Pustular pimples on the hands
back to main page
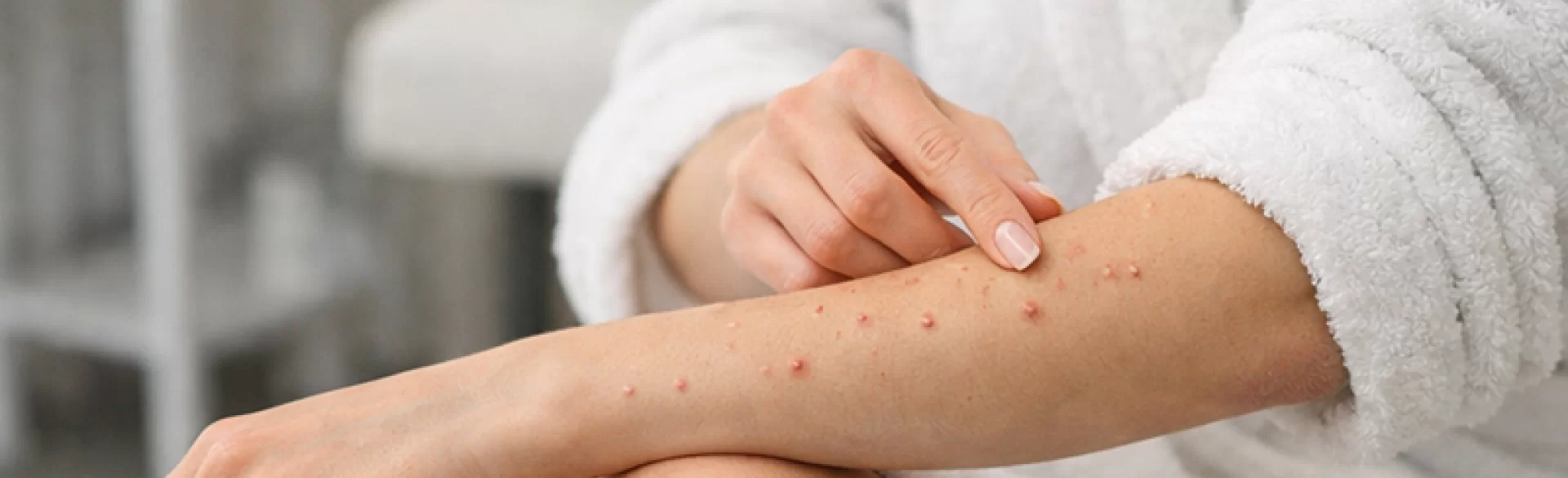
Pustular pimples on the hands are inflammatory skin lesions filled with purulent content, forming within the epidermis or hair follicles. In medical terminology, they are referred to as pustules (pustulae) and are indicative of an ongoing inflammatory process, most often bacterial in nature. These lesions can occur singly or multiple, involving the palms, backs of the hands, fingers, and wrist areas. Depending on the cause, they may be accompanied by pain, redness, swelling, itching, and sometimes systemic symptoms. Pustular pimples are not a disease entity in themselves but a symptom of many dermatological and systemic conditions, thus requiring differentiation and proper diagnosis.
Pustular bumps on hands - causes
The etiology of pustular eruptions on the hands is diverse and includes both infectious and inflammatory or autoimmune factors.
1. Bacterial Infections
The most common causes are infections caused by:
- Staphylococcus aureus
- Streptococcus pyogenes
The most common clinical forms include:
- Impetigo - superficial blisters and pustules with honey-yellow crusts
- Folliculitis - pustules located around the hair follicle
- Furuncles - deeper, painful inflammatory infiltrates
Predisposing factors:
- microtrauma to the skin,
- excessive sweating,
- insufficient hygiene,
- immunosuppression,
- diabetes.
2. Contact Dermatitis and Superinfection
The hands are particularly exposed to contact with:
- detergents,
- disinfectants,
- chemicals,
- occupational allergens.
In the course of contact dermatitis, the damaged epidermal barrier favors secondary bacterial superinfection, leading to the formation of pustular lesions.
3. Inflammatory and Autoimmune Diseases
- Palmoplantar pustulosis - sterile pustules on an erythematous base
- Hidradenitis suppurativa - less common on hands, more common in skin folds
- Drug reactions (e.g., acute generalized exanthematous pustulosis - AGEP)
In palmoplantar pustulosis, the content of the pustules is sterile (without bacteria), and the process is immunological.
4. Changes in the Course of Systemic Diseases
Pustular eruptions may occur more frequently in individuals with:
- diabetes,
- immune disorders,
- chronic inflammatory diseases,
- nutritional deficiencies (e.g., zinc).
Accompanying Symptoms
- pain and tenderness,
- itching or burning,
- swelling,
- local skin warmth,
- in more severe cases: fever and lymph node enlargement.
Differential diagnosis includes herpes, dyshidrotic eczema, fungal infections, or blistering diseases.
Purulent pimples on hands - treatment
Therapeutic management depends on the cause of the changes and their extent.
1. Topical treatment
In mild cases, the following are used:
- antiseptic preparations (octenidine, chlorhexidine),
- antibiotic ointments (mupirocin, fusidic acid),
- topical glucocorticosteroids (in case of inflammatory background),
- zinc preparations with a drying effect.
It is important to:
- avoid squeezing the changes,
- keep the skin clean,
- protect against further irritation.
2. General treatment
Indicated in cases of:
- numerous changes,
- recurrent infections,
- general symptoms.
This may include:
- oral antibiotic therapy (after culture and antibiogram),
- immunomodulating treatment (e.g., in psoriasis),
- control of coexisting diseases (e.g., diabetes).
3. Surgical management
In cases of:
- boils,
- abscesses,
- deep changes,
surgical incision and drainage may be necessary.
In the therapy of chronic changes and in supporting skin regeneration, procedures that improve the epidermal barrier and microcirculation, such as:
- INDIBA® – radiofrequency therapy supporting repair processes,
- LED light treatments with anti-inflammatory effects,
- specialist dermatological procedures improving skin healing.
4. Prevention
- use of protective gloves when working with detergents,
- regular moisturizing of the skin with emollients,
- avoiding mechanical injuries,
- monitoring glucose levels in patients with diabetes,
- prompt treatment of the first signs of inflammation.
In the case of changes persisting for more than 7–10 days, increased pain, spreading inflammation, or general symptoms, a dermatological consultation is necessary. Untreated bacterial infections can lead to complications, including cellulitis or scarring.

