Plaque psoriasis
back to main page
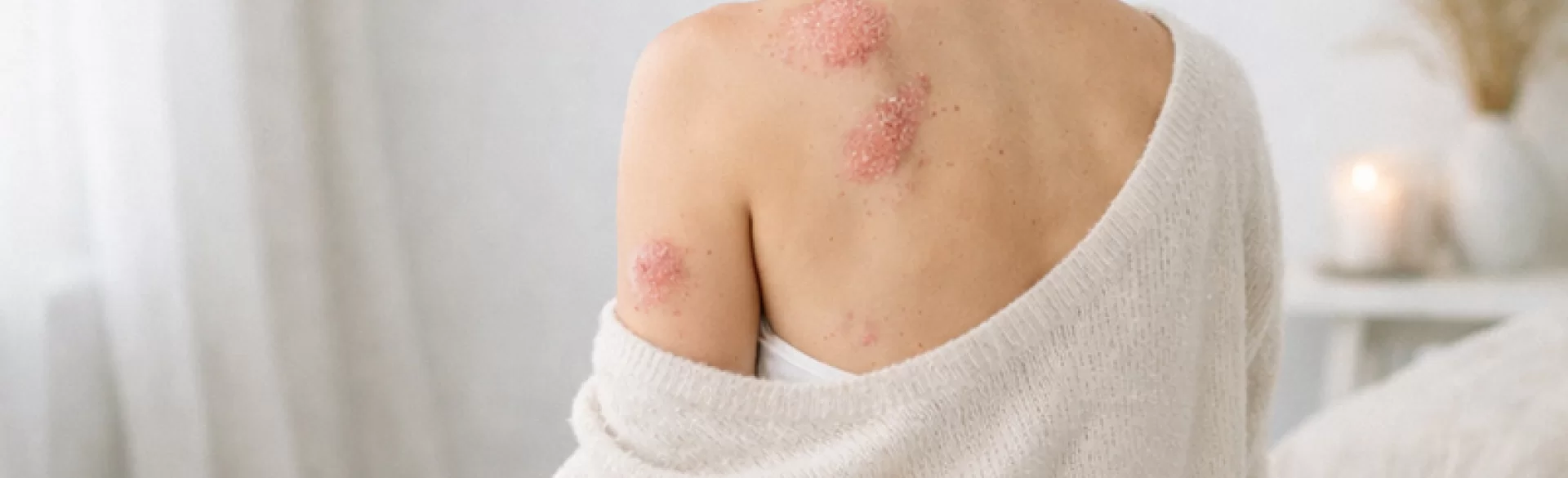
Plaque psoriasis (psoriasis vulgaris) is a chronic, inflammatory, recurrent skin disease with an immunological basis, belonging to the group of autoimmune diseases. It is characterized by an accelerated cycle of keratinocyte proliferation (epidermal cells) and a disrupted immune response, leading to the formation of well-defined, erythematous-scaling plaques. The disease is systemic in nature – in addition to the skin, it may affect the joints (psoriatic arthritis) and is also associated with an increased risk of cardiovascular diseases and metabolic syndrome. The course is variable – ranging from mild, limited lesions to generalized forms requiring systemic treatment.
Plaque psoriasis – causes
The etiopathogenesis of plaque psoriasis is complex and multifactorial. A critical role is played by the abnormal activation of T lymphocytes (especially Th1 and Th17 subpopulations), which produce pro-inflammatory cytokines, including TNF-α, IL-17, and IL-23. These mediators stimulate excessive proliferation of keratinocytes and maintain chronic inflammation within the skin.
The most important predisposing factors include:
1. Genetic predisposition
- Familial occurrence (higher frequency among first-degree relatives).
- Associations with HLA-Cw6 tissue compatibility antigens.
2. Immunological factors
- Overactivity of the IL-23/IL-17 axis.
- Imbalance between pro-inflammatory and anti-inflammatory cytokines.
3. Environmental trigger factors
- Mechanical skin injuries (Koebner phenomenon),
- Infections (especially streptococcal),
- Chronic psychological stress,
- Smoking and excessive alcohol consumption,
- Certain medications (β-blockers, lithium, interferons).
4. Metabolic factors
- Obesity,
- Insulin resistance,
- Dyslipidemia.
Nowadays, psoriasis is considered a systemic inflammatory disease rather than just a dermatological issue.
Plaque psoriasis – symptoms
The most characteristic symptom is erythematous (reddened), well-demarcated plaques covered with silvery-white scales. The lesions most commonly occur:
- on the elbows and knees,
- in the sacral area,
- on the scalp,
- on the nails.
Typical clinical features:
- Stearin candle sign – intense scaling upon rubbing.
- Auspitz sign – pinpoint bleeding after scraping off the scale.
- Koebner phenomenon – appearance of lesions at the site of injury.
The lesions may be accompanied by:
- itching,
- skin tightness,
- burning sensation.
In advanced cases:
- involvement of the nails (onycholysis, pitting),
- joint symptoms (pain, swelling, morning stiffness),
- reduced quality of life and psychological disorders (depression, anxiety).
The severity of the disease is assessed, among other things, using the PASI (Psoriasis Area and Severity Index) scale, which takes into account the extent and intensity of the lesions.
Plaque psoriasis – treatment
Treatment is tailored individually, depending on the extent of the lesions, their location, the patient's age, and any coexisting diseases.
1. Topical treatment (mild and moderate form)
- topical glucocorticosteroids,
- vitamin D₃ analogs (calcipotriol),
- calcineurin inhibitors,
- tars and keratolytic preparations (salicylic acid),
- emollients.
2. Phototherapy
- UVB 311 nm (narrowband),
- PUVA (psoralen + UVA).
Phototherapy exhibits immunomodulating effects and reduces keratinocyte proliferation.
3. Systemic treatment (moderate and severe form)
- methotrexate,
- cyclosporine,
- acitretin,
- biologic drugs (TNF-alpha inhibitors, IL-17, IL-23).
Biologic therapies represent a breakthrough in treating severe forms of psoriasis—they act selectively on specific inflammatory cytokines, showing high efficacy and good tolerance.
4. Supportive treatment
- weight reduction,
- treatment of coexisting diseases,
- psychological support.
The aim of therapy is not only the remission of skin lesions but also the reduction of systemic inflammation.
Treatments for plaque psoriasis
During periods of remission or in mild forms of the disease, supportive treatments can be used to improve patient comfort and support skin regeneration. However, irritating procedures should be strictly avoided during the active phase.
Treatments supporting skin condition:
- gentle moisturizing treatments and rebuilding the hydrolipid barrier,
- soothing therapies using anti-inflammatory preparations,
- LED light treatments (anti-inflammatory and regenerative effects),
- individually tailored dermatological care.
In clinical practice, particular importance is given to:
- rebuilding the epidermal barrier,
- limiting TEWL (transepidermal water loss),
- reducing inflammation.
Every aesthetic procedure should be preceded by a dermatological qualification, as mechanical trauma may trigger new disease lesions (Koebner phenomenon).