Psoriasis of the hands
back to main page
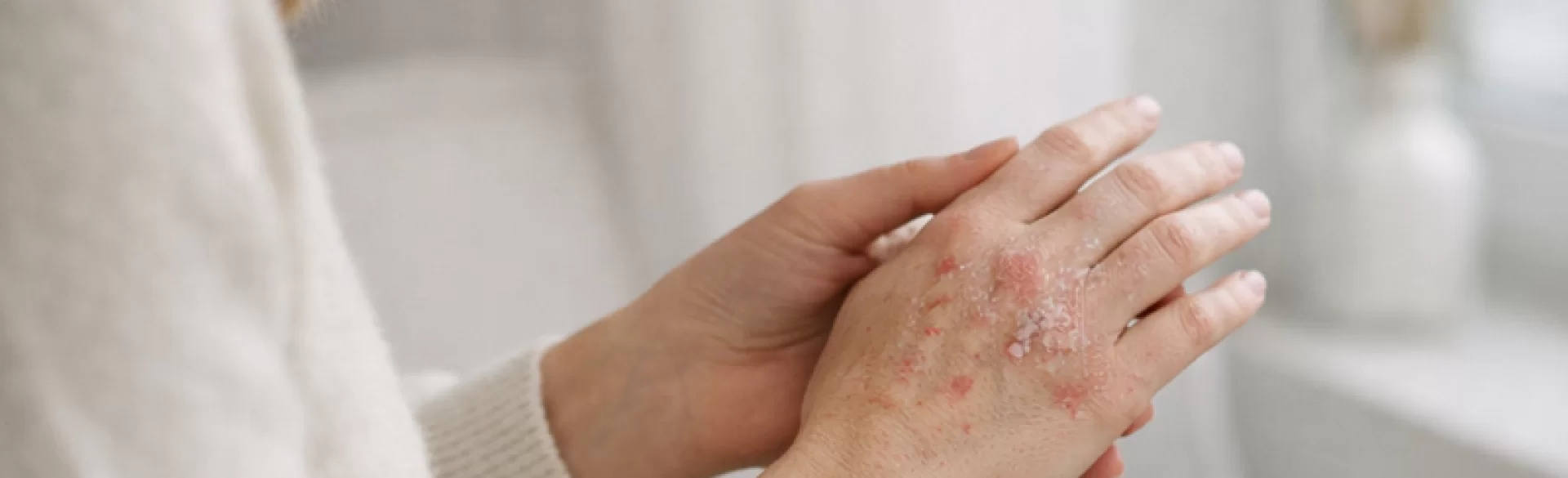
Psoriasis of the hands is a chronic, inflammatory skin disease with an immunological basis, affecting the palmar surface of the hands, often involving the fingers and nail folds. It is part of the spectrum of common psoriasis (psoriasis vulgaris), but due to its location, it poses a significant functional and occupational problem. Skin changes in this area are particularly troublesome - the skin of the hands is thicker, subjected to continuous pressure and microtrauma, which promotes exacerbations. The disease is recurrent, and its course varies individually. The pathogenesis involves immune response disorders with excessive activation of T lymphocytes and accelerated proliferation of keratinocytes, leading to excessive keratinization of the epidermis.
Psoriasis of the hands – the beginnings
Initial symptoms of psoriasis on the hands are often mistaken for contact eczema or atopic dermatitis. The early stage of the disease may have a subtle character, which delays correct diagnosis.
The most common early symptoms include:
- localized erythematous patches (redness of the skin) with clearly defined edges,
- dryness and roughness of the epidermis,
- small areas of excessive keratinization,
- a feeling of skin tightness,
- periodic itching or burning.
On the hands, changes may appear as:
- plaque psoriasis (with plaques covered by silvery scales),
- pustular psoriasis of the hands (palmoplantar pustulosis) – with sterile pustules on an erythematous base,
- hyperkeratotic form – with massive, cracking keratinization.
Factors that initiate or exacerbate lesions include:
- microtrauma (the so-called Koebner phenomenon),
- chronic chemical irritation (detergents, disinfectants),
- psychological stress,
- bacterial or viral infections,
- tobacco smoking (especially in the pustular form).
Early dermatological intervention is important to limit the development of chronic changes and skin cracks, which are common and painful in this location.
Psoriasis of the hands - is it contagious?
Palm psoriasis is not a contagious disease and does not spread through direct contact, touch, or shared use of objects. It is an autoimmune disease with a strong genetic and environmental basis.
Key facts:
- absence of an infectious agent as the cause of the disease,
- no possibility of transmission through skin contact,
- no epidemiological threat in the work environment or family.
The pathogenesis of psoriasis includes:
- activation of the IL-23/Th17 immune axis,
- increased production of pro-inflammatory cytokines (including TNF-α, IL-17, IL-22),
- acceleration of the keratinocyte proliferation cycle (shortening from approximately 28 days to 3–5 days).
Due to the visible changes on the hands, patients often experience social stigma. Educating the surrounding environment and clearly communicating the non-contagious nature of the disease are of significant psychological importance.
Psoriasis of the hands – symptoms
The clinical picture depends on the form of the disease and its stage of advancement. Characteristic features include:
Skin changes:
- Erythematous plaques with clear demarcation,
- Silvery-white scales (though they may be less visible on the palms due to the thickness of the epidermis),
- Intensified hyperkeratosis (keratin thickening),
- Painful skin fissures,
- Pustular lesions (in the pustular form).
Subjective symptoms:
- Itching with varying intensity,
- Burning sensation,
- Painfulness when bending fingers,
- Limitation of manual dexterity.
In some cases, the following coexist:
- Nail changes (pitting, onycholysis),
- Psoriasis in other locations (elbows, knees, scalp),
- Symptoms of psoriatic arthritis.
Diagnosis is primarily based on the clinical picture. In doubtful cases, a histopathological examination is performed, which shows, among other things, acanthosis, parakeratosis, and inflammatory infiltration in the dermis.
Psoriasis of the hands – treatment
Treatment of hand psoriasis is complex and depends on the severity and clinical form of the disease. Due to the thickness of the skin on the hands, topical therapy requires appropriate selection of preparations and their proper application.
Topical Treatment
- Glucocorticosteroids with moderate to high potency,
- Vitamin D₃ analogs (e.g., calcipotriol),
- Vitamin A derivatives (tazarotene),
- Keratolytic agents (urea, salicylic acid),
- Emollients that restore the skin barrier.
Phototherapy
- UVB 311 nm – effective in chronic forms,
- PUVA – in selected resistant cases.
Systemic Treatment (in moderate to severe forms)
- Methotrexate,
- Ciclosporin,
- Acitretin,
- Biological therapies (TNF-α inhibitors, IL-17, IL-23).
In clinical practice, it is important to:
- Avoid irritating factors,
- Protect the skin with gloves (while ensuring ventilation),
- Regularly moisturize the skin,
- Reduce stress.
In supportive therapy for regenerating the skin of the hands, procedures that improve its condition and skin barrier function can be considered, such as individually tailored medical chemical peels, regenerative treatments using platelet-rich plasma, or LED light therapies, always as a complement to dermatological treatment, not as a substitute.
Hand psoriasis requires long-term, consistent management. The aim of therapy is not only to reduce skin lesions but also to improve the patient's quality of life and functional ability.