction of melanocytes.
Pityriasis versicolor on the abdomen – treatment
The treatment is local, and in extensive or recurring cases – systemic. The goal of therapy is to eliminate excessive colonization of Malassezia and normalize the skin's microenvironment.
Local treatment (first choice):
- ketoconazole (shampoo or cream),
- ciclopirox,
- terbinafine,
- selenium sulfide,
- zinc preparations.
Shampoo formulations are often applied to entire areas of the torso (including the abdomen), leaving them on the skin for several minutes before rinsing.
Systemic treatment (in selected cases):
- itraconazole,
- fluconazole.
Systemic pharmacotherapy is reserved for resistant, recurrent, or very extensive cases.
Supportive measures:
- wearing breathable clothing,
- avoiding excessive overheating of the skin,
- limiting the use of strongly occlusive preparations,
- periodic antifungal prophylaxis during the summer season for individuals prone to recurrences.
In cases of persistent discoloration after treatment, dermatological procedures improving skin tone uniformity, such as chemical peels or procedures regulating epidermal renewal, can be considered after completely ruling out an active infection.