White pimples
back to main page
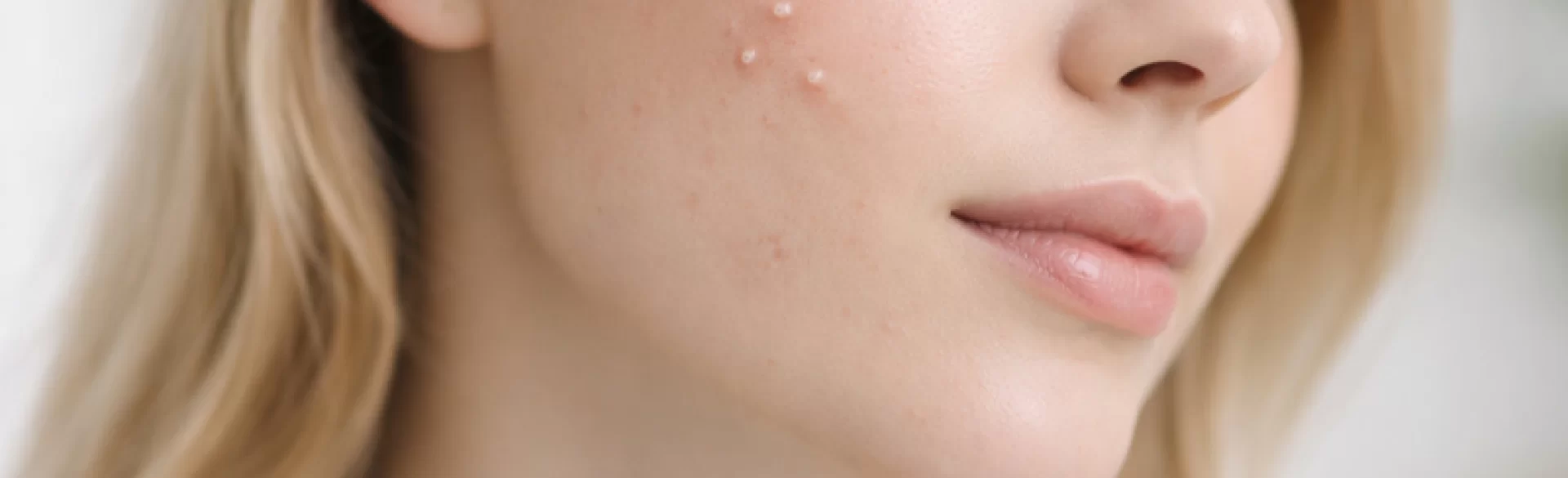
White pimples are a common term for skin lesions characterized by small bumps or pustules with visible, light-colored purulent or sebaceous content. In dermatology, they most frequently correspond to closed comedones (whiteheads) or inflammatory pustules associated with acne vulgaris. They form due to the blockage of the hair follicle opening by excess sebum, keratinized skin cells, and bacteria, mainly Cutibacterium acnes. White pimples can appear on the face (particularly in the T-zone), back, chest, and shoulders. Their presence may be temporary, but in some patients, they are part of a chronic dermatosis requiring dermatological treatment.
White Pimples – Where Do They Come From
The pathogenesis of white pimples is multifactorial and involves four key mechanisms characteristic of acne:
- Excessive sebum production
- stimulated by androgens (especially during puberty),
- exacerbated by stress, lack of sleep, and a high glycemic index diet.
- Disorders of keratinization of the hair follicle opening (hyperkeratinization)
- lead to the blockage of the sebaceous gland duct,
- result in the formation of a closed comedo with a white, invisible sebum plug.
- Proliferation of Cutibacterium acnes bacteria
- these bacteria break down sebum lipids, causing an inflammatory reaction,
- resulting in the formation of a pustule with visible white purulent content.
- Inflammatory skin reaction
- activation of pro-inflammatory cytokines (IL-1, TNF-α),
- swelling and redness of the surrounding tissues.
Factors promoting the formation of white pimples:
- use of comedogenic cosmetics,
- inadequate makeup removal,
- hormonal disorders (e.g., hyperandrogenism, PCOS),
- chronic stress,
- improper skincare (excessive drying of the skin).
It is worth emphasizing that individual white pimples do not always indicate a disease - they become a clinical problem only in the case of numerous, recurring changes or those that leave scars.
White pimples – should you pop them
Squeezing whiteheads is one of the most common skincare and dermatological mistakes. Mechanical pressure on the lesion can lead to:
- the spread of bacteria into deeper layers of the skin,
- worsening of inflammation,
- formation of post-inflammatory hyperpigmentation (PIH),
- development of atrophic or hypertrophic scars.
Particularly dangerous is manipulating lesions in the so-called "danger triangle" of the face (the area around the nose and upper lip), where there is a risk of infection spreading through venous pathways.
Exceptions include professional cleansing treatments performed in controlled conditions by a doctor or qualified cosmetologist. Such a procedure includes:
- proper preparation of the skin (softening, disinfection),
- sterile tools,
- control of the depth of pressure,
- use of anti-inflammatory preparations after the procedure.
From a medical perspective, squeezing in home conditions is not recommended. In the case of painful, extensive, or recurrent lesions, a dermatological consultation is advised.
White pimples – how to remove
The course of treatment depends on the severity of the changes and their cause. Treatment includes both topical therapy and supportive procedures.
1. Topical Treatment
The most commonly used active substances:
- retinoids (e.g., adapalene, tretinoin) – normalize keratinization,
- salicylic acid – has keratolytic and anti-inflammatory effects,
- benzoyl peroxide – limits bacterial growth,
- azelaic acid – reduces inflammation and discoloration,
- topical antibiotics (in specific indications).
2. Systemic Treatment
In cases of moderate to severe acne:
- oral antibiotics (e.g., doxycycline),
- hormonal treatment (in women with hyperandrogenism),
- oral isotretinoin – in severe, resistant cases.
3. Dermatological and Aesthetic Medicine Procedures
In supportive therapy, the following are used:
- chemical peels (salicylic acid, mandelic acid, TCA),
- manual or apparatus-based cleansing,
- anti-inflammatory laser therapy,
- microneedle radiofrequency and fractional laser therapy for scar reduction,
- LED light therapy with bactericidal effects.
In clinical practice, the effectiveness of treatment depends on:
- consistent therapy,
- proper home care,
- elimination of provoking factors,
- individual selection of procedures.
Whiteheads, although often underestimated, manifest as a dysfunction of the pilosebaceous unit. Early implementation of targeted therapy can limit the risk of chronic inflammation and the formation of permanent consequences such as scars and discoloration.