Post-accident scars
back to main page
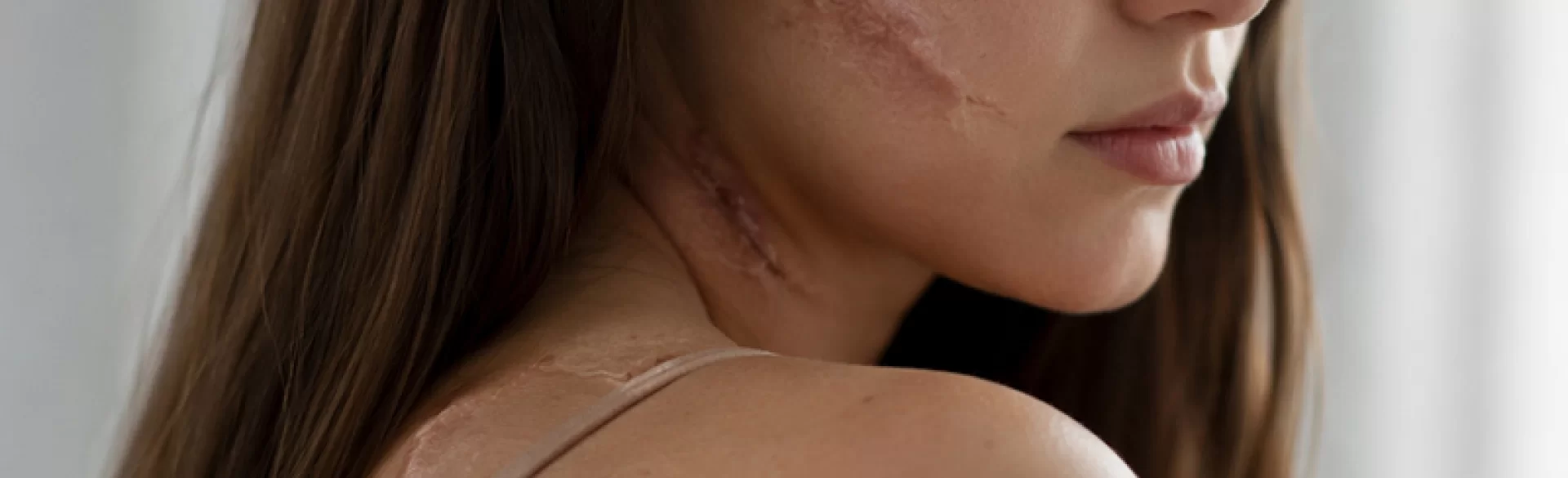
Post-accident scars are permanent changes in the skin and deeper tissues that form at the site of damage after mechanical, thermal, or chemical injury. They are the result of a natural healing process in which the body replaces damaged tissue with newly formed connective tissue. Their appearance, extent, and impact on tissue function depend primarily on the depth of the injury, the location of the wound, how it was managed, the presence of infection, and individual predispositions to scarring. A post-traumatic scar is therefore not merely an aesthetic defect. It can cause pain, itching, a pulling sensation, limited mobility, and in some locations, also functional disorders and significant psychological burden.
Post-accident scars - characteristics
Post-accident scars develop after a wound heals, when tissue continuity is restored with the involvement of collagen fibers. Unlike undamaged skin, scar tissue has a simplified structure, less elasticity, poorer vascularization, and usually does not fully reproduce skin appendages, such as hair follicles or glands. For this reason, a scar may differ from its surroundings in color, consistency, thickness, and susceptibility to stretching.
In clinical practice, post-accident scars do not form a single, homogeneous group. They may take the form of:
- flat scars, relatively inconspicuous and similar in level to the surrounding skin,
- atrophic scars, i.e., depressed, when tissue loss occurs during the healing process,
- hypertrophic scars, raised above skin level but limited to the borders of the original wound,
- keloids, which grow beyond the area of the original injury,
- contracture scars, which can restrict movement, especially around joints,
- hyperpigmented or hypopigmented scars, when the color difference becomes the main problem.
Several key factors influence the final appearance of a scar. The deeper and more extensive the injury, the greater the risk of forming a wide, hard, or irregular scar. Also significant are: skin tension in the given area, delayed healing, wound infection, presence of a foreign body, tissue necrosis, and genetic predisposition to excessive fibrosis. Scars from lacerated wounds, crush injuries, and burns are particularly difficult because the trauma in them is uneven, and the tissue damage goes beyond what is visible at first glance. Medicine does not like chaos, and mechanical trauma usually leaves exactly that.
It is also worth remembering that a scar is a dynamic structure. In the first weeks and months after an injury, it can be red, tense, and hard, and only with time does it mature, fade, and partially soften. The remodeling process can last from a few months to even over a dozen months. Assessing a scar too early can therefore be misleading, but on the other hand, starting treatment too late is also a mistake. The best results are usually achieved when treatment is started at the right time and tailored to the type of scar, rather than to a trendy treatment slogan.
Post-accident scars - removal
The term “scar removal” is colloquial but medically imprecise. In most cases, it is not about the complete erasure of the scar, but about reducing its visibility, improving its structure, softening the tissue, leveling the surface, limiting symptoms and, when necessary, restoring the proper function of the area affected by the scar. This is important because promising a patient “skin like before the accident” usually has nothing to do with honest medicine.
Management depends on the type, age, and location of the scar. In the treatment of fresh hypertrophic scars and in the prevention of abnormal scarring, silicone preparations in the form of gels or patches are of fundamental importance, and in selected cases, also pressure therapy. These methods help maintain adequate hydration of the stratum corneum and influence scar remodeling. For active, itchy, painful, and growing scars, intralesional injections are also used, especially of corticosteroids, sometimes in combination therapies.
For uneven, thickened, or atrophic scars, treatments stimulating collagen remodeling are widely used. These primarily include:
- fractional laser therapy – causes controlled thermal micro-damage, stimulating the remodeling of scar tissue,
- microneedling – induces controlled reparative trauma and supports skin remodeling,
- microneedle radiofrequency – combines needling with heating the deeper layers of the skin, which can improve the structure and cohesion of the scar,
- medical peels – are sometimes used as an aid for superficial changes and accompanying pigmentation disorders.
In the case of post-traumatic scars, there is no single method that is good for everyone. An atrophic scar after an abrasion requires a different approach than a hard, hypertrophic scar after a laceration, and yet another for a contracture after a deep burn. Therefore, modern treatment is usually based on combined therapy. For example, first the activity and hardness of the scar are limited, then its texture and elasticity are improved, and finally, the color or minor irregularities are corrected. Such a staged approach is more rational than performing a series of random treatments in the hope that one will “catch.”
In some cases, procedural or surgical treatment is necessary, particularly when the scar:
- limits mobility,
- distorts surrounding tissues,
- causes significant skin tension,
- is very wide,
- does not respond to conservative treatment.
Surgical scar correction may involve its excision and a new, more precise wound closure, local plasty, or contracture release. Such a procedure does not “cancel” the problem but replaces an abnormal scar with a more functional and usually more aesthetic scar. Often, supplementary treatment, such as silicone therapy or laser procedures, is implemented only after surgical correction.
In aesthetic and dermatological practice, solutions available at Ambasada Urody are also used for the reduction of post-traumatic scars, such as fractional laser, laser scar removal, skin microneedling, microneedle radiofrequency, and procedures aimed at remodeling scars on the body. These methods are used to improve skin texture, reduce depressions, soften tissue, and limit the visibility of scars, but their selection should always depend on the type of scar and its stage of maturation.
Regardless of the chosen method, photoprotection is very important. Fresh and remodeling scars easily undergo permanent discoloration under the influence of UV radiation, which can worsen the treatment outcome more effectively than the injury itself. Sun protection doesn't sound spectacular, but in medicine, it is often the least spectacular things that make the biggest difference.

