Bacterial pustules
back to main page
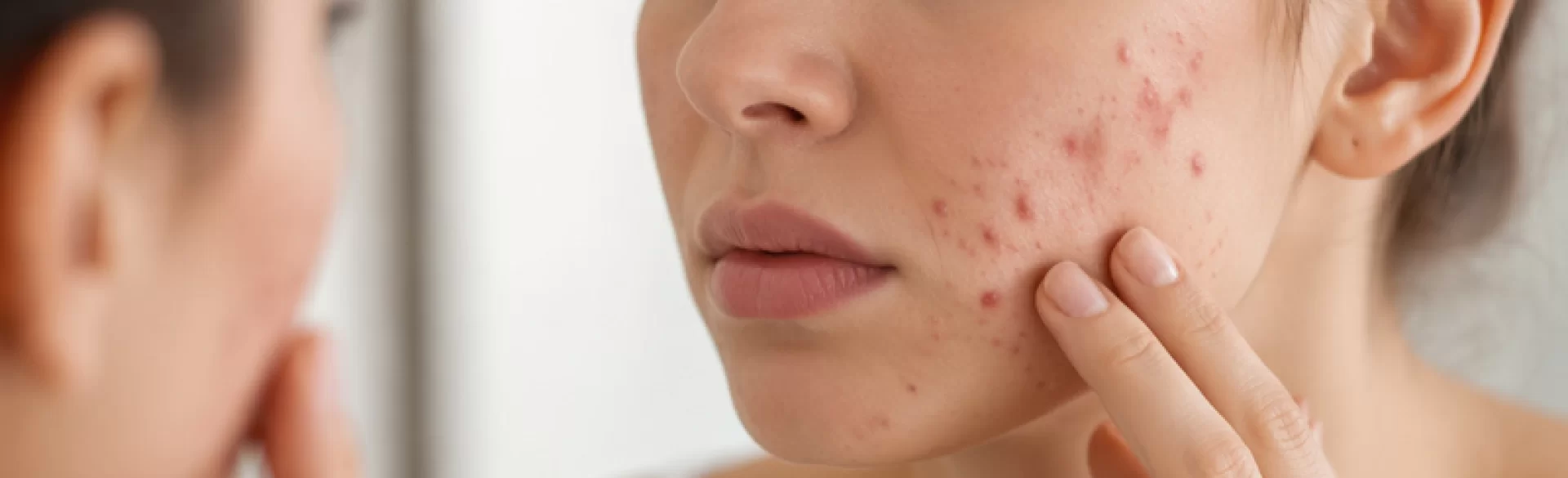
Bacterial pustules are inflammatory skin lesions resulting from a skin infection by bacteria – most commonly Staphylococcus aureus and Streptococcus pyogenes. They take the form of raised eruptions, often filled with purulent content, accompanied by redness, swelling, and pain. They can occur as single or multiple lesions, both superficial and deeper localized. Bacterial pustules represent one of the most common manifestations of skin and skin appendage infections (including hair follicles), and their course and severity depend on the body's immunity and local factors.
Bacterial pustules – what they are
Bacterial pustules belong to the group of primary skin lesions referred to as pustules, i.e., eruptions filled with purulent content. Pus is formed as a result of the body's inflammatory response to the presence of microorganisms and contains leukocytes (mainly neutrophils), bacteria, and fragments of destroyed tissues.
The most common clinical forms of bacterial pustules include:
- folliculitis – superficial infection of the hair follicle opening,
- furuncles (furunculus) – deep, painful inflammatory lesions with tissue necrosis,
- furunculosis – multiple or recurrent furuncles,
- impetigo – superficial infection of the epidermis, especially in children,
- skin abscesses (abscessus) – localized collections of pus in tissues.
The pathogenesis of the lesions includes:
- penetration of bacteria through the damaged epidermis,
- multiplication of microorganisms,
- activation of the immune response,
- development of local inflammation.
Factors predisposing to the formation of bacterial pustules:
- skin micro-traumas (abrasions, scratches, shaving),
- excessive sebum production,
- disturbances of the epidermal barrier,
- chronic diseases (e.g., diabetes),
- reduced immunity,
- improper hygiene or its excess (damage to the skin microbiome).
Bacterial pustules – what they look like
Bacterial pustules have a relatively characteristic clinical presentation, but their appearance may vary depending on the depth of infection and the type of bacteria.
Morphological features of bacterial pustules:
- a lesion elevated above the skin surface,
- presence of yellowish or whitish purulent content,
- surrounding erythema (redness),
- often present edema and pain,
- possible crust formation after the lesion ruptures.
Depending on the type of lesion:
- superficial pustules – small, well-demarcated, located within the follicular orifice,
- boils – larger, hard, painful nodules with a central necrotic core,
- impetigo – vesicles and pustules rapidly transforming into honey-yellow crusts,
- abscesses – deep, tense, painful lesions with a palpable collection of pus.
In the course of bacterial infections, systemic symptoms may also occur:
- elevated body temperature,
- enlargement of regional lymph nodes,
- malaise (in more severe cases).
An important diagnostic aspect is to differentiate bacterial pustules from lesions of other origins:
- acne (where comedones predominate),
- viral lesions (e.g., herpes),
- autoimmune diseases (e.g., pemphigus).
Bacterial pustules – location
Bacterial pustules can occur all over the body; however, there are areas particularly predisposed to their formation due to the presence of hair follicles, sebaceous glands, and conditions conducive to bacterial multiplication.
Most common locations:
1. Face
- areas around the nose, chin, and cheeks,
- areas with increased sebum production,
- often associated with folliculitis or secondary infection of acne lesions.
2. Scalp
- especially in places of mechanical irritation,
- associated with folliculitis.
3. Back and chest
- areas rich in sebaceous glands,
- favorable environment for bacteria (sweat, occlusion).
4. Armpits and groins
- moist areas exposed to friction,
- frequent occurrence of abscesses and boils.
5. Buttocks and thighs
- associated with pressure, occlusion, and micro-injuries,
- frequent folliculitis.
6. Lower limbs
- especially in people with circulatory disorders,
- increased risk of secondary skin infections.
Localization factors increasing the risk of lesions:
- excessive sweating,
- wearing tight clothing,
- chronic skin irritation,
- lack of adequate skin ventilation.
It is worth emphasizing that the location of lesions can have diagnostic significance – for example, recurrent pustules within the armpits and groins may indicate acne inversa (hidradenitis suppurativa), which requires a separate therapeutic approach.
Treatment of bacterial pustules depends on their severity, depth, and cause. The basis is the elimination of infection and the restoration of proper skin barrier function.
General management:
- topical antibacterial preparations (e.g., mupirocin, fusidic acid),
- systemic antibiotic therapy in more severe cases,
- antiseptic agents,
- avoiding manipulation of lesions (risk of infection spread).
Supportive dermatological and aesthetic methods:
- skin cleansing and seboregulating treatments – reduction of the environment conducive to bacteria,
- chemical peels – keratolytic and antibacterial action,
- light therapy (LED, IPL) – anti-inflammatory and bactericidal action,
- laser therapy – reduction of inflammatory lesions and post-inflammatory hyperpigmentation,
- treatments using radiofrequency technology (e.g., INDIBA) – supporting tissue regeneration and reduction of inflammation.
In clinical practice, combined therapies are increasingly used, which allow to:
- shorten treatment time,
- reduce the risk of recurrence,
- improve skin quality after the lesions have subsided.
The choice of therapy should be individual and take into account:
- patient age,
- location of lesions,
- comorbidities,
- severity of infection.