Pimples with blood on the face
back to main page
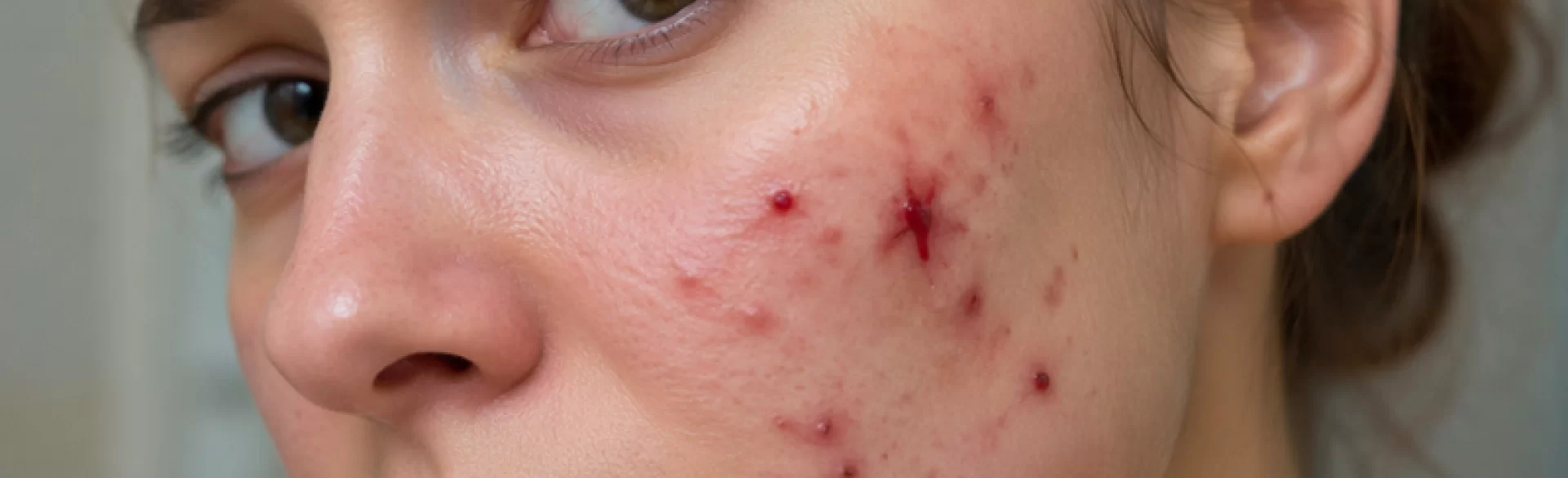
Bloody pimples on the face are inflammatory skin lesions in which damage to the capillaries occurs and bloody content is present within the lesion. They are most often an advanced form of inflammatory acne or the result of mechanical disruption of the skin structure, leading to the formation of an erosion or micro-injury. The presence of blood indicates deeper tissue damage, involving not only the epidermis but also the dermis. These types of lesions require special therapeutic caution because they are associated with an increased risk of scarring, post-inflammatory hyperpigmentation, and secondary bacterial infections.
Pimples with blood on the face – where do they come from
The pathogenesis of pimples with a hemorrhagic component is based on disturbances in the functioning of the pilosebaceous unit and an intensified inflammatory reaction. Three processes are of key importance: excessive sebum production, abnormal keratinization of hair follicle openings, and colonization by Cutibacterium acnes bacteria. In the course of intense inflammation, damage to the walls of small blood vessels and extravasation of blood occur.
The most important etiological factors include:
- inflammatory acne – especially papulopustular and nodulocystic forms,
- mechanical skin damage – squeezing, scratching, rubbing,
- blood vessel fragility – common in people with vascular skin or in the course of inflammatory states,
- hormonal disorders – especially an excess of androgens stimulating the sebaceous glands,
- use of aggressive dermatological preparations (e.g., excessive exfoliation),
- inflammation of hair follicles,
- systemic factors – vitamin deficiencies (e.g., vitamin C), coagulation disorders.
In clinical practice, a very important element is distinguishing whether the lesion arose spontaneously or as a result of manipulation. Squeezing pimples leads to a rapid increase in pressure within the lesion, resulting in vessel rupture and the spread of inflammation deeper into the skin. Consequently, the risk of developing the following increases:
- atrophic scars,
- post-inflammatory hyperpigmentation (PIH),
- bacterial superinfections.
Bloody pimples on the face – how to treat
Treatment of bloody pimples requires a multi-directional approach including inflammation control, acceleration of skin regeneration, and complication prevention. The therapeutic strategy should be adapted to the severity of the lesions and their depth.
Dermatological treatment
In primary therapy, the following are used:
- topical retinoids – normalize the keratinization process and prevent the formation of new lesions,
- benzoyl peroxide – has antibacterial and anti-inflammatory effects,
- topical or systemic antibiotics – in case of severe inflammation,
- oral isotretinoin – in severe, resistant forms of acne,
- hormonal treatment – in patients with endocrine disorders.
Local and regenerative management
Proper care supporting the healing process is of key importance:
- preparations with panthenol, allantoin, ceramides – accelerate regeneration,
- anti-inflammatory ingredients (e.g., niacinamide),
- restoration of the skin's hydrolipid barrier,
- strict photoprotection – reduces the risk of post-inflammatory hyperpigmentation,
- elimination of irritating factors.
Lesions with the presence of blood should be treated like skin micro-injuries – they require an environment conducive to regeneration, rather than aggressive exfoliation.
Procedural treatment
In the case of recurrent, deep lesions or those leaving marks, aesthetic dermatology procedures are used:
- chemical peels (e.g., salicylic acid, azelaic acid) – keratolytic and anti-inflammatory action,
- non-ablative laser therapy – reduction of inflammation and stimulation of skin remodeling,
- needle mesotherapy – improvement of tissue regeneration and nourishment,
- LED light therapy – antibacterial and soothing effect.
The selection of the procedure should take into account the phase of the lesion – in an active inflammatory state, soothing methods are preferred, while remodeling treatments are used after the lesions have healed.
Differentiation of lesions
In clinical practice, it is important to differentiate bloody pimples from other lesions:
- erosions – superficial epidermal defects, often after trauma,
- hemorrhagic lesions – related to vessel fragility or clotting disorders,
- acne fulminans – a severe, rare form of acne requiring urgent treatment.
Prognosis and healing time
Healing time depends on the depth of the lesion and the management method:
- superficial lesions: 3–7 days,
- deeper inflammatory lesions: 1–3 weeks,
- manipulated lesions: often a longer process and higher risk of complications.
The prognosis is good with proper therapy; however, completely avoiding skin marks requires early intervention and the elimination of damaging factors.
Treatments used in the therapy of acne lesions
In the practice of aesthetic medicine clinics, a comprehensive approach to the therapy of acne and its consequences is used. The most commonly used procedures include:
- needle mesotherapy – improvement of skin regeneration and quality,
- chemical peels – regulation of keratinization and reduction of inflammatory lesions,
- laser therapy – anti-inflammatory action and reduction of discoloration and scars,
- LED light therapies – support for antibacterial treatment,
- regenerative treatments – skin restoration after inflammation.
Their appropriate combination allows not only for the treatment of active lesions but also for improving skin structure and limiting the risk of permanent consequences.