Red pimples on the back
back to main page
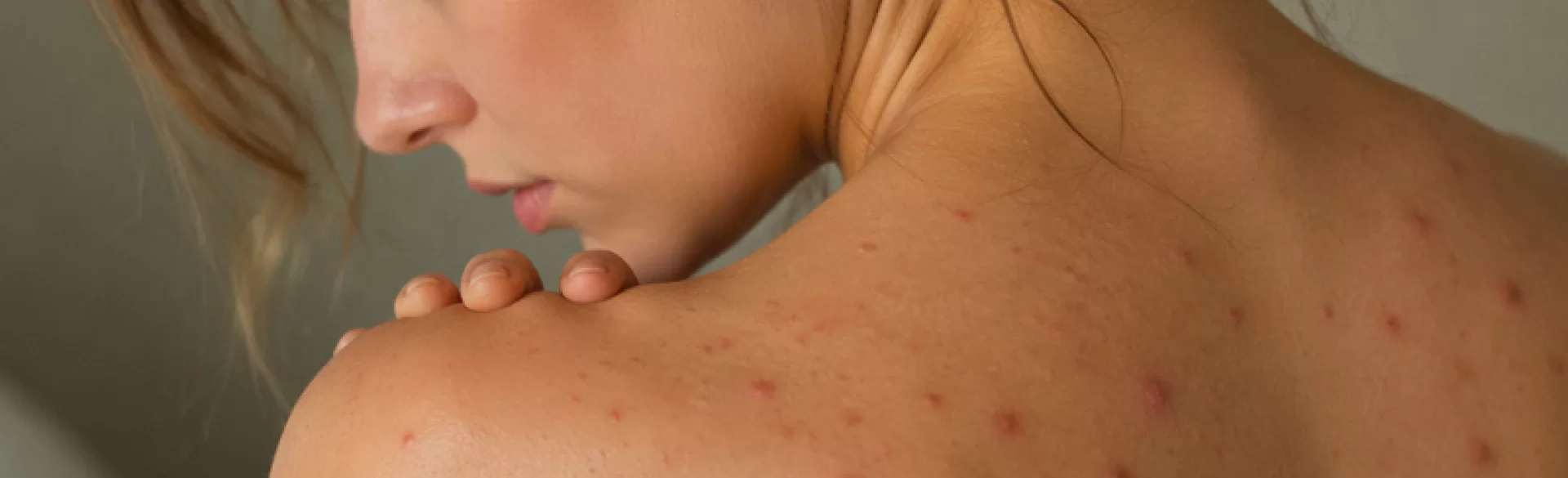
Red pimples on the back are inflammatory skin lesions that can take the form of papules, pustules, or nodules. They are most often associated with sebaceous gland disorders, excessive keratinization of the hair follicle openings, and the presence of microorganisms, mainly Cutibacterium acnes bacteria. This problem affects both adolescents and adults, and its severity can vary – from single lesions to extensive, painful inflammatory foci. The location on the back results from a large number of sebaceous glands and limited skin ventilation in this area.
Red bumps on the back - causes
The etiology of red pustules on the back is multifactorial and includes both endogenous (internal) and exogenous (external) factors. A key role is played by the overproduction of sebum, leading to the clogging of hair follicle openings and the formation of inflammatory lesions.
The most important causes include:
- Acne vulgaris – the most common cause, associated with excessive activity of sebaceous glands, colonization by Cutibacterium acnes, and an inflammatory reaction
- Hormonal disorders – especially excess androgens, which increases sebum production
- Hyperkeratosis of hair follicle openings (hyperkeratinization) – leads to the formation of comedones and secondary inflammatory lesions
- Excessive sweating and skin occlusion – e.g., wearing tight clothing, synthetic materials, or prolonged stay in a humid environment
- Improper skin care – the use of comedogenic (pore-clogging) cosmetics
- Folliculitis – can have a bacterial or fungal basis
- Dietary and lifestyle factors – a high glycemic index diet, stress, lack of sleep
- Medications – e.g., corticosteroids, some hormonal preparations
It is worth emphasizing that lesions on the back often have a more severe course than on the face due to thicker skin and a higher number of sebaceous glands. Left untreated, they can lead to the formation of scars, including hypertrophic scars and post-inflammatory hyperpigmentation.
Red pimples on the back - what they look like
The clinical presentation of red pustules on the back is varied and depends on the cause and the severity of the inflammatory process. Lesions can occur individually or in clusters, covering various areas of the back – most commonly the upper part (shoulder blade and neck area).
Typical features of the lesions:
- Papules (papule) – small, red, elevated lesions without visible purulent content
- Pustules (pustule) – lesions containing purulent content, often with a whitish tip
- Inflammatory nodules (nodules) – deep, painful lesions of larger sizes
- Cysts (cysty) – lesions filled with liquid or semi-liquid content, which can lead to scarring
- Erythema (redness) – the result of vasodilation and inflammatory reaction
Additionally, there may occur:
- itching or tenderness, especially with deeper lesions
- post-inflammatory hyperpigmentation – brown or red spots persisting after healing
- scars – especially in the case of chronic or improperly treated lesions
In the differential diagnosis, other disease entities should be considered, such as acne mechanica (caused by friction), drug-induced acne, fungal folliculitis, or heat rash (miliaria).
The assessment of the morphology of the lesions is of significant clinical importance, as it allows for the selection of appropriate therapeutic management and prediction of the risk of complications, including the formation of permanent scars.
Red bumps on the back – dermatological and aesthetic treatments
In the case of persistent or severe inflammatory lesions on the back that do not respond to pharmacological treatment or care, dermatological procedures and aesthetic medicine treatments are of significant importance. Their aim is to reduce inflammation, normalize the activity of the sebaceous glands, limit microbial colonization, and prevent the formation of scars and post-inflammatory hyperpigmentation.
The most commonly used methods include:
- Chemical peels (medical) – utilizing, among others, salicylic, mandelic, or trichloroacetic (TCA) acid. They have a keratolytic (exfoliating) effect, unblock the openings of hair follicles, and exhibit anti-inflammatory and sebum-regulating properties. Particularly effective in treating comedonal and papulopustular lesions.
- Laser therapy – including fractional lasers and anti-inflammatory devices. The mechanism is based on selective targeting of the sebaceous glands and reduction of Cutibacterium acnes bacteria. Additionally, they stimulate skin remodeling, which is important in the prevention and treatment of acne scars.
- Light therapy (LED) – especially blue light (bactericidal effect) and red light (anti-inflammatory and regenerative effect). A non-invasive method, often used as a supplement to other therapies.
- Microneedle mesotherapy – involves controlled microneedling of the skin, which induces repair processes and stimulates collagen production. It can be used both in the treatment of active lesions (in combination with active substances) and in the reduction of acne scars.
- Medical skin cleansing – a procedure involving manual or assisted removal of comedones and pustules, performed under controlled conditions. It allows for reducing the risk of inflammation spreading and improves the effectiveness of topical therapy.
- Microneedle radiofrequency – a technology combining microneedling with the action of radio wave energy, leading to the reduction of inflammation and remodeling of the dermis. Particularly useful in the treatment of chronic lesions and scars.
In clinical practice, combination therapies are most commonly used, as a single method rarely provides optimal results. The selection of an appropriate treatment protocol should be individual and take into account:
- severity of inflammatory lesions,
- skin type and its reactivity,
- presence of scars or hyperpigmentation,
- previous treatment methods.
These treatments are a significant supplement to dermatological treatment, especially in resistant or recurrent cases, and their proper application allows not only for the reduction of skin lesions but also for the improvement of the quality and structure of the back skin.