Vascular birthmark
back to main page
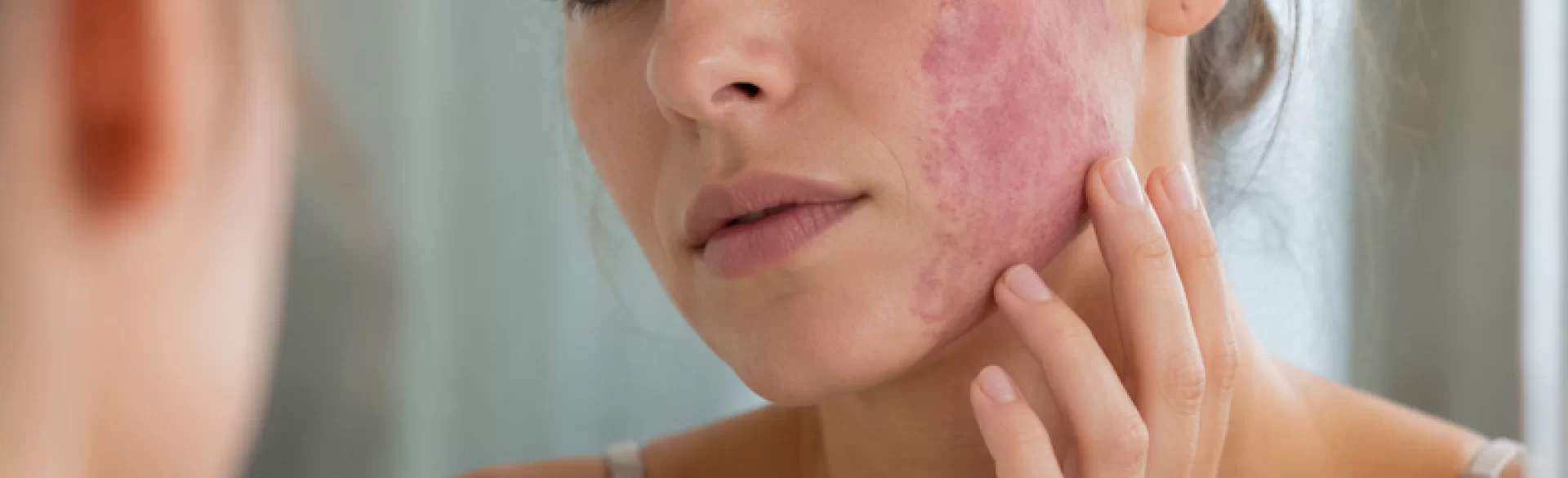
A vascular nevus is a congenital or acquired skin lesion resulting from the abnormal development of blood or lymphatic vessels. It is characterized by the presence of dilated or excessively distributed vascular structures within the dermis, which clinically manifests as a red, pink, purple, or bluish lesion. These lesions can be flat or raised, single or multiple. In most cases, they have a benign course, however, their clinical significance results from both aesthetic aspects and – in selected situations – the possibility of coexisting systemic disorders or progression of the lesion.
Vascular birthmark – location
Vascular birthmarks can occur in any area of the body, however, there are predisposed sites for their appearance, which results from local anatomical and embryological conditions. They are most commonly observed within:
- the face and neck – particularly in the form of flat vascular malformations (so-called port-wine stains),
- the scalp – often in the form of infantile hemangiomas,
- the trunk – lesions of capillary or cavernous hemangioma character,
- upper and lower limbs – including lesions associated with vascular syndromes,
- mucous membrane areas – less common, but may have diagnostic significance.
From a clinical point of view, it is important to distinguish between two main categories of lesions:
- hemangiomas (hemangioma) – proliferative lesions that usually appear in infancy and tend to undergo spontaneous regression,
- vascular malformations – present from birth, they grow proportionally to the organism and do not disappear spontaneously.
The location of the lesion affects its functional and aesthetic significance. Birthmarks within the face can lead to psychosocial disorders, while lesions located in the area of the orbits, nose, or oral cavity can disrupt physiological functions. In the case of extensive malformations, imaging diagnostics (Doppler USG, magnetic resonance imaging) may be necessary to assess the depth and nature of the lesion.
Vascular birthmark – removal
Therapeutic management of vascular birthmarks depends on their type, size, location, and growth dynamics. Modern medicine offers a wide range of methods that allow for the effective and safe treatment of these lesions.
The most important techniques include:
1. Vascular laser therapy
It is the method of choice for treating many superficial vascular lesions. It uses the phenomenon of selective photothermolysis – laser light energy is absorbed by hemoglobin, leading to the closure of pathological vessels without damaging the surrounding tissues. The most commonly used are:
- pulsed dye lasers (PDL),
- Nd:YAG lasers,
- IPL systems (intense pulsed light).
2. Sclerotherapy
It involves injecting an obliterating substance into the vessel lumen, which induces controlled inflammation and vessel closure. The method is used mainly in the case of larger venous malformations.
3. Pharmacological treatment
In selected cases, especially in infants with proliferative hemangiomas, beta-blockers (e.g., propranolol) are used, which inhibit the growth of the lesion and accelerate its regression.
4. Surgical treatment
Reserved for deep, extensive, or treatment-resistant lesions. It involves complete excision of the lesion, often with tissue reconstruction.
5. Radiosurgery and electrocoagulation
Used for small superficial lesions, particularly those of a telangiectasia nature.
In clinical practice, a combined approach is increasingly used, integrating various therapeutic methods to achieve the optimal aesthetic and functional effect.
Within the procedures used in aesthetic medicine and dermatology, the following are available, among others:
- laser vessel closure,
- IPL light therapies,
- treatments using radiofrequency (RF) waves,
- technologies supporting skin regeneration and erythema reduction.
The choice of method should be preceded by thorough diagnostics and assessment of the nature of the lesion, as inappropriate management can lead to complications such as scars, discoloration, or recurrence of the lesion.