Blisters with serous fluid
back to main page
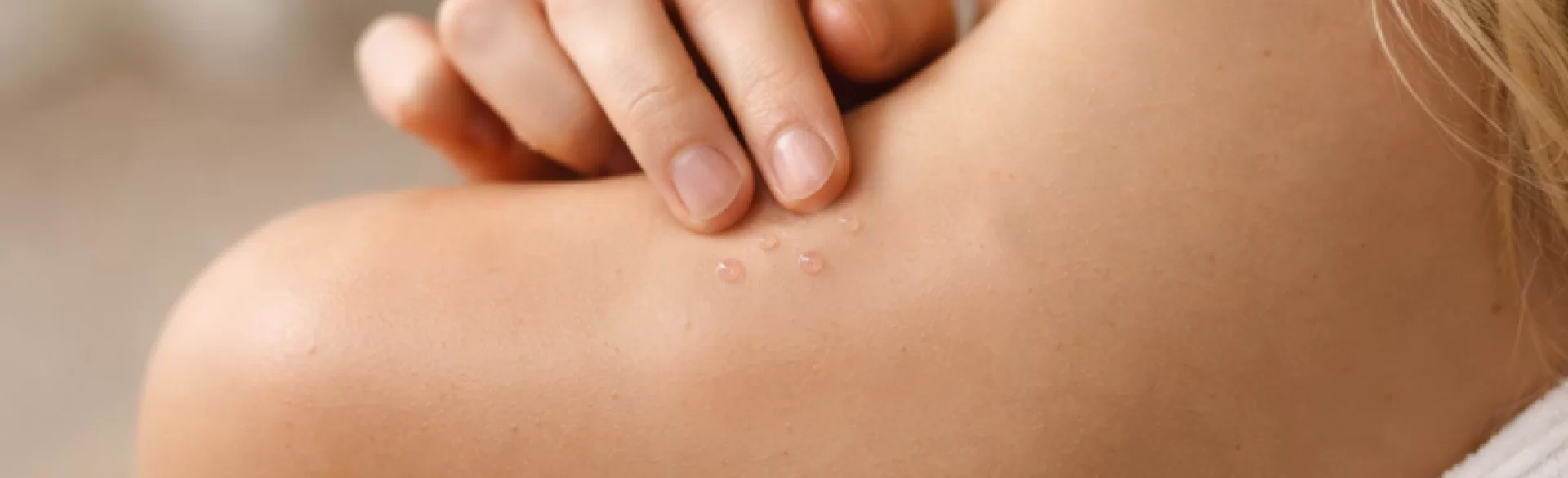
Serous fluid blisters are skin eruptions characterized by vesicles or small blisters filled with a clear or slightly yellowish serous fluid (serum). In dermatology, they are referred to as *vesicles (vesiculae)* if their diameter does not exceed 5 mm, or *bullae (bullae)* when they are larger. The serous fluid is a filtrate of blood plasma that forms as a result of an inflammatory reaction, damage to the epidermal barrier, or immunological disorders. These lesions can accompany both mild inflammatory dermatoses and autoimmune or infectious diseases. Proper assessment of these requires consideration of the location, dynamics of the changes, accompanying symptoms, and clinical history.
Blisters with serous fluid – causes
The formation of fluid-filled blisters is a consequence of:
- damage to intercellular connections in the epidermis (acantholysis),
- separation of the epidermis from the dermis,
- intense inflammatory response with plasma exudation,
- immune reaction against skin structures.
The most common causes include:
1. Inflammatory and allergic diseases
- Contact eczema (allergic or irritant) – a type IV hypersensitivity reaction; blisters often appear on the hands, face, neck.
- Atopic dermatitis (AD) – in the acute phase, small, oozing blisters may appear.
- Dyshidrotic eczema (dyshidrosis) – characteristic, deeply seated blisters on the hands and feet.
2. Infectious diseases
- Herpes simplex (HSV-1, HSV-2) – clusters of painful blisters on an erythematous base.
- Chickenpox – scattered lesions at different stages of development.
- Impetigo (bullous form) – most common in children.
- Blistering reactions in the course of bacterial or fungal infections.
3. Autoimmune blistering diseases
- Bullous pemphigoid – tense blisters in elderly individuals.
- Pemphigus vulgaris – flaccid blisters resulting from acantholysis.
- Dermatitis herpetiformis (Duhring's disease) – small, intensely itchy blisters associated with celiac disease.
4. Physical factors
- Thermal and chemical burns.
- Sunburns.
- Friction and mechanical injury.
Clinically, it is important to distinguish serous from purulent lesions (containing neutrophils) – the presence of cloudy content, pain, and systemic symptoms may suggest bacterial superinfection.
Serous fluid blisters – treatment
Therapeutic management depends directly on the etiology of the changes. Symptomatic treatment without determining the cause may lead to chronicity of the disease process or complications.
1. Local treatment
- Topical glucocorticoids – reduction of inflammation in eczema and atopic dermatitis.
- Calcineurin inhibitors (tacrolimus, pimecrolimus) – alternative for sensitive areas.
- Drying agents (e.g., potassium permanganate solution, octenidine) – for weeping lesions.
- Topical antibiotics – only with confirmed superinfection.
2. Systemic treatment
- Antihistamines for itching.
- Systemic antibiotics – for bacterial infection.
- Antiviral agents (acyclovir, valacyclovir) – in HSV infection.
- Systemic immunosuppression (e.g., corticosteroids, azathioprine) – in autoimmune diseases.
3. Supportive measures
- Protection of the epidermal barrier (emollients with proven reparative effects).
- Elimination of irritant or allergen.
- Avoidance of mechanical damage to blisters – self-puncturing increases the risk of superinfection and scarring.
4. Procedural intervention in case of complications
In cases of persistent inflammatory changes, post-inflammatory hyperpigmentation, or scars from secondary skin damage, supportive regenerative therapies may be implemented:
- Medical peels (TCA acid, AHA/BHA acids) – reduction of hyperpigmentation.
- Fractional laser therapy – skin remodeling in scars.
- Microneedle radiofrequency – stimulation of neocollagenesis.
- Regenerative therapies using platelet-rich plasma (PRP).
In clinical practice, it is crucial to distinguish between transient changes and symptoms of systemic disease. In cases of:
- rapid increase in the number of blisters,
- involvement of mucous membranes,
- presence of fever,
- severe pain,
urgent dermatological consultation and sometimes hospitalization is necessary.