Pimples on the cheeks
back to main page
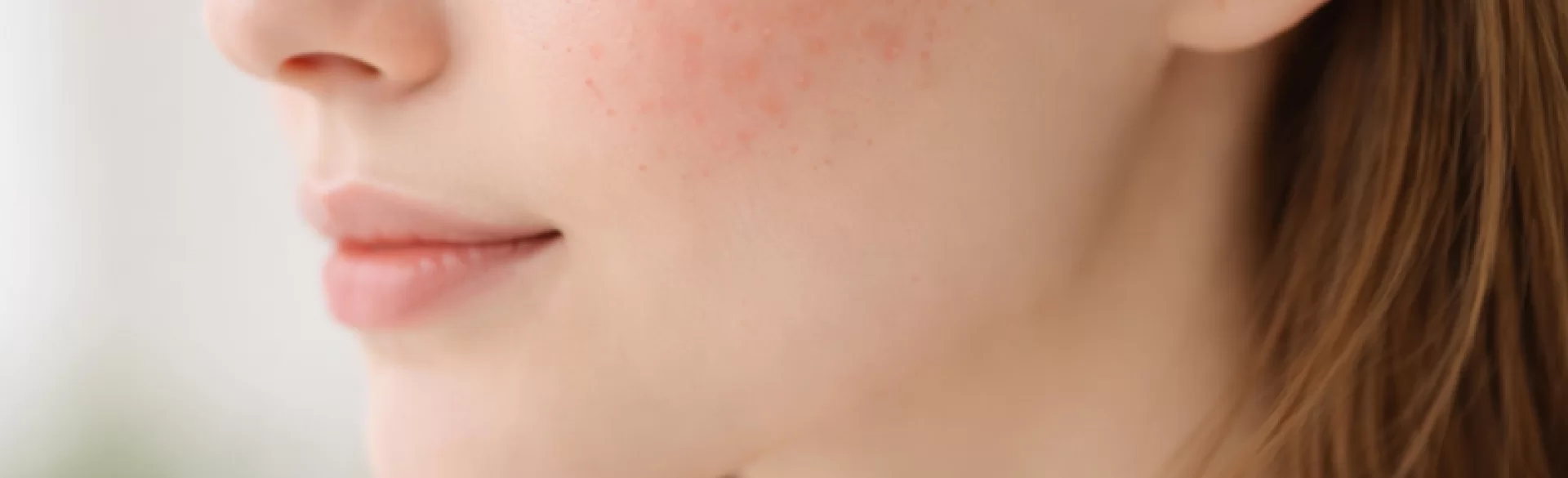
Pimples on the cheeks are skin changes of an inflammatory or non-inflammatory nature, appearing within the facial skin, most commonly in the course of acne vulgaris, rosacea, hormonal disorders, or hypersensitivity reactions. They can manifest as papules, pustules, open and closed comedones, as well as painful inflammatory infiltrates. The location on the cheeks has clinical significance – this area is characterized by high sebaceous gland activity and frequent contact with external factors (cosmetics, protective masks, phones). Proper diagnosis requires differentiation from folliculitis, allergic contact dermatitis, or vascular dermatoses.
Acne on the Cheeks – Causes
The etiology of papulopustular lesions on the cheeks is multifactorial, involving both local and systemic mechanisms.
Most common causes:
- Acne vulgaris – excessive sebum production, hyperkeratinization of hair follicle openings, colonization by Cutibacterium acnes, and inflammatory response.
- Hormonal disturbances – hyperandrogenism (e.g., in PCOS), insulin resistance, fluctuations in estrogen and progesterone levels.
- Rosacea – particularly in the papulopustular form, with accompanying erythema and telangiectasias.
- Contact dermatitis (allergic or irritant) – reaction to components of cosmetics (e.g., preservatives, fragrances, silicones, comedogenic oils).
- Maskne – changes induced by prolonged wearing of protective masks.
- High glycemic index diet – increased secretion of IGF-1 and stimulation of sebaceous glands.
- Chronic stress – activation of the HPA axis (hypothalamus–pituitary–adrenal) and exacerbation of inflammation.
It is important to note that in adult women, lesions on the cheeks often coexist with hormonal acne, which may require endocrine diagnostics (TSH, prolactin, androgens).
Pimples on the cheeks – home remedies
Home care should be supportive and does not replace dermatological therapy in the case of severe inflammatory changes.
Recommended actions:
- Gentle skin cleansing twice a day using a product with a pH close to physiological (about 5.5).
- Avoiding aggressive mechanical peels that exacerbate inflammation.
- Using non-comedogenic dermocosmetics.
- Limiting simple sugars and dairy if a correlation with exacerbation of symptoms is observed.
- Regularly changing pillowcases and disinfecting the phone.
What to avoid:
- squeezing pimples (risk of acne scars and post-inflammatory hyperpigmentation),
- using alcohol or toothpaste as "drying agents",
- self-combining multiple highly active ingredients (retinoids + acids + benzoyl peroxide).
If changes persist for more than 6–8 weeks, recurrent inflammations, or scar formation occur, a dermatological consultation is necessary.
Acne on cheeks – treatment
Treatment should be tailored to the clinical diagnosis and the severity of the changes.
1. Topical treatment
- Retinoids (adapalene, tretinoin) – normalization of keratinization and anti-inflammatory action.
- Benzoyl peroxide – reduction of bacterial colonization.
- Azelaic acid – anti-inflammatory action and lightening of hyperpigmentation.
- Metronidazole or ivermectin – in rosacea.
2. Systemic treatment
- oral antibiotics (doxycycline),
- hormonal treatment (contraception with an anti-androgenic component),
- isotretinoin in severe forms of acne.
3. Procedural therapies used in aesthetic dermatology
For persistent inflammatory changes, acne scars, or post-inflammatory hyperpigmentation, effective methods include:
- medical peels (salicylic acid, azelaic acid, TCA),
- fractional CO₂ laser therapy – stimulation of collagen remodeling,
- microneedle radiofrequency – scar reduction and skin texture improvement,
- LED light therapy (anti-inflammatory action),
- manual, apparatus cleansing, and sebum-regulating treatments.
In clinical practice at the Beauty Embassy in Warsaw, combined therapies are used, including: medical peels + LED light, microneedle radiofrequency, and regenerative treatments supporting the reconstruction of the epidermal barrier.