Puerperium
back to main page
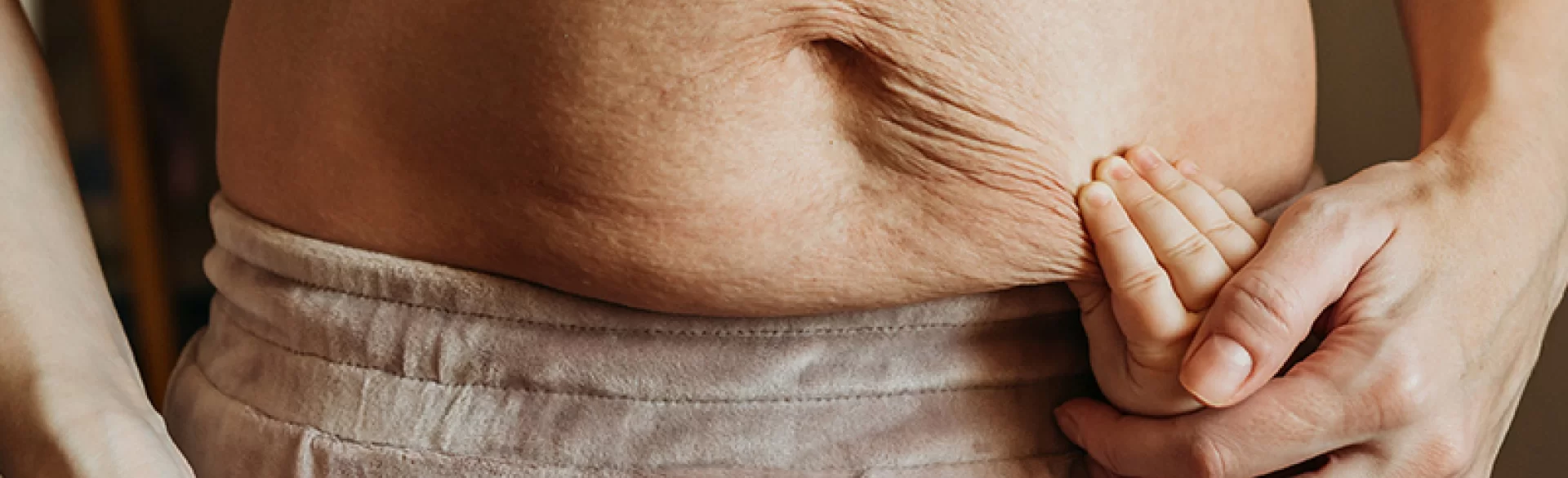
The puerperium (Latin: puerperium) is the physiological period immediately following childbirth, during which a woman's body gradually returns to its pre-pregnancy state. It includes the processes of involution of the reproductive organs (i.e., their contraction), tissue regeneration, and hormonal and metabolic adaptation. During this time, significant changes also occur in the cardiovascular, hormonal, and psychological systems. The puerperium is a crucial stage for a woman's health—both physically and emotionally—and its proper course conditions the restoration of the body's balance and reduces the risk of postpartum complications.
Postpartum period - how long does it last
The postpartum period typically lasts about 6 weeks (42 days) from the time of delivery, although this period may vary individually depending on the course of the pregnancy, the type of delivery, and the woman's overall health.
In classic medical terms, three stages of the postpartum period are distinguished:
- Immediate postpartum period (up to 24 hours after delivery) – a period of intensive medical supervision during which there is the greatest risk of complications, such as postpartum hemorrhage.
- Early postpartum period (up to 7 days) – a time of intensive uterine involution and tissue healing.
- Late postpartum period (up to 6 weeks) – a stage of further bodily recovery and hormonal stabilization.
The process of uterine contraction (involution) proceeds dynamically – its mass decreases from about 1000 g immediately after delivery to about 50-70 g after the end of the postpartum period. At the same time, the lochia (postpartum discharge) gradually diminish, changing in color and character (from bloody to serous, and then to mucous).
In some women, particularly those who are breastfeeding, hormonal processes may prolong the period of return to full physiological balance, especially with regard to the menstrual cycle.
Puerperium - changes in the body
The postpartum period is associated with wide-ranging changes affecting almost all body systems. The most significant concern the reproductive, hormonal, and psychological systems.
Anatomical and physiological changes:
- Uterine involution - gradual contraction of the uterus and regeneration of the endometrium.
- Regeneration of the cervix and vagina - restoration of the epithelium and tissue tone.
- Healing of postpartum wounds - in the perineal area (after an episiotomy or tearing) or of the abdominal wall after a cesarean section.
- Changes in the breasts - development of lactation under the influence of prolactin and oxytocin.
Hormonal changes:
- a rapid decrease in estrogen and progesterone levels,
- an increase in prolactin concentration (especially in breastfeeding women),
- the effect of oxytocin on uterine contraction and the lactation process.
Systemic changes:
- increased diuresis (elimination of excess fluids),
- changes in the coagulation system (increased risk of thrombosis),
- gradual normalization of blood parameters (e.g., hematocrit).
Psychological changes:
- mood swings related to hormonal adaptation,
- the so-close baby blues (a mild, transient low mood),
- the risk of postpartum depression requiring diagnosis and treatment.
Postpartum period after vaginal birth and after cesarean section
The course of the postpartum period differs significantly depending on the type of delivery, which affects the pace of recovery and potential complications.
Postpartum after vaginal delivery:
- faster mobilization and return to activity,
- healing processes predominantly involve the perineal tissues,
- greater emphasis on pelvic floor muscle rehabilitation,
- lower risk of surgical complications.
Postpartum after cesarean section:
- longer recovery time,
- healing of the postoperative wound in the abdominal wall and the uterus,
- higher risk of complications such as:
- wound infection,
- suture dehiscence,
- formation of internal adhesions,
- venous thrombosis.
In the case of a cesarean section, scar monitoring and its proper remodeling are particularly important. Abnormal healing can lead to the formation of hypertrophic scars, pain symptoms and disorders of muscle-fascial function.
In both cases, early initiation of urogynaecological physiotherapy is crucial, as it supports pelvic floor regeneration, improves muscle function and reduces the risk of urinary incontinence or pelvic organ prolapse.
Postpartum period - when to see a specialist
Although the postpartum period is a physiological process, there are a number of symptoms that require urgent medical consultation. Their occurrence may indicate developing complications.
The most important warning signs include:
- heavy vaginal bleeding (greater than a menstrual period),
- persistent or increasing lower abdominal pain,
- fever (>38°C) and signs of infection,
- foul-smelling lochia,
- pain, redness, or swelling of the wound (perineum or cesarean incision),
- difficulty urinating or defecating,
- signs of thrombosis (pain and swelling of the lower limbs),
- marked mood deterioration, anxiety, depressive symptoms.
Indications for a scheduled consultation include:
- failure of proper uterine involution,
- persistent pain in scar areas,
- symptoms of pelvic floor dysfunction (e.g., urinary incontinence, a feeling of "heaviness" in the vagina),
- breastfeeding problems.
In clinical practice it is recommended that every woman attends a follow-up gynecological visit at about 6 weeks after delivery, and much earlier in the presence of worrying symptoms.
Contemporary approaches to postpartum care primarily include conservative methods supporting the physiological regeneration of tissues during the postpartum period, such as:
- urogynecological physiotherapy,
- early scar therapy (manual, after complete wound closure),
- education on correct activation of the pelvic floor muscles and breathing patterns.
This approach enables safe support of healing processes and reduces the risk of later functional complications.
Advanced procedures that stimulate tissue remodeling, such as laser therapy or microneedle radiofrequency, are used only after the postpartum period has ended and tissues have fully regenerated, in cases requiring further therapy.
Their proper implementation – at the appropriate time and after specialist qualification – allows a more effective and safer return to full physical function.
