Atrophic scars
back to main page
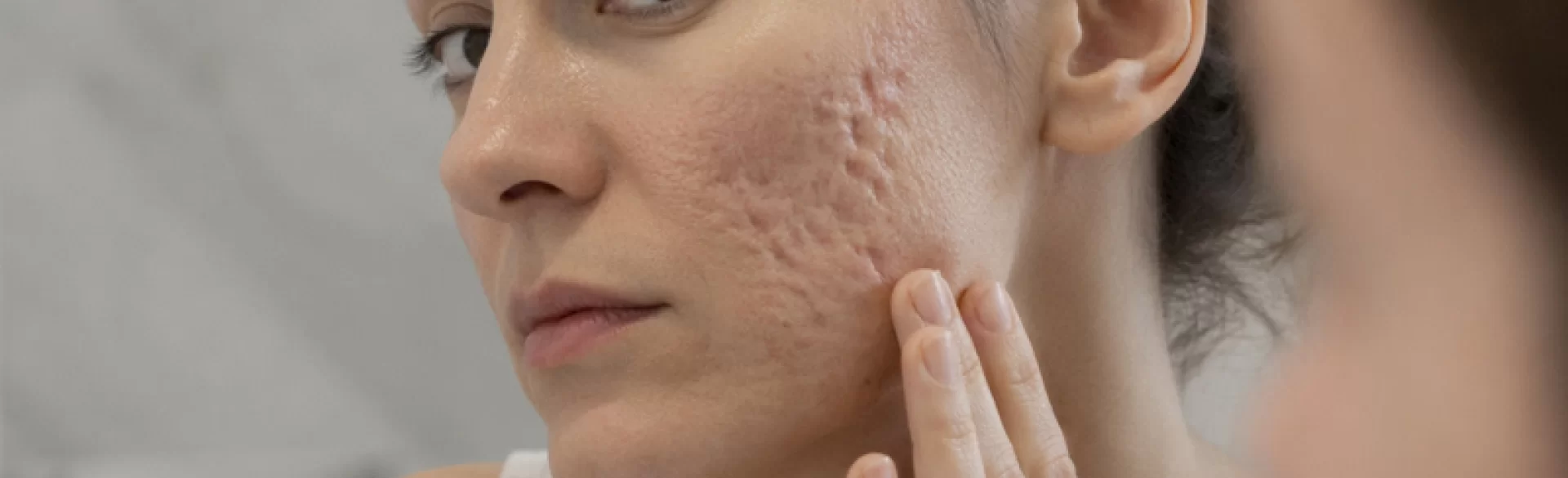
Atrophic scars (atrophic) are permanent skin lesions resulting from an improper healing process in which there is insufficient production of collagen and other components of the extracellular matrix. As a result, the skin at the site of the injury collapses, creating characteristic depressions of various depths and shapes. They are most commonly observed after acne, chickenpox, or mechanical injuries. Atrophic scars represent a significant dermatological and aesthetic problem because they affect the skin's structure, its uniformity, and visual perception, and their spontaneous regression remains limited.
Atrophic scars – what they are
Atrophic scars are the result of an imbalance between collagen degradation and synthesis during the skin healing process. Under physiological conditions, fibroblasts are responsible for tissue reconstruction through the production of type I and III collagen. In the case of atrophic scars, the activity of these cells is insufficient, leading to the formation of defects in the dermis.
Several basic types of atrophic scars are distinguished:
- ice pick – narrow, deep, resembling punctures,
- boxcar – with distinct, sharp edges and a flat bottom,
- rolling – extensive, wavy depressions resulting from fibrous subcutaneous bands.
The most common causes of their formation include:
- inflammatory acne (especially nodulocystic forms),
- viral infections (e.g., chickenpox),
- mechanical and surgical injuries,
- genetic factors affecting skin repair processes.
At the histological level, a reduced density of collagen fibers, disorganization of elastin, and disturbances in the architecture of the dermis are observed. These changes are permanent, which justifies the necessity of implementing therapies that stimulate tissue regeneration.
Atrophic scars – how to remove
Atrophic scar removal is based on the stimulation of skin repair processes and the induction of neocollagenesis, i.e., the formation of new collagen. The key goal of the therapy remains the restoration of tissue volume and evening out the skin surface.
Therapeutic management includes:
- fibroblast stimulation – stimulating cells to produce collagen and elastin,
- skin remodeling – reconstruction of existing collagen fibers,
- improvement of microcirculation – increasing the supply of oxygen and nutrients,
- reduction of fibrous adhesions – releasing the skin from structures causing it to sink.
In clinical practice, a multi-stage approach is used, combining various therapeutic methods. Of significant importance are:
- depth and type of the scar,
- location of the lesions,
- patient's age and the skin's regenerative capabilities.
Therapeutic differences: shallow vs deep scars
Shallow scars:
- affect mainly the epidermis and superficial layers of the dermis,
- respond well to:
- chemical peels,
- non-ablative laser therapy,
- microneedle mesotherapy,
- usually require shorter therapy and fewer treatments.
Deep scars:
- reach deep layers of the dermis,
- often require:
- ablative lasers,
- microneedle radiofrequency,
- subcision,
- combined therapies,
- their treatment is more complex and long-term.
Therapy time and number of treatments
The treatment process is staged and requires consistency:
- microneedle mesotherapy / RF: 3–6 treatments every 4–6 weeks,
- fractional laser: 2–5 treatments every 6–8 weeks,
- medical peels: series of 4–8 procedures,
- subcision: usually 1–3 treatments depending on the severity of the changes.
Full collagen remodeling occurs gradually and can last 3–12 months from the start of therapy.
Real effects of therapy
In clinical practice, the following are achieved:
- shallowing of scars by 30–70%,
- improvement of skin structure and its tension,
- evening out of skin tone.
Complete removal of scars occurs rarely; however, modern therapies enable significant improvement in skin quality and reduction in the visibility of lesions.
Prognosis and factors affecting outcomes
Prognosis depends on:
- age of the scars (fresh ones react better),
- depth of the lesions,
- genetic predispositions,
- lifestyle and skin care.
Factors worsening the condition of scars:
- exposure to UV radiation (collagen degradation),
- manipulation of inflammatory lesions (e.g., squeezing acne),
- chronic skin inflammation,
- smoking tobacco (impaired microcirculation),
- lack of proper care and photoprotection.
Atrophic scars – treatments
Modern treatment of atrophic scars is based on combination therapies that work on multiple levels – from the skin surface to its deep layers.
Comparison of therapeutic methods
| Method | Mechanism of action | Type of scars | Effects |
|---|---|---|---|
| Fractional CO₂ laser | micro-damage + neocollagenesis | deep, boxcar | intense skin remodeling |
| Non-ablative laser | collagen stimulation without damage | shallow, mixed | structural improvement |
| Microneedle RF (Secret RF, Deage EX) | microneedling + thermal energy | rolling, mixed | skin densification and tightening |
| regeneration induction | shallow | texture improvement | |
| controlled exfoliation | shallow, ice pick | skin smoothing | |
| Subcision | release of adhesions | rolling | scar lifting |
| Fillers | volume replenishment | single defects | immediate effect |
Indications: which treatment for which type of scars
- ice pick:
- TCA peels (CROSS technique),
- ablative laser,
- boxcar:
- CO₂ fractional laser,
- microneedle RF,
- rolling:
- subcision,
- microneedle RF,
- combined therapies.
Therapies used in clinical practice
Modern therapeutic protocols include, among others:
- fractional laser therapy – intensive skin remodeling,
- microneedle radiofrequency (Secret RF, Reaction RF) – improvement of tension and structure,
- microneedle mesotherapy – stimulation of regeneration,
- medical peelings – smoothing the skin surface.
The highest effectiveness is achieved by combining technologies, which simultaneously allows to:
- release adhesions,
- stimulate fibroblasts,
- rebuild collagen,
- improve skin quality on many levels.
Choosing the appropriate method requires an individual clinical assessment and often combining several technologies in order to achieve the optimal therapeutic effect.