Fungal infection of the scalp
back to main page
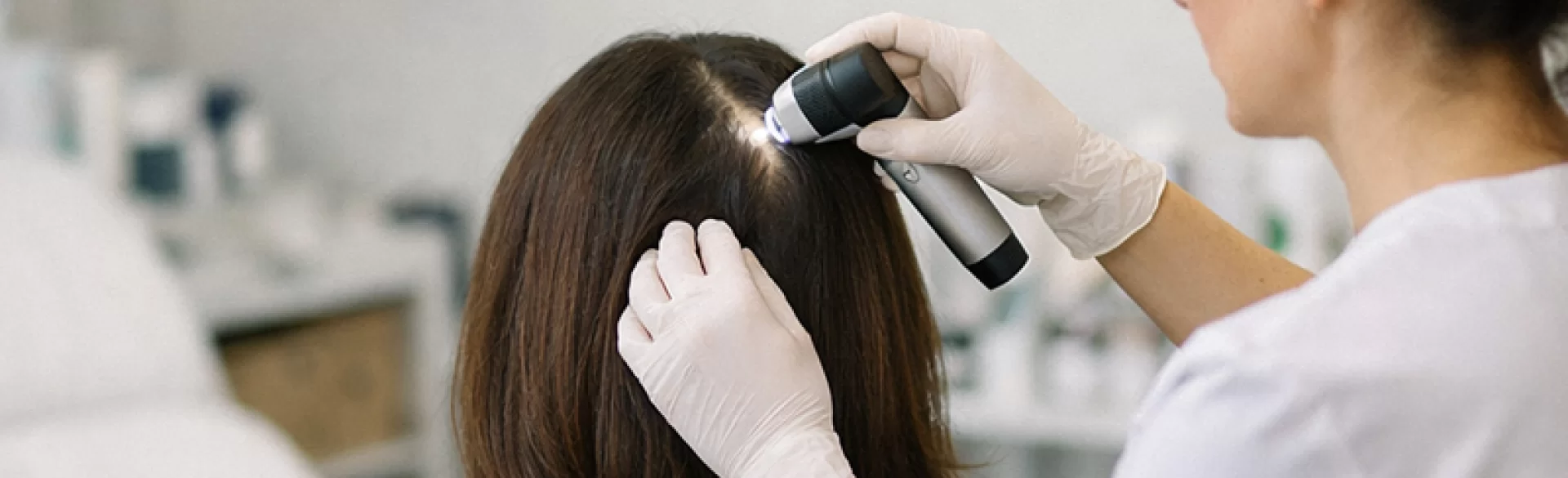
Ringworm of the scalp (tinea capitis) is a dermatophyte infection involving the scalp and hair follicles. The disease primarily affects preschool and school-aged children, but it can also occur in adults, especially those with weakened immune systems. The etiological agent is dermatophytes – keratinophilic fungi capable of decomposing keratin, which is the main protein that makes up the epidermis and hair. The infection leads to hair shaft damage, areas of hair loss, and an inflammatory reaction of varying intensity. Untreated ringworm can result in permanent hair loss due to scarring. Diagnosis is based on clinical examination and mycological confirmation.
Fungal infection of the scalp – causes
The disease-causing factor is dermatophytes from the genera:
- Trichophyton (e.g., T. tonsurans, T. violaceum)
- Microsporum (e.g., M. canis)
- less commonly Epidermophyton
The source of infection can be:
- anthropophilic – transmitted between humans (most common in schools and kindergartens),
- zoophilic – after contact with an infected animal (cats, dogs, rodents),
- rarely geophilic – from the environment (soil).
Transmission occurs through:
- direct contact with an infected person,
- sharing brushes, combs, hats, towels,
- contact with an infected animal.
Predisposing factors:
- immature immune system (children),
- micro-injuries to the scalp,
- reduced immunity (chronic diseases, immunosuppressive treatment),
- poor hygiene.
In pathogenesis, the key significance lies in the ability of dermatophytes to penetrate the hair follicle and multiply within the hair shaft (endothrix or ectothrix infection type). This causes weakening of the hair structure and its brittleness just above the skin surface.
Scalp ringworm - symptoms
The clinical picture depends on the type of pathogen and the host's immune response. Several forms are distinguished:
1. Superficial form
- scaly, round patches,
- hairs broken at a height of 1–3 mm ("black dots"),
- mild itching,
- no scarring.
2. Microsporic form (most often Microsporum canis)
- clearly demarcated patches,
- hairs broken evenly,
- fluorescence under Wood's lamp.
3. Inflammatory form (kerion)
- painful, infiltrated inflammatory nodule,
- purulent secretion,
- enlarged lymph nodes,
- risk of permanent cicatricial alopecia.
General symptoms (rare):
- low-grade fever,
- malaise.
Differential diagnosis should consider:
- alopecia areata,
- seborrheic dermatitis,
- scalp psoriasis,
- trichotillomania.
Diagnosis is confirmed by:
- direct mycological examination (KOH preparation),
- fungal culture,
- Wood's lamp examination,
- dermatoscopy (characteristic "comma hairs," "corkscrew hairs").
Fungal infection of the scalp – how to treat
Treatment of tinea capitis always requires systemic therapy because topical preparations do not penetrate deeply enough into the hair follicle.
Systemic treatment
Most commonly used medications:
- terbinafine – first-line drug for Trichophyton infections,
- griseofulvin – particularly effective in Microsporum infections,
- itraconazole,
- fluconazole.
Duration of therapy:
- usually 4–8 weeks,
- in inflammatory forms, even longer.
The choice of drug should be based on pathogen identification.
Topical treatment (supplementary)
- antifungal shampoos (ketoconazole, ciclopirox),
- trimming hair in affected areas,
- disinfecting personal items.
Inflammatory form (kerion)
Requires:
- systemic antifungal treatment,
- sometimes short-term glucocorticoid therapy to reduce scarring.
Prevention
- treatment of all household members in case of carrier state,
- monitoring of pets,
- avoiding sharing hygiene items,
- rapid implementation of therapy after diagnosis.
The prognosis is good with early treatment. Delayed therapy in the inflammatory form can lead to permanent hair loss.