Scars on the back
back to main page
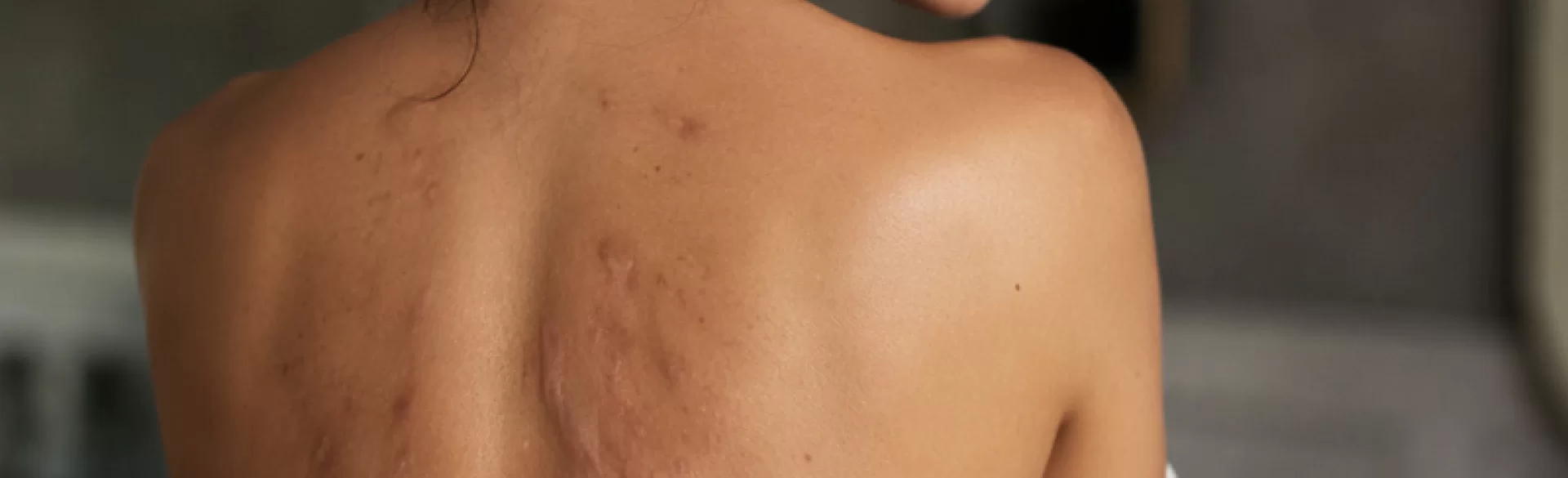
Scars on the back are permanent structural skin changes resulting from the healing process after tissue damage. Within them, abnormal reconstruction of collagen occurs – the main structural protein of the dermis. Depending on the course of healing, atrophic scars, hypertrophic scars, and keloids are distinguished. The back area, due to a large number of sebaceous glands, the frequent occurrence of acne, and high skin tension, is particularly predisposed to the formation of visible and therapeutically challenging scars. These changes can cause not only an aesthetic defect but also subjective symptoms such as itching, tenderness, or a feeling of skin tension.
Scars on the back - causes
The most common cause of scars on the back is acne vulgaris, especially its inflammatory form – nodulocystic acne. In the course of deep inflammation, damage to the dermis occurs, and the repair process leads to the deposition of improperly organized collagen. As a result, scars of various morphology are formed.
The main causes include:
- Chronic skin inflammation – especially untreated or improperly treated acne
- Mechanical skin damage – squeezing lesions, scratching, injuries
- Folliculitis and furunculosis
- Injuries and burns – both thermal and chemical
- Surgical procedures – especially in the shoulder and upper back area
An important factor is also local skin tension. The back, especially the interscapular and shoulder area, is subject to constant movement, which causes tissue stretching during healing. This promotes the formation of hypertrophic scars and their widening.
Genetic and individual factors remain significant, such as:
- tendency to form keloids
- skin phototype (higher risk in individuals with darker complexions)
- individual activity of fibroblasts (collagen-producing cells)
It is worth emphasizing that not every post-inflammatory lesion is a scar. Post-inflammatory hyperpigmentation (PIH) or post-inflammatory erythema often coexist, which can mimic or exacerbate the visibility of scars, yet they require a different therapeutic approach.
Scars on the back - how to get rid of them
Treatment of back scars is a multi-stage process and depends on the type of scar, its depth, duration, and the activity of skin inflammatory processes. Therapy is based on two main mechanisms: stimulating collagen remodeling (in atrophic scars) and inhibiting its excessive production (in hypertrophic scars and keloids). In clinical practice, combined therapies are most commonly used because a single method rarely leads to satisfactory improvement.
Atrophic scars - treatment
Atrophic scars are formed as a result of tissue loss and insufficient collagen production. The therapy aims to stimulate fibroblasts to synthesize new collagen and remodel the existing skin structure.
Most important methods:
- Fractional laser therapy (CO₂, Er:YAG, non-ablative)
It causes controlled micro-damage in the skin, initiating regenerative processes. As a result, skin density increases and scars become shallower. Ablative lasers work more intensively but require longer recovery.
- Microneedle radiofrequency (RF microneedling)
It combines microneedling with radiofrequency energy, leading to deeper collagen stimulation without damaging the skin surface to the same extent as a laser.
- Microneedling (micro-needle mesotherapy)
The mechanical creation of micro-channels in the skin stimulates repair processes and improves the penetration of active substances.
- Chemical peels (e.g., TCA)
Used mainly for shallower scars and coexisting hyperpigmentation. They cause controlled exfoliation and regeneration of the epidermis and partially the dermis.
The effect of the therapy is the gradual smoothing of the skin surface, improvement of its structure and color.
Hypertrophic scars - treatment
Hypertrophic scars are the result of excessive collagen production, but they do not exceed the boundaries of the original wound. Treatment is aimed at reducing their volume and biological activity.
Methods used:
- Corticosteroid injections (e.g., triamcinolone)
They inhibit fibroblast proliferation and collagen synthesis, leading to the flattening of the scar.
- Silicone therapy (gels, patches)
It maintains proper hydration and the skin's microenvironment, which influences the regulation of scarring processes.
- Laser therapy (especially vascular and fractional lasers)
It reduces the vascularity of the scar and supports its remodeling.
The goal of treatment is to soften, flatten, and reduce the redness of the scar.
Treatment of keloids
Keloids are the most advanced form of pathological scarring and are characterized by growth beyond the boundaries of the original injury and a high tendency for recurrence.
Therapeutic management includes:
- Intralesional injections (corticosteroids, often in combination therapies)
- Cryotherapy – leading to the destruction of pathological tissue
- Laser therapy as an element of combined therapy
The treatment of keloids requires special caution, as overly aggressive procedures can stimulate their further growth.
The importance of combined therapies and treatment planning
Modern dermatology and aesthetic medicine are based on the individualization of therapy. In practice, this means combining different methods to achieve a synergistic effect, e.g.:
- laser therapy + microneedling
- injections + laser therapy
- RF microneedling + chemical peels
Also of key importance are:
- previous treatment of active acne or skin inflammation
- proper qualification of the scar type
- regularity of therapy
Without eliminating the causative factor (e.g., active acne), scar treatment is ineffective or short-lived.
Procedures used in clinical practice
Modern aesthetic medicine clinics use advanced technologies that enable effective skin remodeling:
- fractional CO₂ and Er:YAG laser therapy
- microneedle radiofrequency
- needle and micro-needle mesotherapy
- medical chemical peels
Their common goal is:
- stimulation of neocollagenesis
- improvement of skin structure and density
- reduction of scar visibility
The effects of the therapy are gradual and cumulative, and their scope depends on the type and severity of the changes.

