Blackheads between the breasts
back to main page
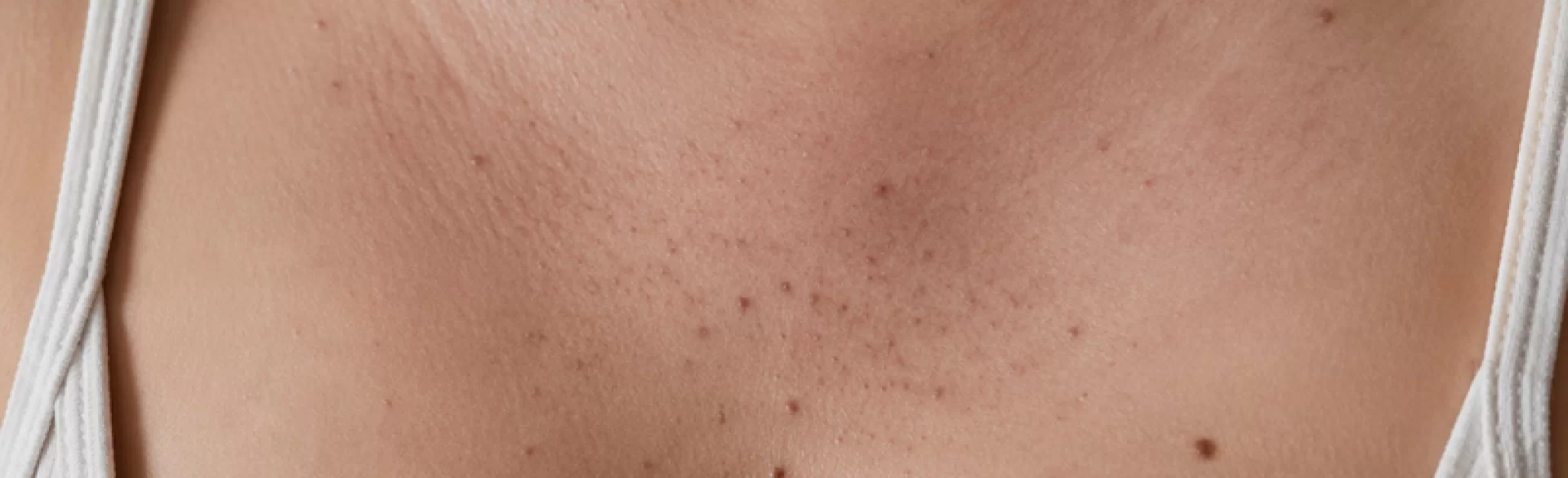
Blackheads between the breasts (open and closed comedones within the sternum and cleavage) are a common dermatological problem associated with dysfunction of the pilosebaceous unit. This area is characterized by a large number of sebaceous glands and specific skin microenvironment conditions, such as increased sweating, friction, and limited ventilation. As a result, there is excessive sebum production, its accumulation in the openings of the hair follicles, and the formation of keratosebaceous plugs. These lesions can be isolated or coexist with truncal acne, posing both an aesthetic and a dermatological problem.
Blackheads between the breasts – why they form
The etiopathogenesis of blackheads in the area between the breasts is multifactorial and involves both internal (endogenous) and external (exogenous) mechanisms. A key role is played by the excessive activity of sebaceous glands and keratinization disorders, i.e., the process of epidermal cornification.
The most important causes include:
1. Sebum overproduction (seborrhea)
Sebaceous glands in the sternal area exhibit high activity, especially under the influence of androgens. Excess sebum promotes the formation of plugs closing the openings of hair follicles.
2. Epidermal keratinization disorders (hyperkeratosis)
Abnormal exfoliation of keratinocytes leads to their accumulation in the openings of sebaceous glands, which initiates the formation of comedones:
- closed comedones (whiteheads),
- open comedones (blackheads), in which the dark color results from the oxidation of melanin rather than the presence of impurities.
3. Microenvironment of the cleavage skin
The area between the breasts favors the development of lesions due to:
- increased humidity (sweat),
- limited air circulation,
- friction between the skin and clothing,
- local overheating.
4. Hormonal factors
Hormonal fluctuations (e.g., in the menstrual cycle, during pregnancy, or in endocrine disorders) intensify sebum production and predispose to the formation of lesions.
5. External factors (comedogenic)
- use of heavy cosmetics (oils, lotions, SPF filters with high comedogenic potential),
- improper skin hygiene or excessive drying,
- wearing tight, synthetic underwear,
- use of perfumes and fragrance products in the cleavage area.
6. Skin microflora
The growth of bacteria, including Cutibacterium acnes, can lead to secondary inflammation and the transformation of blackheads into inflammatory lesions (papules, pustules).
It is worth emphasizing that blackheads in this location are often chronic and recurrent, especially in the presence of coexisting seborrheic skin or acne.
Blackheads between the breasts – cleansing
Therapeutic management in the case of blackheads between the breasts should be comprehensive and include both appropriate home care and dermatological and treatment procedures. The goal of treatment is to normalize sebum secretion, restore the proper keratinization process, and mechanically remove existing lesions.
1. Home care (the basis of therapy)
Daily care should be based on preparations with documented comedolytic (blackhead-dissolving) properties:
Active substances with the highest effectiveness:
- salicylic acid (BHA) – penetrates into the pores, has anti-inflammatory and exfoliating effects,
- retinoids (e.g., retinol, retinal) – regulate keratinization and reduce sebum production,
- azelaic acid – has antibacterial properties and normalizes keratinization,
- niacinamide – reduces seborrhea and has anti-inflammatory effects.
Care principles:
- gentle skin cleansing 1–2 times a day,
- avoiding comedogenic preparations,
- using light, non-occlusive cosmetics,
- regular exfoliation (chemical, not mechanical).
2. Manual and professional cleansing
In the case of persistent lesions, procedures performed in a professional setting are more effective:
Manual skin cleansing
Consists of the mechanical removal of blackheads after prior skin preparation (softening, keratolytic preparations). The procedure requires experience to avoid complications such as hyperpigmentation or scars.
The use of acids (e.g., salicylic, mandelic, glycolic) enables:
- reduction of the stratum corneum,
- unclogging the openings of the sebaceous glands,
- improvement of skin texture.
Mechanical exfoliation of the epidermis that improves pore cleansing and stimulates skin regeneration.
3. Modern supporting methods
In clinical practice, technologies supporting the treatment of comedonal lesions are also used:
- hydrogen cleansing – uses active hydrogen to reduce free radicals and cleanse pores,
- hydrodermabrasion – mechanical-water exfoliation and infusion of active substances,
- Geneo (OxyGeneo) – exfoliation, oxygenation, and improvement of skin functions,
- oxygen infusion – improves skin oxygenation and supports regeneration,
- carboxytherapy – increases microcirculation and cellular metabolism,
- light therapy (LED) – anti-inflammatory and sebum-regulating effects.
4. Dermatological treatment
In more advanced cases, it may be necessary to implement pharmacological treatment:
- topical retinoids (e.g., adapalene),
- preparations with benzoyl peroxide,
- in selected situations, systemic treatment (e.g., oral retinoids).
5. Prevention of recurrence
A long-term therapeutic effect requires the elimination of predisposing factors:
- using breathable, natural clothing,
- avoiding excessive skin overheating,
- regular hygiene of the skin on the décolleté,
- conscious choice of cosmetics (non-comedogenic).
Blackhead reduction in the décolletage area - treatments
In the practice of aesthetic medicine and cosmetology, a number of procedures are used to support the treatment of blackheads in this area. The most frequently used include:
- chemical peels (AHA, BHA acids),
- manual cleansing and hydrogen cleansing,
- microdermabrasion,
- oxygen infusion,
- LED light therapies,
- treatments regulating the activity of sebaceous glands and improving microcirculation.
These procedures allow not only for the reduction of existing lesions, but also for the improvement of skin quality and a reduction in the tendency for their recurrence.