Varicose veins behind the knees
back to main page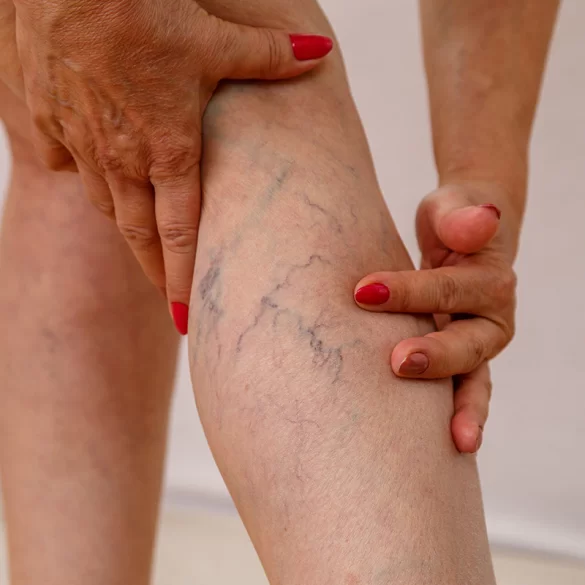
Varicose veins behind the knees are pathologically dilated, elongated, and tortuous superficial veins located in the area of the popliteal fossa and on the posterior surface of the knee. They constitute one of the forms of chronic venous disease (chronic venous disease – CVD), resulting from disturbances in venous blood outflow from the lower limbs. In this location they often involve branches of the small saphenous vein or the great saphenous vein and their numerous tributaries. Due to the specific anatomy of the popliteal fossa and the presence of numerous venous connections, these changes can cause both aesthetic complaints and clinical symptoms, such as a feeling of heaviness in the legs, skin tightness, or pain that worsens during prolonged standing or sitting. Untreated varicose veins can, over time, lead to progression of venous insufficiency.
Varicose veins behind the knees – causes
Varicose veins under the knees develop as a result of disturbances in venous blood outflow from the lower limbs, most often due to venous valve insufficiency. Valves are anatomical structures located inside veins whose role is to prevent the backflow of blood under the influence of gravity. When they become damaged or weakened, blood begins to flow backward (a phenomenon known as venous reflux), which leads to gradual dilation and elongation of the vessel wall.
The popliteal area is particularly predisposed to the formation of varicose veins because important components of the lower limb venous system run there, including the junction of the small saphenous vein to the popliteal vein. If this connection is insufficient, varicose veins may develop on the posterior surface of the knee and in the upper part of the calf.
The most important factors that predispose to the development of varicose veins include:
- genetic predisposition – an inherited weaker structure of the venous wall,
- prolonged standing or sitting, especially in work that requires a static position,
- pregnancy, which causes increased pressure in the veins of the lower limbs,
- overweight and obesity, which increase the load on the venous system,
- low physical activity, leading to weakening of the calf muscle pump,
- hormonal changes, particularly those related to estrogen and progesterone,
- the aging process, which causes loss of elasticity of the venous walls.
In many cases, varicose veins under the knees are part of a broader picture of chronic venous disease, so their appearance should prompt evaluation of the entire venous system of the lower limbs.
Varicose veins behind the knees – symptoms
Varicose veins in the popliteal area may, for a long time, not cause significant complaints and be perceived mainly as an aesthetic problem. However, as the disease progresses, symptoms arise due to increasing venous blood stasis and elevated pressure in the superficial vessels.
The most commonly observed symptoms include:
Local symptoms:
- visible, dilated and tortuous veins behind the knee,
- bluish‑violet discoloration of the vessels,
- a feeling of tightness or pressure in the popliteal fossa,
- tenderness or pain on palpation,
- mild swelling in the area of the knee or the upper calf.
General symptoms of chronic venous insufficiency:
- a feeling of heaviness in the legs that worsens by the end of the day,
- burning or throbbing along the course of the veins,
- nocturnal calf muscle cramps,
- itching of the skin around the varices,
- easy fatigability of the legs during prolonged standing.
A characteristic feature of venous symptoms is their worsening in the standing position and improvement after elevation of the lower limbs. This results from improved venous outflow and decreased pressure in the vessels.
In the differential diagnosis, other conditions that can cause a swelling in the popliteal area should also be considered, such as a Baker's cyst, vascular malformations, or enlarged lymph nodes.
Varicose veins under the knees – what to do
The appearance of varicose veins under the knees requires, above all, proper diagnostics and assessment of the degree of venous system insufficiency. Changes in this area are often the first sign of hemodynamic disorders in the venous system of the lower limbs, so they should not be treated solely as an aesthetic problem.
The basic diagnostic examination is Doppler ultrasound of the lower limb veins, which allows assessment of the direction of blood flow, the competence of venous valves, and the presence of so-called venous reflux (i.e., the backward flow of blood in the veins). This examination makes it possible to determine whether the varicose veins are an isolated lesion or result from insufficiency of larger venous trunks.
In the early stage of the disease, conservative management is recommended, which includes:
- compression therapy (use of compression garments, e.g., compression stockings or knee-high compression socks),
- regular physical activity, particularly walking, swimming, or cycling, which support the so-called calf muscle pump,
- avoiding prolonged standing and sitting, especially with the legs hanging down,
- maintaining a healthy body weight, since overweight increases pressure in the venous system,
- elevating the lower limbs during rest, which facilitates venous blood drainage.
If symptoms worsen, phlebotropic agents (e.g., diosmin, hesperidin, troxerutin) may also be helpful, as they improve venous wall tone and reduce swelling.
It should be emphasized that conservative measures do not remove existing varicose veins, but slow disease progression and limit symptoms. In the case of established changes, procedural methods that close or remove incompetent veins are the most effective.
Varicose veins under the knees – are they dangerous?
Varicose veins behind the knees in many cases initially constitute mainly an aesthetic problem; however, in medical terms they are a sign of chronic venous disease (CVD). This means they may indicate hemodynamic disturbances in the venous system of the lower limbs, related to venous valve insufficiency and impaired blood outflow. Untreated changes can gradually progress and lead to the development of more advanced stages of the disease.
In the first stage of venous disease, varicose veins mainly cause symptoms such as a feeling of heaviness in the legs, tightness in the popliteal area, or intermittent swelling of the lower limbs. Over time, as a result of sustained increased pressure in the venous system, additional symptoms may appear due to chronic blood stasis.
Potential complications of untreated varicose veins include:
- superficial phlebitis – inflammation of the venous wall, which may be accompanied by pain, redness, and hardening of the vessel,
- superficial venous thrombosis, involving the formation of a thrombus within the lumen of the vein,
- chronic lower limb edema, resulting from microcirculation disturbances,
- skin hyperpigmentation caused by deposition of hemoglobin breakdown products,
- lipodermatosclerosis, that is fibrosis of the skin and subcutaneous tissue associated with chronic inflammation,
- in advanced cases venous ulcers of the lower legs.
It is worth emphasizing, however, that not every varicose vein leads to serious complications. Much depends on the degree of venous system insufficiency, the diameter of the affected vessels, and the presence of reflux in larger venous trunks. For this reason, any visible venous change, especially when accompanied by pain or swelling, should be evaluated with a Doppler ultrasound of the lower limb veins.
Early diagnosis of the disease allows for the implementation of appropriate management – from conservative treatment to minimally invasive procedures – which significantly reduces the risk of disease progression and the occurrence of complications.
Varicose veins under the knees – diagnostics
Diagnosis of varicose veins below the knees is based on clinical examination and assessment of the venous system function using imaging studies. A key element of the diagnostics is determining whether the changes are isolated or are part of a more extensive venous insufficiency.
The basic examination is Doppler ultrasonography (Doppler ultrasound) of the lower limb veins, which allows for:
- assessment of the direction of blood flow in the veins,
- detection of venous reflux,
- assessment of deep vein patency,
- identification of incompetent venous valves,
- determination of the source of the varicose veins.
The examination is usually performed in the standing position, because in this position it is easier to visualize flow disturbances and valve insufficiency.
In the diagnosis of chronic venous disease the CEAP classification is also used, which takes into account:
- C (clinical) – clinical signs,
- E (etiological) – the cause of the disease,
- A (anatomical) – the location of changes in the venous system,
- P (pathophysiological) – the mechanism of flow disturbances.
This classification allows standardization of the disease description and facilitates selection of the appropriate treatment method.
In some cases it is also necessary to differentiate varicose veins from other conditions causing symptoms in the knee area, including:
- Baker's cyst,
- deep vein thrombosis,
- venous malformations,
- post-traumatic changes in the soft tissues.
Early diagnosis is crucial because it enables implementation of treatment that prevents disease progression and the development of complications of chronic venous insufficiency.
Varicose veins behind the knees – how to treat
Leczenie żylaków pod kolanami zależy od stopnia zaawansowania choroby, średnicy zmienionych żył oraz obecności refluksu w większych pniach żylnych. Współczesna flebologia preferuje małoinwazyjne techniki zamykania niewydolnych naczyń, które zastąpiły w dużej mierze klasyczne operacje chirurgiczne.
Najczęściej stosowane metody obejmują:
1. Skleroterapię
Skleroterapia polega na podaniu do światła zmienionej żyły specjalnego preparatu obliterującego, który powoduje uszkodzenie śródbłonka i zamknięcie naczynia. W rezultacie krew zostaje przekierowana do prawidłowo funkcjonujących żył.
Metoda ta jest szczególnie skuteczna w przypadku:
- drobnych i średnich żylaków,
- poszerzonych żył siateczkowatych,
- pozostałości żylaków po wcześniejszym leczeniu chirurgicznym.
Odmianą tej techniki jest skleroterapia piankowa, w której lek podawany jest w postaci mikropianki, co zwiększa skuteczność zamykania większych naczyń.
2. Laserowe zamykanie naczyń
W leczeniu niewydolnych żył coraz częściej wykorzystuje się laseroterapię wewnątrznaczyniową, która polega na wprowadzeniu do żyły cienkiego światłowodu emitującego energię laserową. Energia ta powoduje obkurczenie i zamknięcie ściany naczynia.
Technika ta charakteryzuje się:
- wysoką skutecznością terapeutyczną,
- krótkim czasem rekonwalescencji,
- minimalnym ryzykiem powikłań.
W praktyce klinicznej stosuje się również laseroterapię przezskórną, która umożliwia zamykanie mniejszych żylaków i poszerzonych naczyń bez konieczności wprowadzania światłowodu do żyły.
3. Zabiegi chirurgiczne
W bardziej zaawansowanych przypadkach, zwłaszcza gdy obecna jest niewydolność dużych pni żylnych, konieczne może być leczenie chirurgiczne, takie jak:
- miniflebektomia – usunięcie żylaków przez drobne nacięcia skóry,
- stripping żyły odpiszczelowej lub odstrzałkowej – klasyczna metoda chirurgiczna polegająca na usunięciu niewydolnego pnia żylnego.
Obecnie zabiegi te wykonuje się znacznie rzadziej niż w przeszłości, ponieważ coraz częściej zastępowane są technikami małoinwazyjnymi.
W praktyce klinicznej często stosuje się leczenie skojarzone, które polega na zamknięciu głównego źródła refluksu (np. niewydolnego pnia żylnego), a następnie usunięciu pozostałych żylaków przy użyciu skleroterapii lub laseroterapii.
W medycynie estetycznej i flebologii stosuje się również technologie wspomagające leczenie zmian naczyniowych, takie jak laser neodymowo-yagowy (Nd:YAG), który umożliwia zamykanie powierzchownych naczyń żylnych poprzez selektywną fototermolizę hemoglobiny. Energia światła powoduje podgrzanie krwi w naczyniu i jego stopniowe zamknięcie.
W Ambasadzie Urody w terapii zmian naczyniowych stosowane są między innymi:
- laserowe zamykanie naczynek,
- skleroterapia,
- zabiegi laserem Nd:YAG,
które pozwalają na redukcję widocznych żylaków oraz poprawę mikrokrążenia skóry.
Skuteczność leczenia zależy jednak nie tylko od zastosowanej metody, ale również od prawidłowej diagnostyki układu żylnego, indywidualnego doboru terapii oraz stosowania zaleceń profilaktycznych po zabiegu.