Seborrheic pimples
back to main page
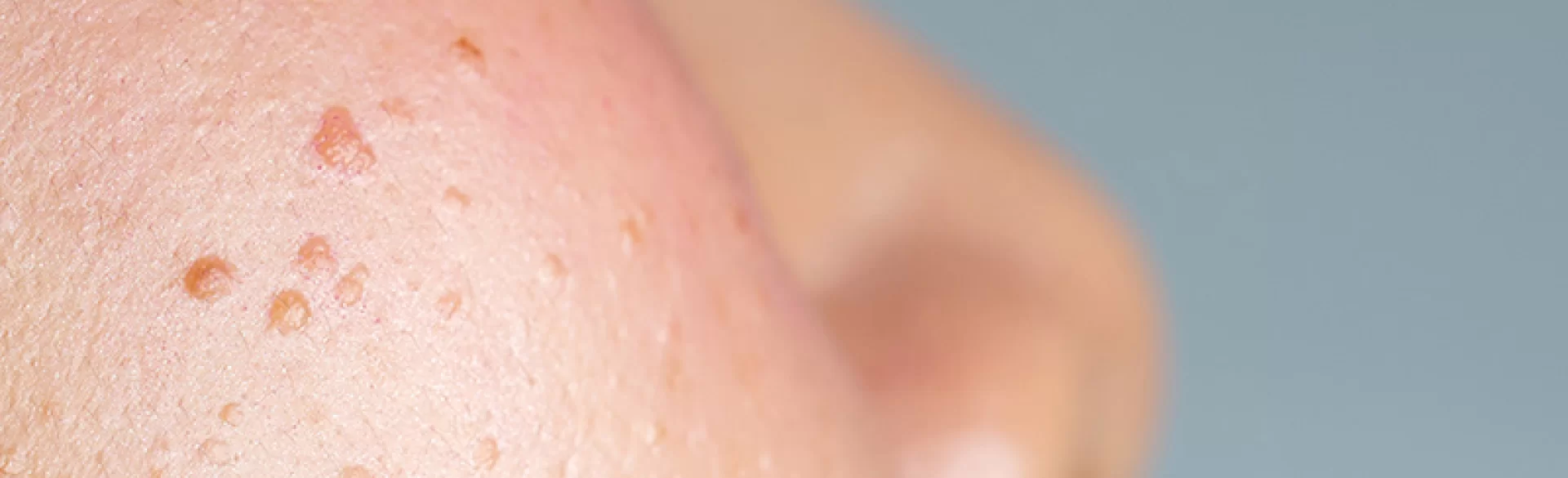
Seborrheic pimples are one of the most common manifestations of sebaceous gland dysfunction, leading to excessive sebum production and the formation of inflammatory and non-inflammatory skin lesions. This phenomenon is most commonly associated with acne vulgaris, but it can also occur as an isolated form of seborrheic disorder. These pimples develop as a result of complex interactions between sebum overproduction, impaired keratinization of the hair follicle openings, and microbial activity, especially Cutibacterium acnes. These lesions are primarily located in areas with high sebaceous gland activity, such as the face, chest, and back.
Seborrheic pimples – what they look like
Seborrheic pimples take on a diverse clinical morphology, depending on the severity of the disorders and the presence of inflammation. The primary feature is the coexistence of comedonal lesions (open and closed) and inflammatory lesions.
The most commonly observed forms include:
- open comedones (blackheads) – dark spots resulting from the oxidation of keratin and lipids in the opening of the hair follicle,
- closed comedones (whiteheads) – small, white bumps under the skin surface,
- papules (papules) – raised, red inflammatory lesions without purulent content,
- pustules (pustules) – lesions containing visible purulent content,
- inflammatory nodules – deeper, painful infiltrates with a higher intensity of inflammatory reaction.
A characteristic feature of skin with seborrheic pimples is:
- excessive shining (“oily skin” effect),
- dilated openings of the sebaceous glands,
- thickening of the stratum corneum of the epidermis,
- uneven skin texture.
These lesions are most often located in the so-called seborrheic zone (T-zone), covering the forehead, nose, and chin, but can also occur on the cheeks, back, and cleavage. In a chronic course, they can lead to the formation of post-inflammatory hyperpigmentation and atrophic scars.
Seborrheic pimples – causes
The pathogenesis of seborrheic pimples is multifactorial and includes both endogenous (internal) and exogenous (external) factors. Hyperactivity of the sebaceous glands and keratinization process disorders play a key role.
The main causes include:
1. Overproduction of sebum (seborrhea)
Sebaceous glands produce excessive amounts of sebum under the influence of androgens (e.g., testosterone and its derivatives). Sebum provides an environment conducive to bacterial growth and clogging of hair follicle openings.
2. Keratinization disorders
Excessive keratinization of epidermal cells (hyperkeratosis) occurs, leading to the clogging of hair follicle openings and the formation of comedones.
3. Microbiological activity
The bacterium Cutibacterium acnes breaks down sebum into free fatty acids, initiating inflammation and intensifying the skin's immune response.
4. Hormonal factors
- puberty,
- hormonal disorders (e.g., hyperandrogenism, polycystic ovary syndrome),
- hormonal fluctuations in the menstrual cycle.
5. Genetic predisposition
An inherited tendency for seborrhea and keratinization disorders significantly increases the risk of developing lesions.
6. Environmental and lifestyle factors
- high glycemic index diet,
- consumption of dairy products (in some cases),
- stress (effect on the hypothalamic–pituitary–adrenal axis),
- improper skin care (comedogenic cosmetics, excessive drying).
7. Medications and external substances
Certain preparations (e.g., corticosteroids, androgens) can aggravate seborrhea and promote the formation of acne lesions.
From a pathophysiological point of view, the interaction of these factors is crucial, leading to chronic inflammation within the pilosebaceous unit.
Seborrheic pimples – how to treat
Treatment of seborrheic pimples requires a multi-directional approach, including dermatological therapy, proper care, and lifestyle modification. The therapeutic strategy depends on the severity of the lesions.
1. Topical treatment (topical therapy)
It forms the basis of therapy in mild and moderate forms:
- retinoids (e.g., adapalene, tretinoin) – normalize the keratinization process and unblock follicle openings,
- azelaic acid – has anti-inflammatory and antibacterial effects,
- benzoyl peroxide – reduces the population of C. acnes bacteria,
- topical antibiotics (e.g., clindamycin) – used in combination therapy.
2. General treatment (systemic)
In more advanced cases:
- oral antibiotics (e.g., doxycycline) – anti-inflammatory and antibacterial action,
- oral isotretinoin – strong sebostatic effect (inhibition of sebum production),
- hormonal therapy (e.g., hormonal contraception in women) – regulation of androgen influence.
3. Dermatological care
Proper care is an integral part of treatment:
- use of non-comedogenic products,
- regular, gentle skin cleansing,
- avoiding excessive degreasing of the skin (which can intensify secondary seborrhea),
- use of products regulating sebum secretion.
4. Aesthetic medicine procedures and procedural dermatology
Modern dermatology uses methods that support treatment and improve skin quality:
- chemical peels (e.g., salicylic, mandelic acid, TCA) – exfoliation of the epidermis and unblocking of pores,
- manual and cavitation skin cleansing – removal of blackheads,
- light therapies (LED) – anti-inflammatory and bactericidal action,
- mesotherapy – improvement of skin function and its regeneration,
- treatments regulating the function of sebaceous glands.
The mechanism of action of the above methods is mainly based on:
- reduction of hyperkeratosis,
- normalization of sebum secretion,
- reduction of inflammation,
- improvement of the skin microenvironment.
5. Lifestyle modification
- low glycemic index diet,
- stress reduction,
- proper skin hygiene,
- avoiding manipulation of lesions (which limits the risk of scarring).
In clinical practice, the greatest effectiveness is achieved through combination therapy, combining pharmacological treatment with procedural interventions and conscious skin care.