Papular psoriasis
back to main page
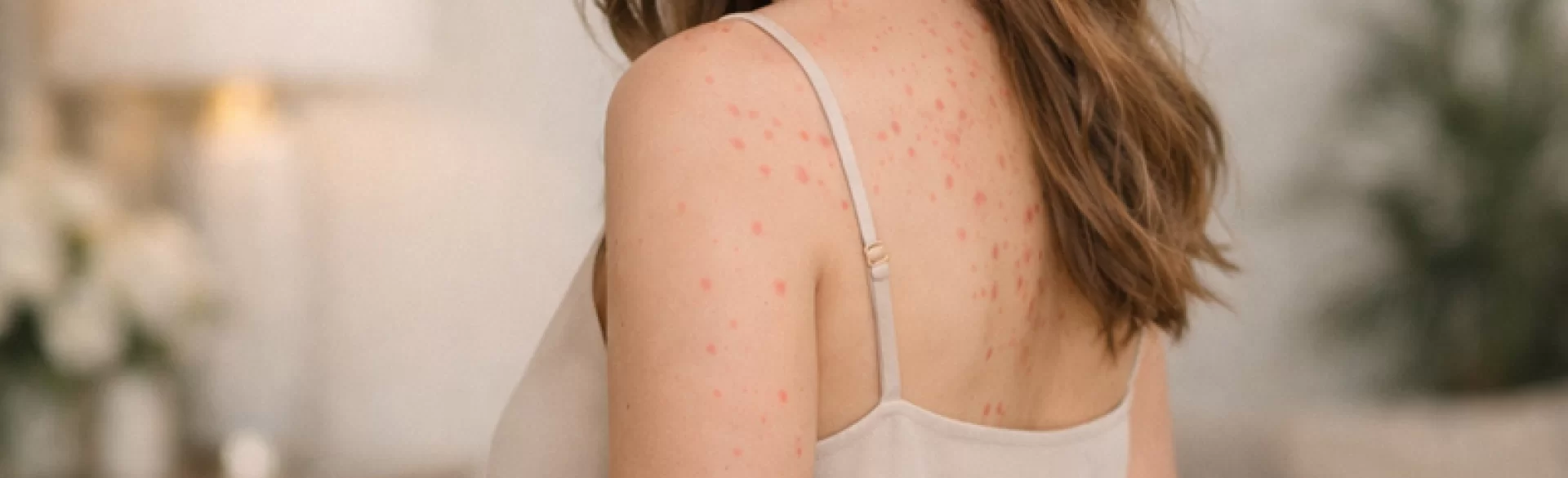
Łuszczyca grudkowa (łac. psoriasis guttata) jest jedną z klinicznych odmian łuszczycy – przewlekłej, zapalnej choroby skóry o podłożu immunologicznym. Charakteryzuje się występowaniem licznych drobnych zmian skórnych w postaci grudek lub niewielkich ognisk rumieniowo-złuszczających, które przypominają krople wody rozsiane na powierzchni skóry. Choroba najczęściej pojawia się nagle i dotyczy głównie dzieci, młodzieży oraz młodych dorosłych. U wielu pacjentów pierwsze objawy występują po przebytej infekcji, szczególnie paciorkowcowym zapaleniu gardła. Łuszczyca grudkowa może mieć przebieg samoograniczający się, jednak u części chorych stanowi wstęp do rozwoju przewlekłej łuszczycy plackowatej.
Papular - guttate psoriasis
The most characteristic form of papular psoriasis is guttate psoriasis, whose name comes from the typical appearance of skin lesions resembling drops. These lesions usually have a diameter of a few millimeters up to about 1 cm and are symmetrically distributed on the skin.
The most common locations include:
- trunk (back and chest)
- arms and thighs
- scalp
- less often the face
The skin lesions take the form of:
- small red papules or spots,
- areas covered with a fine, silvery scale,
- numerous eruptions appearing simultaneously over a large area of skin.
In contrast to plaque psoriasis, lesions in guttate psoriasis are significantly smaller and more numerous, and their development usually has a sudden onset.
Bacterial infections, primarily Streptococcus pyogenes infections, play an important role in the pathogenesis of this form of the disease. In many patients, an outbreak of lesions appears 2–3 weeks after tonsillitis or pharyngitis. This mechanism is related to an abnormal immune system response, which activates T lymphocytes and leads to excessive proliferation of keratinocytes, the cells of the epidermis.
Factors that increase the risk of developing papular psoriasis include:
- genetic predisposition,
- bacterial and viral infections,
- psychological stress,
- certain medications (e.g., beta-blockers or lithium),
- skin injuries.
Papular psoriasis – symptoms
Symptoms of guttate psoriasis usually appear suddenly and rapidly, often within a few days. The disease can affect large areas of the skin, causing numerous outbreaks of small lesions.
The most typical symptoms are:
- numerous small erythematous papules measuring a few millimetres in diameter,
- the presence of a delicate silvery scale on the surface of the lesions,
- scattered inflammatory lesions on the trunk and limbs,
- skin itching of varying severity,
- a burning sensation or hypersensitivity of the skin.
On dermatological examination, characteristic signs of psoriasis can be observed, such as:
- the stearin candle sign – descaling of the scale after gentle scraping,
- the Auspitz sign – pinpoint bleeding after removal of the scale.
Skin lesions usually do not cause pain, but their sudden eruption can be a significant cosmetic and psychological problem for the patient.
Some patients also have:
- scalp lesions resembling dandruff,
- nail involvement (less frequent than in plaque psoriasis),
- a relapsing course of the disease.
In many cases guttate psoriasis resolves spontaneously within several weeks or months. However, in approximately 30–40% of patients it may progress to a chronic form of psoriasis.
Papular psoriasis – treatment
Treatment of papular psoriasis depends on the severity of the skin lesions, their extent, and the presence of triggering factors. Therapy aims to reduce skin inflammation, limit excessive keratinization, and control the body's immune response.
The most commonly used treatment methods include:
Topical treatment
It is primarily used in mild forms of the disease.
The most commonly used preparations include:
- topical glucocorticosteroids – reduce inflammation and itching,
- preparations with vitamin D3 analogues (e.g., calcipotriol),
- topical retinoids regulating keratinization of the epidermis,
- keratolytic preparations with salicylic acid or urea.
Phototherapy
One of the most effective methods for treating papular psoriasis is narrowband UVB (NB-UVB) phototherapy. Ultraviolet radiation inhibits the excessive activity of the immune system in the skin and slows keratinocyte proliferation.
Phototherapy is particularly effective in cases of:
- numerous eruptions,
- extensive lesions on the trunk and limbs,
- lack of response to topical treatment.
Systemic treatment
In more severe forms of the disease, systemic therapy is used, such as:
- oral retinoids,
- methotrexate,
- cyclosporine,
- modern biologic drugs modulating the immune response.
If the disease was triggered by a streptococcal infection, treatment of the bacterial infection is also necessary, usually with antibiotic therapy.
Supportive measures
Appropriate skin care also plays an important role in therapy, helping to reduce dryness and scaling.
It is recommended to:
- regular use of emollients,
- avoid irritating cosmetics and detergents,
- reduce stress, which can worsen the course of the disease,
- treat comorbid conditions.
In aesthetic dermatology, procedures that support improvement of skin condition and reduction of inflammatory lesions are also used, such as LED light therapies, dermatological peels, and skin regenerative procedures, which can support epidermal renewal and improve barrier function.