Acne on the back of the neck
back to main page
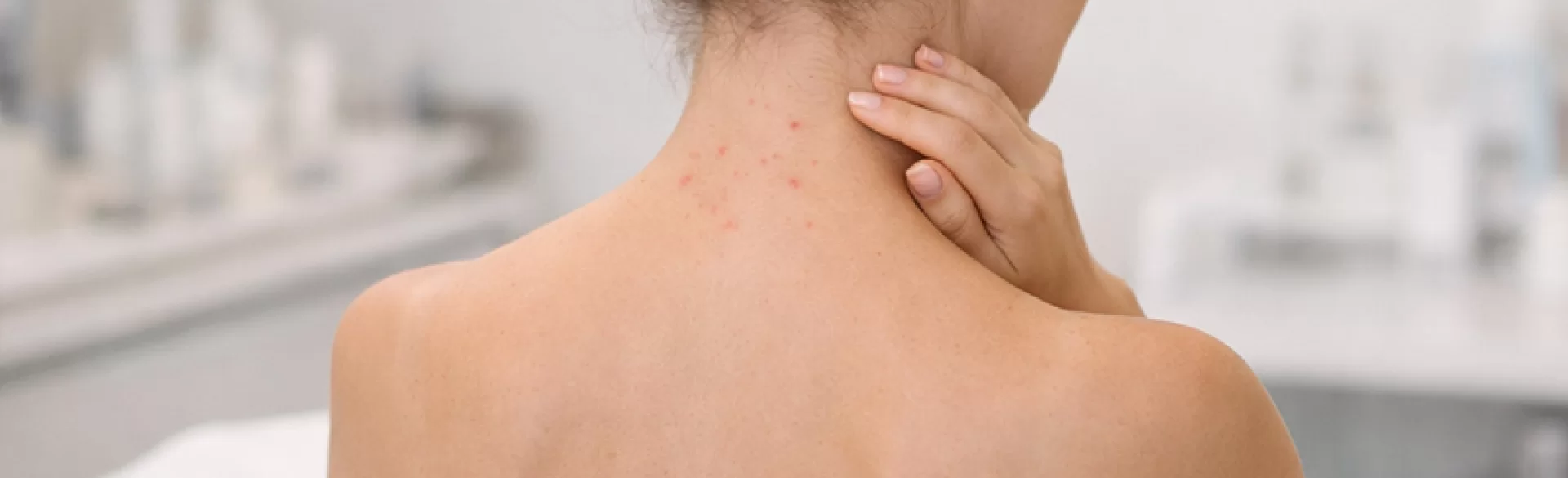
Pimples on the back of the neck are inflammatory skin changes located around hair follicles and sebaceous glands in the nape area. They most commonly appear as papules, pustules, or painful nodules, which can persist chronically and recur. This area is particularly prone to mechanical irritation (collars, turtlenecks, sports equipment), excessive sweating, and bacterial colonization. These changes may be part of common acne, folliculitis, or—in more severe cases—conglobate acne or keloidal folliculitis of the neck (acne keloidalis nuchae). Due to the risk of scarring and discoloration, proper diagnosis and causal treatment are required.
Pimples on the back of the neck – causes
The pathogenesis of inflammatory changes in this location is multifactorial and includes both systemic and local factors.
1. Excessive sebum production (seborrhoea)
- stimulated by androgens (e.g., during puberty, in hyperandrogenism),
- leads to blockage of hair follicle openings.
2. Hyperkeratinization of the hair follicle opening
- excessive keratinization causes the formation of microcomedones,
- promotes the development of inflammation.
3. Bacterial colonization
- mainly by Cutibacterium acnes,
- in folliculitis also by Staphylococcus aureus.
4. Mechanical and environmental factors
- friction (shirt collars, helmets, backpack straps),
- moisture and sweat (environment conducive to bacterial growth),
- lack of proper skin hygiene after physical exertion.
5. Individual predispositions
- thick, seborrheic skin,
- tendency to scarring,
- metabolic disorders (insulin resistance, obesity).
It is important to distinguish classical acne lesions from acne keloidalis nuchae, which is a chronic inflammation of the hair follicles on the neck leading to the formation of hard, hypertrophic scars. This condition is more common in men with short, coarse hair and requires specialized dermatological treatment.
Back of neck acne - how to treat?
Therapeutic management should depend on the severity and nature of the lesions (non-inflammatory, inflammatory, purulent, cicatricial).
1. Topical Treatment
Used in mild and moderate forms:
- Topical retinoids (adapalene, tretinoin) – normalize keratinization and prevent the formation of microcomedones,
- Benzoyl peroxide – has antibacterial and anti-inflammatory effects,
- Topical antibiotics (e.g., clindamycin) – in short cycles, always in combination therapy,
- Products with azelaic acid – reduce inflammation and post-inflammatory hyperpigmentation.
2. Systemic Treatment
In cases of numerous, painful, recurring lesions:
- Oral antibiotics (e.g., tetracyclines),
- Oral isotretinoin – in severe forms of acne,
- Hormonal therapy (in women with confirmed hyperandrogenism).
3. Supportive Measures
- Avoiding pressure and friction around the neck area,
- Quickly drying the skin after physical exercise,
- Using dermocosmetics with sebum-regulating and keratolytic effects,
- Avoiding squeezing lesions (risk of hypertrophic scars).
4. Procedural Treatment
In chronic and recurrent cases, dermatological and aesthetic medicine procedures can be helpful:
- Chemical peels (salicylic acid, mandelic acid, pyruvic acid) – regulate keratinization and seborrhea,
- Laser therapy (e.g., fractional lasers) – reduction of post-inflammatory scars,
- LED light therapy – anti-inflammatory and antibacterial action,
- In cases of cicatricial lesions – injection procedures (e.g., corticosteroids into the scar).
In clinical practice, effective treatment often requires combination therapy – pharmacological and procedural – and the elimination of mechanical factors.